Health Sciences News
College of Education professor aims to disrupt multiple sclerosis through pioneering research study
Auburn University College of Education professor Evelyn Hunter’s research is intended to cause disruption. After all, the word disrupt is literally in the name of her pioneering research study, which is focused on helping those with multiple sclerosis.
“We’re attempting to determine whether or not our social experiences or psychological health impact the levels of inflammatory markers,” said Hunter, an associate professor of counseling psychology in Auburn’s College of Education and a licensed psychologist who is leading the Disrupt MS study. “So, it helps us to more accurately pinpoint what types of experiences we might need to target in intervention so that we can disrupt the pathway to psychological distress and then perhaps limit the impact on the body.”
Just last year, Hunter’s Disrupt MS study was emboldened by an $850,000 philanthropic grant by the Bristol Myers Squibb Foundation to support research into health disparities in rural communities. Hunter said that while her study focuses on those with MS in rural areas, its findings also have the potential for even greater reach.
"Multiple sclerosis is what is considered a model chronic illness," Dr. Hunter explained. "We can use the knowledge that we gain from research with MS patients to apply to other types of illnesses."
Hunter said MS manifests differently in each individual, with symptoms ranging from vision issues to motor problems. Dr. Hunter's research focuses on how social experiences and psychological health influence inflammatory markers in MS patients. By pinpointing these influences, the study aims to develop interventions that can disrupt pathways to psychological distress, ultimately improving patient care. And the rural component of the work is important because she said MS patients in such locations face unique challenges.
"Our health is very much connected, and rural communities tend to have a lack of access to all of the things that make us healthier," Hunter said. "Managing a chronic illness like multiple sclerosis in rural communities can be more difficult than managing in urban environments or towns or cities that are more resource-intensive."
A second phase of the Disrupt MS study involves forming patient-provider coalitions, including psychologists, neurologists, and public health providers. This collaborative effort seeks to create psychological interventions tailored to MS care.
"We want providers to think about focusing on the whole person in MS care," Hunter said. "But we also want providers to be thinking about how we might apply the knowledge from this research to other forms of chronic illness, especially those forms of chronic illness where we see deep levels of disparities for different populations."
Hunter said her work aims to create good disruption, ultimately leading to a meaningful impact on healthcare.
"I get excited to think about the ways we might improve lives overall, and developing psychological interventions is something that can really improve the lives of individual patients,” she said. “And that’s exciting to be a part of.”

Evelyn Hunter (left), an associate professor in Auburn's College of Education, is pictured working in a lab. Hunter's Disrupt MS study is focused on those with MS in rural areas.
Categories: Health Sciences
Chen's work on nanomaterials in medicine featured in Science Coalition "Research Innovators" spotlight
Research by Pengyu Chen focused on nanomaterials in medicine is featured in the latest "Research Innovators" spotlight by The Science Coalition. Learn more here.
.jpg)
Pengyu Chen
Categories: Health Sciences, Engineering
Stress science event encourages collaboration across disciplines
Stress science researchers from across Auburn University came together at the Auburn Alumni Center recently for a one-day gathering to share ideas and research in a multidisciplinary environment. The April 8 event was part of Auburn's Team Science Series, which offers opportunities to connect and collaborate among researchers across disciplines.
A number of AU faculty members made presentations, including Ford Dyke, associate clinical professor in the School of Kinesiology and Director of Mindfulness@Auburn; Wendy Gordon, professor of human development and family science; and Danielle Wadsworth, professor of kinesiology.
Also included were Haruka Wada, associate professor of biological sciences; Robert Judd, Buris R. Boshell Endowed Chair and head of the Department of Anatomy, Physiology and Pharmacology in the College of Veterinary Medicine; Jennifer Robinson, professor of psychological sciences; and Rita Graze, associate professor of biological sciences.
"Stress involves a strain or pressure due to demanding circumstances and can result in both adaptive and maladaptive outcomes," according to Jennifer Kerpelman, associate vice president for research and one of the organizers of the event. "Auburn researchers across a number of disciplines study environmental, biological, psychological and social stress at the molecular level all the way to the community level in plants, animals and humans.
"This event offered a new opportunity for these researchers to connect, collaborate and create community across those disciplines," Kerpelman continued. "Participants gained valuable insights from experts on effectively securing research grants and were encouraged to share ideas for novel projects, discuss developing interdisciplinary collaborations and contemplate new ways to strengthen stress management efforts on campus and in the community."
"Across disciplines, Auburn researchers apply complementary approaches to conceptualize, measure and understand the effects and mechanisms of stress and stress responses," added Stephen Erath, associate dean and professor of human sciences and another event organizer.
"At the stress science event, we encouraged interdisciplinary conversations that will lead to collaborative proposals and projects addressing major stress science challenges. We will continue to facilitate conversations and collaborations among stress researchers with shared interests in the future."

Ford Dyke, associate clinical professor in the School of Kinesiology and director of Mindfulness@Auburn, speaks on stress management to attendees of the Team Science Series stress science event, April 8, 2025.
Categories: Health Sciences, Life Sciences
Turning pages, building bonds: The power of shared reading with babies
The ability to read is an essential and crucial life skill. In fact, you are currently displaying your literacy skills by reading this feature. Central to the recent data collected by researchers in Auburn University’s College of Human Sciences is the idea that consistent shared book reading between parents and their babies during the early developmental stages of life can bring with it several positive benefits.
Guided by theory, research and practice — along with cooperation by caregivers and in partnership with Alabama pediatric clinic partners — waves of data focusing on families’ experiences with shared book reading, parents’ mental health symptoms, parent-provider relationship quality and more were collected and thus, the Books and Babies studies were born.

The researcher spearheading the Books and Babies studies is Dr. Cynthia Frosch, associate professor of Human Development and Family Science (HDFS) at the College of Human Sciences, along with her graduate student research assistants, Olivia Martín-Piñón and Jamie Gensbauer. Sheila Sjolseth, a current HDFS doctoral student, and Kimberly Rogers, a graduate of the HDFS master’s degree program, were key contributors to the first wave of data collection for the study.
“Starting at birth, reading with children puts them on a path to success,” said Frosch. “I would say that it's never too early to begin sharing books with babies. Developing those routines can be a source of comfort, stability and familiarity for the parent-infant or caregiver-infant relationship. In addition, the benefits early literacy skills provide are far reaching. Children who hear more language and understand how books work have that advantage when they enter school.”
The first wave of the Books and Babies study was built on a theoretical framework to explore factors associated with shared book reading frequency including infant characteristics, parent/caregiver characteristics and social contextual factors. To bring this vision to life, Books and Babies 1.0 partnered with two Alabama pediatric clinics that are a part of the non-profit organization, Reach Out and Read.
Reach Out and Read was founded in 1989 to help families make reading a part of their routines and the organization serves as a critical partner in Auburn’s research. Part of Reach Out and Read’s strategic plan is to serve 10 million children by 2030 aiming to create a world where every family uses shared reading to build the bonds needed for their children’s health and future.
For the first wave of the Books and Babies study, data were collected in 2022 focusing on 70 parents of 4 and 6-month-old infants. Three different age-appropriate books along with three different posters that depict families reading with their babies were provided to clinics for clinic exam rooms. Families were also provided with a large magnet featuring the project logo and a message to “Share Books with Your Baby!’

Pictured is a sample magnet with the project logo provided to families.
During a pediatric well-child visit, a physician or nurse practitioner provided a selected book to the family and discussed the benefits of early shared reading. Parents or caregivers then had the option to scan a QR code sticker placed on the book taking them to the study conducted by Auburn researchers for data collection.
“We felt really good about the quality of data that we obtained, and this is where the clinics play a crucial role as research partners,” said Frosch.
Findings from that pilot study showed that 77% of parents or caregivers reported a high-quality relationship with their infant’s pediatrician and 57% of parents or caregivers reported being distracted by technology. This was important because the study’s pediatric clinic partners expressed an interest in understanding families’ technology use.
Interestingly, what affected shared book reading frequency the most was parents’ insurance type, mental health symptoms and perceptions of the parent-provider relationship.
“It's not just about early literacy. It's also about quality relationships,” said Frosch. “The quality of the relationship parents share with their pediatrician seems to matter for how frequently parents read with their babies.”
According to a recent U.S. Surgeon General’s Advisory on the Mental Health and Well-being of Parents, 41% of parents say that most days they are so stressed they cannot function and 48% say that most days their stress is completely overwhelming.
“Our research is starting to uncover how valuable parents’ mental health experiences like anxiety and depression can be for understanding book sharing practices.”
Dr. Cynthia Frosch
“Our research is starting to uncover how valuable parents’ mental health experiences like anxiety and depression can be for understanding book sharing practices,” said Frosch. “If your family is economically stressed and doesn’t have access to high quality, affordable childcare or if you're struggling with mental illness, that can create stress on families and add more burden. If you tell families to read more but they are facing these challenges, then that's not going to be supportive to families.”
Those factors were part of the focus of the Books and Babies 2.0 study in the summer of 2024 that doubled the number of Alabama Reach Out and Read Clinic partner sites to four total. The data collected focused on 173 caregivers.
Findings from the second study revealed that the top three needs expressed by families were access to healthy food, access to affordable childcare and access to educational opportunities for their children. Pediatric providers noted supports and resources for mental health as the top need for families. In addition, 94.7% of providers found that their clinic was either very successful or extremely successful when it came to meeting Reach Out and Read’s aims and 65% reported that the Books and Babies study posters added value to promote shared book reading with families.
The Books and Babies studies are made possible thanks to grant funding provided to the EARLY Lab by The Women’s Philanthropy Board at Auburn University. The EARLY Lab, housed within the Early Learning Center on Auburn’s main campus, focuses on early relational health, emphasizing caregiver-child relationships from birth through age 5 years. Through research and practice, EARLY’s goal is to reduce disparities in socioemotional health and early language and literacy development, while strengthening relationships within families.
“I think we have been good stewards of those funds, and we were really intentional,” said Frosch. “Between planning the two studies, collecting data, purchasing all the books, driving to the clinics, and buying custom book-shaped cookies for the pediatric providers to say thank you for their engagement, I feel really good about the work we did.”
As for the future, a third Books and Babies study is on the horizon. That study looks to expand recruitment while centering on family voice and asking new questions that focus on infant and parent sleep, parents’ feelings of judgement in the parental role and more.
"Being a part of Books and Babies allowed me to see the real stakes of my doctoral work,” said Martín-Piñón. “So much of research is behind the scenes, but with a project like Books and Babies, we can see the benefit our work has firsthand. Working in partnership with pediatricians was so impactful that it has inspired new directions for my future research, and that is what innovative higher education is all about: inspiring students and supporting the community that they serve."
Ultimately, the goal is to expand the reach of the study and promote early shared book reading within families as a tool to build strong relationships and to provide a foundation for lifelong literacy and learning.
“The most rewarding part of the project for me is the collaborative work with our clinic partners,” said Frosch. “That's been really neat, and I say to my students that at the end of the day, the worst-case scenario is we have gotten hundreds of books into the hands of families in communities throughout Alabama. That's a win-win. That is an outcome of the work that we have done where really no one loses.”

Categories: Health Sciences, Education, Graduate Student Research
Dogs and turtles: Kinesiology, forestry professors team up for research project
What do turtles, scent-trained dogs, and human movement have in common? A School of Kinesiology faculty member in Auburn University’s College of Education is using all three to conduct research. Associate Professor Heidi Kluess is launching a study that will implore dog owners to walk their pets – and collect data on box turtles in Alabama.
In a joint project with the College of Forestry, Wildlife and Environment, Kluess hopes dog owners and their dogs – human-dog citizen science teams – can use their daily walks to find box turtles for forestry researchers to collect data on the number of turtles in the state and their health conditions. While their findings will help researchers to learn more about turtles, the physical activity taking place will assist Kluess in her research on human behavior when walking with dogs.
“We want to study a person’s walking habits when there is a purpose for their exercise,” Kluess said. “We know when people walk with their dogs, they walk more. The idea is they are not only walking with their dog but they are also looking for turtles. So, will they walk more?”
Participants will track physical activity for six months, anywhere they would normally walk, while also collecting data for turtle research by taking photos of the turtles and noting their GPS location. College of Forestry, Wildlife, and Environment Research Assistant Professor Jean Fantle-Lepczyk will use the information to better understand common box turtle population dynamics.
“I am an amateur dog trainer and a conservation biologist by training,” Fantle-Lepczyk said. “This study is a great chance for me to marry my long-held interest in dog training, particularly in scent work, with my professional research interests as the wildlife biologist on the project.”
Kluess explained that the box turtle is not currently on the endangered species list, but could be, and scientists don’t know much about their distribution and where they are located.
“Our ultimate goal is to make this a bigger conservation effort with the turtles,” Kluess said. “One fun thing we will do with the turtles is use artificial intelligence to identify the turtles because they are actually identifiable by their shell. We’re hoping we would get the same turtle submitted more than once.”
Fantle-Lepczyk said one of the challenges in this sort of work is finding the same animals repeatedly to follow their fate.
“I am interested in learning more about the population dynamics of common box turtles across the southeast, particularly in comparing dynamics between natural and human-dominated landscapes,” Fantle-Lepczyk explained. “This project will provide a novel and innovative way of gathering this information.”
The initial training for the participating human-dog citizen science teams took place earlier this month, where dogs learned turtle odor and their owners learned about collecting needed data for the project, which is being funded initially by the Association of Professional Dog Trainers.
In approximately three months, the teams will come back for physical fitness testing on the humans and the dogs. They will repeat this again at the six-month mark.
“Most dogs experience the world through their nose so this is just giving them a focus and a purpose when they go on a walk,” Kluess said.

Heidi Kluess
Categories: Health Sciences, Life Sciences, Education
How the Gene Machine is fighting breast cancer across Alabama
The big pink bus that the Gene Machine once called home is hardly inconspicuous. If you’ve traveled Wire Road at any point over the last seven years, there’s a good chance you spotted the vibrant 2002 Ford Super Duty F-250 from the road, even if you weren’t aware of its connection to Auburn.
“Before joining the lab, I didn’t know what the Gene Machine was,” shared Sheniqua Glover ’18, a graduate student in the Gene Machine lab. “I’ve known a lot of students that recognize the bus and recognize the Gene Machine from the bus, but they don’t necessarily know what that means.”
The Gene Machine is the passion project of Nancy Merner, an associate professor and geneticist in the College of Veterinary Medicine. Kicking off in 2017 with the purchase of the big pink bus, the project’s Gene Machine travels across Alabama to examine the DNA of individuals diagnosed with breast cancer and other associated cancers.
Though it’s unclear who coined the term “Gene Machine,” the pink bus now synonymous with the project once served as both transportation and a mobile blood donation center. However, this changed in February 2023, when 279 donors generously gave during Tiger Giving Day and raised $26,445 for the project. This money went directly to funding Gene Machine Two, a Ford Escape Plug-in Hybrid SUV with detachable magnets for more covert home visits.
“Breast cancer is the most commonly diagnosed cancer in American women, besides skin cancer,” shared Merner. “One in eight women will be diagnosed with breast cancer in their lifetime, so that’s a 13% lifetime chance of developing a particular cancer.”
Many of the men and women that the Gene Machine comes across are surprised to learn that only 10% of breast cancers can be classified as hereditary, meaning caused by mutations in genes inherited from parents. This is because hereditary breast cancer must fit certain criteria, as outlined by the National Comprehensive Cancer Network.
This means that breast cancers—even in those with a family history of the disease—are not necessarily going to be the product of inherited genes. “Most breast cancers, they’re genetic,” said Merner,” but not anything that you got from your mom and dad. It’s mutations that are occurring in your cells over time. And then, as those mutations accumulate, that’s when it turns into cancer.”
“The fact that this can appear, regardless of and disconnected from family inheritance, is fascinating. And not something that I think the wider world knows,” said Narfunda Gibson Ross, a self-described “16-year thriving survivor” who was connected with the Gene Machine eight years after undergoing a double mastectomy and chemotherapy for Stage 2 ductal carcinoma breast cancer.
Ross’s sister, Jatunn Gibson, who served as an Auburn University assistant professor and extension specialist in Human Development and Family Studies from 2015–2024, also chose to pursue genetic screening, having been diagnosed with breast cancer six years after Ross.
At the time, both women were shocked to learn that their breast cancer diagnoses were not the product of inherited genes, despite their shared family history of breast cancer. These experiences highlight how little we currently understand about hereditary breast cancer—and how important it is that the Gene Machine project fills the gaps.

Merner clarified, “The issue is, if 100 women get genetic screening and they fit all these criteria for hereditary breast cancer, we’re only going to be able to solve maybe 30% of them with what we know today causes breast cancer. So that means that we have 70% of people that fit hereditary breast cancer criteria that we don’t know what the genetic cause is. That’s why research is so important.”
What Dogs Tell Us About Breast Cancer
Though people are often confused when they learn that the Gene Machine is stationed at Auburn’s College of Veterinary Medicine (rather than, say, the College of Human Sciences), it helps to visualize canines as a model of hereditary breast cancer. Through what’s known as comparative genomics, the mutations in the genomes of predominantly inbred dogs can be compared to the mutations in human genomes, and vice versa.
The Gene Machine is not alone in its mission. The Auburn University Research Initiative in Cancer (AURIC), an organization founded in 2012 to unite researchers against cancer, is likewise housed at the College of Veterinary Medicine.
“That [relationship] has everything to do with the World Health Organization’s One Health Initiative,” said Betsy Stallworth ’02, a registered nurse who serves as the project’s recruitment coordinator. “Humans, animals, and the earth are one health. We affect one another and can help one another.”

Stallworth is a major part of the project’s success across the state, contributing to a 60% increase in enrollment in 2024. Despite this growth, she maintains that the focus of the project is the person, not the numbers. “Behind every file of DNA on the screen is a human being. We’re trying to help families. We’re trying to help communities. We’re trying to help the world.”
When the pandemic hit in 2020, however, the Gene Machine team was forced to reformulate its approach. Reaching out to the Alabama Department of Public Health, Merner was granted access to the state’s cancer registry of potential participants, whom they began contacting over email and phone.
Reaching Out To Those In Need
More Than A Number
In 2022, the Gene Machine received a four-year research scholar grant from the American Cancer Society to identify and study the genome sequences of African American women who have hereditary breast cancer. The nearly $800,000 grant is validation not only for Merner’s team but also for those taking part in the research.
As an African American woman taking part in the study, Ross saw the Gene Machine as a positive response to the gaps in public healthcare. “When you go to the doctor, you almost feel like a number. You’re pushed through and you’re pushed out. With the Gene Machine, they have one focus, and that focus is on the gene and to study its actions.”
“We have to make a lot of effort so that other ethnic groups and underrepresented people who participate in research are no longer afraid,” said Merner. “They seem to ask, ‘If I’m giving you a piece of me, then what are you going to do with that?’”

“We just have high hopes that we’re going to make a discovery with all these efforts,” said Merner.
Though this level of medical mistrust is still present among her fellow cancer survivors, Ross believed that the Gene Machine team was working hard to assuage those concerns.
“I do see a hesitance in [survivors]. They’re not quite sure what the study is going to be because some of them still have it embedded in them about the Tuskegee Syphilis Study. They just shy away from it, [but] knowledge is rewarding. So if you know you have something, you can pass that along to someone else. You can save a life with it.”
Glover is thankful that she can help encourage participants who may be wary of the study’s intentions. “With me being African American, I can attest personally that [when you see] someone that looks like you, you receive it way better than seeing someone of another ethnicity telling you the exact same thing.”

It’s Personal
During enrollment events, the Gene Machine team makes a point of highlighting the confidentiality of the participants’ DNA samples and personal health information. The supercomputer that is used to store the team’s data is triple password-protected and inaccessible by the internet. All consent forms are also regulated and assessed by the Institutional Review Board.
Though Merner hopes to continue her journey toward making a high-impact genetic discovery and building a strong cohort of researchers, the goal of the Gene Machine remains the same as it was in 2017: to encourage men and women across Alabama to learn all they can about their own personal health.
“You might not think that we’re making a difference, but we are,” Merner said. “We have hundreds of genomes right now, and we’re aiming for thousands. We just have high hopes that we’re going to make a discovery with all these efforts.”
Whether it’s driving down the road in a hybrid SUV–or chugging along in a pink bus that gets nine miles to the gallon–the Gene Machine project is radically altering the future of breast cancer prevention. One gene at a time.

Nancy Merner is an associate professor in Auburn’s College of Veterinary Medicine.
Categories: Health Sciences
Nursing professor receives simulation research fellowship
Associate Clinical Professor Tiffani Chidume was selected to participate in a research fellowship of the International Nursing Association of Clinical Simulation and Learning (INACSL). The research fellowship is a twelve-month program designed to develop future leaders in simulation research.
The unique, web-based fellowship is comprised of monthly webinars with experts, extensive reading, and writing, with guidance on the best practices and processes of conducting simulation research. Fellows work on a research project, grant application, or research manuscript during the twelve-month period and are assigned an experienced mentor to guide them during the development of their project.
“I feel incredibly honored and fortunate to have been selected as an INACSL Research Fellow from such a competitive pool of applicants,” said Chidume. “This opportunity to participate in group sessions with esteemed peers and mentors, engage in interactive discussions led by prominent figures in simulation research, and receive guidance on my research projects is truly invaluable. I am grateful for the recognition of my work and excited to embark on this enriching fellowship experience with INACSL.”
According to Chidume, the research fellowship is significant for advancing knowledge in simulation education, allowing for sharing of cutting-edge ideas, collaboration, and mentorship from leaders. The interactive discussions which are specifically described as being "led by prominent figures in simulation research," suggest that the content will be at the forefront of advancing simulation education through research.
“The fellowship presents an invaluable opportunity for me to broaden the scope and impact of my simulation research. With the guidance and feedback from a dedicated mentor, I will be able to elevate the rigor and quality of my work, enabling me to advance to the next level as a researcher.
“Importantly, one of my key goals for this fellowship is to position myself for securing simulation-specific grants for AUCON. The insights and connections fostered through this program will be instrumental in identifying relevant funding opportunities and crafting compelling proposals that align with the latest advancements and priorities in the field. By leveraging the collective expertise of the cohort, I aim to develop innovative research projects that address critical gaps and contribute substantially to the growing body of knowledge in clinical simulation and learning. The INACSL Fellowship promises to be a transformative experience, equipping me with the necessary tools, networks, and guidance to expand the horizons of my simulation research while actively pursuing the financial support needed to execute high-impact studies that can shape the future of simulation education at AUCON.”
“The research fellowship is pivotal for the advancement of educational methods, patient safety, technological innovation, and professional development,” said Dr. Pao-Feng Tsai, associate dean for research at AUCON. “By fostering research, interdisciplinary collaboration, and leadership, the fellowship contributes significantly to improving practices and outcomes across the nursing fields that rely on simulation-based training and research.
“Simulation is an emerging trend in training essential skills and knowledge in nursing before students begin bedside practice. AUCON has one of the best simulation labs in Alabama. This fellowship award recognizes Dr. Chidume's excellence in simulation education and will provide mentorship support, enabling her to pursue future simulation research.”

Tiffani Chidume
Categories: Health Sciences
Pharmacy investigator receives NIH support to study kratom
For those going through the mental and physical stress of living with human immunodeficiency virus, or HIV, another challenge is how other substances, from medications, natural substances and illicit drugs can affect the therapies. The Harrison College of Pharmacy’s Angela Calderón is currently leading a study to investigate interactions between these therapies and the natural botanical kratom.
Titled “In vitro assessment of kratom pharmacokinetic CYP interactions with HIV ART drug metabolism,” and funded by the National Institute on Drug Abuse, the project will investigate the interactions between extracts of Mitragyna speciosa, also known as kratom, and certain HIV antiretroviral drugs that could affect the success of the HIV antiretroviral therapy.
“Individuals living with the stress of HIV are at increased risk of substance abuse, including abuse of natural substances, such as kratom, said Calderón. “This investigation will address the critical safety issue of botanical-HIV drug interactions as natural substances can alter therapeutic drug levels in the blood and thereby affect the safety and efficacy of HIV drugs.”
Calderón, Gilliland Professor in the Department of Drug Discovery and Development, is the principal investigator on the project, and is joined by co-investigators Richard Van Breemen, professor of pharmacology and pharmacognosy at the Oregon State University College of Pharmacy, and Satyanarayana Pondugula, professor of veterinary anatomy with the Auburn University College of Veterinary Medicine.
Kratom is a naturally-occurring botanical from the coffee family, primarily found in southeast Asia. Two of its compounds, mitragynine and 7-hydroxymitragynine, interact with opioid receptors in the brain and those that consume it report stimulant-like effects, as well as effects similar to those of opioids and sedatives.
Investigating the effects of kratom is important as the pharmacokinetic interactions caused by it can affect enzymes and drug transporters and can either enhance the toxicity of a therapy or reduce its efficacy. Specifically, regarding HIV antiretroviral therapies, it is known that opioids can decrease their efficacy, so it is important to learn more about kratom because of its opioid-like effects.
“When an opioid-like recreational drug such as kratom is introduced, botanical-drug interactions can occur that interfere with the efficacy of these established interventions, since the majority of antiretroviral therapy drugs are metabolized by the same cytochrome P450 pathways that metabolize opioids,” said Calderón. “Furthermore, since opioids usually decrease the efficacy of these regimens and increase toxicity, adverse drug events ensue and a serious and significant gap remains in our understanding of the these botanical-drug interactions.”
Deaths attributed to interactions between kratom and other drugs have been reported around the country. This study is innovative in that it is the first of its kind to investigate interactions between kratom and HIV antiretroviral therapy drug regimens.
Calderón and her team ultimately hope to provide evidence to guide the safe and naturally accompanying use of kratom with these drugs.
“Understanding the significance of this and other potential pharmacokinetic interactions with kratom is essential for ensuring the safe and effective use of antiretroviral therapy,” said Calderón. “By enabling the fundamental understanding of interactions between HIV drugs and kratom constituents, this project will provide a rationale for confirmatory clinical trials and ultimately, an improved efficacy of HIV treatment protocols.”

Angela Calderón
Categories: Health Sciences
Auburn researcher aims to help prevent, control avian influenza
Since 2022, avian flu — a rapidly circulating Influenza Type A virus — has affected over 81 million poultry, as well as the industries that depend on them. In Alabama alone, poultry generates more than 80,000 jobs and $15 billion in revenue.
In the past two years, a disease-causing strain of avian flu, known as H5N1, has impacted 1,046 flocks across the United States. Miria Criado, an assistant professor in Auburn’s College of Veterinary Medicine, is tackling this timely topic by investigating how these influenza viruses evolve and examining approaches to reducing their deadly impact on poultry.
“This work is focused on understanding how avian influenza circulates between species, how the virus evolves to continue circulating and how the bird’s immune system responds to the virus,” Criado said. “We are especially interested in how we can use some currently available tools or vaccines to help control these outbreaks.”
To advance this avian flu research, Criado received a grant from the U.S. Department of Agriculture (USDA), U.S. National Poultry Research Center for approximately $644,000 per year. This non-assistance cooperative agreement, which is a renewable grant for up to four years and $2.5 million, is a collaboration between the USDA and Auburn University. Criado, the lead principal investigator, is collaborating with Auburn Assistant Professor Constantinos Kyriakis, Erica Spackman, acting research lead within the USDA’s Exotic & Emerging Avian Viral Diseases Research and David Suarez, acting USDA laboratory director.
THE BASICS OF BIRD FLU
Poultry are susceptible to two different kinds of avian flu: low-pathogenicity (LPAI) and high-pathogenicity (HPAI). LPAI can cause a variety of mild symptoms or none at all, said Criado. In contrast, HPAI strains typically lead to the death of the birds within two days.
In all of Criado’s research at Auburn, she is working with LPAI.
“There’s so many questions that we can answer using LPAI strains,” she said. “It’s a great opportunity to study avian flu in a very safe way.”
Criado’s research will allow her to better understand how LPAI strains are circulating among poultry and provide insights for future studies involving HPAI: a key goal given that HPAI is spreading rapidly.
“Two years ago, we only had around 40 HPAIV outbreaks reported,” Criado said. “In the last few years, we have had thousands of outbreaks. Almost all continents around the world had detections.”
This high transmission of HPAI can quickly decimate a flock, and several biosecurity measures and quarantine need to be in place for the affected poultry premise.
“One of the reasons this new strain is concerning is because the amount of virus you need to infect a bird is really, really low compared to previous strains that were circulating,” Criado said.
The virus has a surprisingly simple structure for its detrimental impacts. Criado said a virus is genetic material surrounded by a protein coat and an additional layer with surface proteins.
“If you think about a virus as a ball, then imagine there are all of these surface proteins attached to the outside of the ball,” she said. “You may have one influenza virus strain with a square green protein or a rounded red one.”
These surface proteins seek to bind to a bird’s cells. Once the protein latches onto the cell, the virus releases its genetic material into the cell and hijacks its normal operations. The virus’ genetic material — RNA in the case of bird flu — becomes the cell’s instruction guide, causing it to produce more of the virus.
The bird’s body may respond by producing certain proteins, known as antibodies, which adopt different tactics depending on the situation. For example, an antibody may block one of the virus’s surface proteins from latching to the bird’s cell.
But this tactic may only ward the virus off for so long; viruses are adept at adapting.
“This virus mutates a lot, especially in these surface proteins,” Criado said. “When this evolution happens, it can be difficult for the antibody to defend the bird from the virus.”
BRIDGING BASIC, APPLIED SCIENCE AT AUBURN
Criado is churning out basic science insights in the laboratory that can lead to improved approaches for reducing the impact of avian flu. She is studying poultry cells in a flask to better understand how the virus evolves and interacts with poultry immune cells, known as host cells.
“You can look at the genome of the virus and compare it to old or current strains to try to figure out if there is evolution,” she said. “We are especially interested in understanding how the surface proteins may change and interact with the host.”
For example, perhaps a certain segment of the virus’ genetic information is more susceptible to mutations. If Criado can pinpoint this segment of genetic material and determine what it encodes, she would be armed with more insight when developing applied solutions.
“Our work could help explain a pattern where a specific protein tends to evolve,” she said. “Maybe we can use a vaccine later to target that surface protein that can be more effective than what we’ve been using nowadays.”
Moving forward, Criado plans to conduct poultry studies using LPAI virus and vaccines through extensively vetted protocols. Through this work, she aims to develop recommendations that can help curb the deadly impact and spread of avian flu, as well as provide insights about counter-measures that can be implemented at facilities and farms to help control the spread of avian flu.
As Criado conducts her grant-funded research, she is leveraging her extensive expertise. She has previously investigated how LPAI and HPAI viruses replicate and transmit in different avian species. She also has studied vaccines for avian flu, including a recent peer-reviewed publication where she and her coauthors found that multivalent vaccines could protect chickens against avian flu and other important viral infections that affect poultry.
Across her basic and applied work, Criado’s multi-pronged research has the potential to positively impact poultry, humans and the environment. While avian flu is rare in humans, Criado hopes her research can help the scientific community be ahead of the curve if the disease were to become widespread beyond birds.
“My work is rooted in the OneHealth concept that the health of people is closely connected to the health of animals and our shared environment,” Criado said. “Long-term, we hope our research leads to practical tools, recommendations and intervention strategies to reduce avian flu’s impact, especially in poultry.”

Miria Criado candles eggs to observe the growth and development of chicken embryos. (Photo credit: Molly Bartels)
Categories: Health Sciences, Agriculture
Prolific patent portfolio earns mechanical engineering professor NAI Fellow status
Auburn University has yet another National Academy of Inventors (NAI) Fellow.
Mehmet Arik, associate professor of mechanical engineering, was recently tapped for the professional honor (widely recognized as the most prestigious awarded to academic inventors) on the strength of more than 120 issued patents with a broad range of applications in medical systems, energy systems, aviation systems and photonics technologies.
Already an American Society of Mechanical Engineers (ASME) Fellow, Arik says his latest distinction means even more.
"Being an NAI Fellow is even more of a joy for me because it shows that collaborative work always pays off," Arik said. "I developed my patents with many colleagues from academia and industry and I truly enjoy collaborating with researchers and engineers across many fields."
Arik came to Auburn in 2022 after 11 years as a faculty researcher at Özyeğin University in Istanbul, Turkey. He began his professional career at General Electric (GE) Global Research Center in 2000 as a senior engineer working on research and technology development programs related to energy, aviation, medical, industrial systems and lighting industries. The electronics thermal management group he organized conducted award-winning research for both GE and government organizations such as the Department of Energy, Defense Advanced Research Projects Agency and the National Institute of Standards and Technology. While at GE, Arik created a suite of respected intellectual property built on innovations benefitting multiple industries while building an exceptionally robust portfolio of scholarly contributions to more than 75.
It was his patent portfolio, however, that earned him nominations from multiple NAI Fellows.
"Many of my patents went into practice in industry in many different product segments, which I'm very proud of," Arik said. "Those inventions already have social and economic impact as well as environmental benefits. While publishing extensively can be very satisfying, patents have a different value in science and technology."
A patent in which Arik takes particular pride is a novel cooling approach that has been instrumental in many modern LED lighting applications. But the most meaningful may be his system for measuring junction temperature of photonics devices.
"That was very special for me because I developed it with my undergraduate and graduate students while I was in Turkey," Arik said. "It was so hard to get a USPTO (United States Patent and Trademark Office) patent from Turkey but young minds helped make it happen."
The same can be said for his latest patent disclosure, which was developed last year with one of his current graduate students.
"Being named an NAI Fellow is yet another testament to the impact of Dr. Arik's work," said Mario Eden, dean of engineering. "But the collaborative spirit that drives his research is, I think, as impressive as the innovations that have earned him this distinction."
Arik believes the prestige stemming from the NAI's recognition will enable even more opportunities for invention and development, both individually and collaboratively.
"I want to be an ambassador for innovation and entrepreneurship within the communities I belong to," he said. "Auburn is, of course, top of that list. I want to help young students, fellow faculty and researchers to develop intellectual property that truly makes an impact."
Arik is Auburn’s eighth NAI fellow. Previous honorees include J. David Irwin, Joseph W. Kloepper, John Weete, S.D. “Dave” Worley, Bruce Tatarchuk, Vitaly Vodyanoy and Fa Foster Dai. Dai, Irwin and Tatarchuck are all engineering faculty.
Media Contact: Jeremy Henderson, jdh0123@auburn.edu, 334-844-3591

Mehmet Arik
Categories: Health Sciences, Energy & the Environment, Transportation, Engineering, Economic Development
Computer science and software engineering researcher part of $1.8 million NIH study to pioneer platform for the analysis of single-cell data
Tin Nguyen is pioneering a new platform for the analysis of single-cell data through the creation of an easy-to-use web interface through software programs designed in his laboratory.
Nguyen, an associate professor in computer science and software engineering and director of Auburn University’s Bioinformatics Lab, is a co-investigator on a $1.8 million National Institute of Health award granted to the bioinformatics company AdvaitaBio. This research will 1) accurately identify cell types and composition in complex tissues, 2) infer cell developmental stages and pseudo-time trajectories, and 3) identify cell-type-specific pathways and punitive mechanisms in phenotype comparisons. Auburn University’s portion of the grant is $813,000.
The study, “A web-based platform for robust single-cell analysis, bulk data deconvolution and system-level analysis,” co-authored by Nguyen in collaboration with AdvaitaBio’s researchers, will provide new methodologies for single-cell analysis that far exceed current technologies.
“A special feature of this software is that it will be able to analyze very large datasets,” Nguyen said. “Imagine that the data has a million cells, which can be very difficult for any software to analyze. But this software will be able to analyze extremely-large-scale data. Second, it can also infer cellular development for multiple sets of cells and cell types. Being able to follow the developmental evolution of each cell will allow for important advances in areas such as cancer research.
AdvaitaBio is the leader in the interpretation of high-throughput biomedical data including variant interpretation, pathway analysis, disease subtype discovery and integration across multiple data types. Currently, nine of the top 10 pharma companies rely on Advaita’s state-of-the-art algorithms to solve complex problems. Advaita provides a suite of advanced analysis software to more than 13,000 registered users worldwide: iPathwayGuide, for functional interpretation of genes and proteins; iVariantGuide, for genetic variant analysis; iKnowledgeBase, a collection of knowledge and pre-analyzed data from various phenotypes, and iBioGuide, a search engine revealing connections between genes, pathways, SNPs, drugs, and more.
“Our preliminary work shows that single-cell analysis and cellular deconvolution can achieve an outstanding accuracy of approximately 90 to 100 percent if we properly utilize reference single-cell datasets and pathway knowledge” said AdvaitaBio CEO Dr. Sorin Draghici.
Nguyen added that data from single cells can be used to analyze any disease, the source of the diseases, down to the muscles and blood vessels.
“This project is very interesting to me because I’m happy that some of the academic work we do here can be translated into the health industry, where it can be useful and help save lives,” Nguyen said.
Media Contact: Joe McAdory, jem0040@auburn.edu, 334.844.3447

Tin Nguyen
Categories: Health Sciences, Engineering
Auburn research center renamed with renewed focus on neuroimaging
A major research center within Auburn’s Samuel Ginn College of Engineering has been renamed the Auburn University Neuroimaging Center to highlight its renewed focus on solving critical neurological health challenges.
The center — headquartered in the Thomas Walter MRI Research Building in the Auburn Research Park — is focused on advancing the latest in neuroscience research and leveraging the university’s expertise in engineering, sciences and veterinary medicine with the use of advanced magnetic resonance imaging.
On Friday, members of the Auburn University Board of Trustees watched a video that touted the center’s capabilities.
“Our vision is to become a leading center for MRI research with emphasis on brain imaging, cardiovascular imaging, orthopedic imaging and coil design,” said Thomas Denney, director of the Auburn University Neuroimaging Center and the Mr. & Mrs. Bruce Donnellan & Family Endowed Professor in electrical and computer engineering. “These areas represent an intersection between the needs of the MRI research community and existing expertise and strengths of Auburn University.”
The center will allow the university to expand its groundbreaking brain research, among other capabilities, through the MRI devices at the site and the academic and research prowess of Auburn faculty.
“I dreamed of building an MRI research program here at Auburn where large medical centers recognize our contributions,” Denney said. “Through research, Auburn University has moved the needle and more than exceeded my expectations. Since opening this building, we’ve been able to double our staff. Those (MRI) machines are great, but people are the ones who write research papers and people are the ones who earn those research grants. The university is sitting on a gold mine in terms of data and capabilities.”
Approximately 90 percent of the images processed at the center focus on the brain.
“The neuroimaging center is a blessing to my practice and to our student-athletes because we literally use it on a daily basis, including the weekend,” said Michael Goodlett, chief medical officer and team physician for Auburn Athletics. “It gets us back to play quicker because not all injuries are surgical, and this definitely helps us determine very quickly in the course what’s surgical and what’s not surgical.”
Jennifer Robinson, professor of psychological sciences, said her research work also has benefited greatly from the center.
“I’m particularly focused on the interaction between cognition and emotion,” she said. “So, disorders like post-traumatic stress disorder are of great interest to me. And then also just knowing how much that can help our soldiers and folks that have experienced PTSD.”
New research explorations already underway include, but are not limited to:
- Meredith Reid, assistant professor in electrical and computer engineering, who is exploring post-traumatic stress disorder biomarkers in senior adults via spectroscopy.
- Adil Bashir, associate professor in electrical and computer engineering, who is studying muscle and brain energy production capacity on the cells and determining mitochondrial metabolic homeostasis by utilization of phosphorus spectroscopy.
- Gopikrishna Deshpande, professor in electrical and computer engineering, who is examining how artificial intelligence can be used to predict brain disorders and human/animal behavior using information from brain networks obtained from MRI.
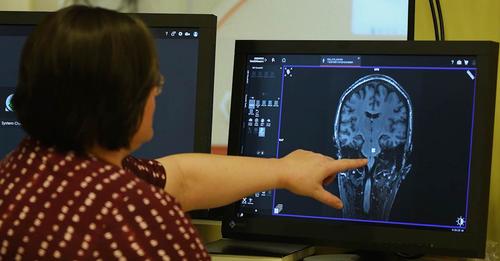
Meredith Reid, assistant professor in electrical and computer engineering, is exploring post-traumatic stress disorder biomarkers in senior adults via spectroscopy.
Categories: Health Sciences, Engineering
Piazza leading pharmacy’s innovative Cancer Research Center at Auburn University
For most academic scientists conducting biomedical research, the possibility of advancing a new medicine from the lab to the clinic is, at best, an aspiration. Despite the odds, Gary Piazza and his research team in the Auburn University Harrison College of Pharmacy (HCOP) have discovered a highly potent and selective anticancer treatment and are collaborating with investigators at the University of Alabama-Birmingham (UAB) O’Neal Comprehensive Cancer Center to advance a new drug candidate to clinical trials for patients with the most fatal of cancers.
Piazza joined HCOP in 2021 as the W.W. Walker Professor and head of the Department of Drug Discovery and Development. A highly respected cancer investigator, Piazza came to Auburn as a UAB graduate with more than 35 years of research experience, including 10 years as a professor at the University of South Alabama Mitchell Cancer Institute in Mobile and 10 years as a principal scientist with Southern Research in Birmingham.
Along with his administrative responsibilities, Piazza continues his groundbreaking research as director of the newly created Cancer Research Center at HCOP.
A team of scientists who started to collaborate while at Southern Research also made the move from MCI to Auburn, including Xi Chen, a medicinal chemist; Adam Keeton, a cancer biologist; Yulia Maxuitenko, a pharmacologist; and Kristy Berry, a lab manager with expertise in mouse tumor models.
Join Auburn’s research efforts
“We share a common interest in cancer research but have very different skill sets,” said Piazza. “Having a multidisciplinary team with diverse scientific expertise has allowed us to solve many technical problems as we seek to advance our experimental drugs to the clinic.”

Gary Piazza
Categories: Health Sciences
Auburn’s College of Veterinary Medicine hosts 14th annual Boshell Diabetes and Metabolic Diseases Research Day
Auburn University’s College of Veterinary Medicine will host the 14th annual Boshell Diabetes and Metabolic Diseases Research Day on Friday, April 28, at the Auburn-Opelika Marriott Resort at Grand National.
“Here at Auburn, we are attacking this disease from all sides from the laboratory through a variety of clinical studies,” said Robert Judd, director of the Boshell Research Program and professor of pharmacology in the College of Veterinary Medicine’s Department of Anatomy, Physiology and Pharmacology. “Research Day is an exciting opportunity for us to bring researchers and medical professionals together to share and discuss information about diabetes, obesity and their treatments.”
The annual Boshell Research Day event brings together experts from around the U.S. to present current topics related to diabetes and the role of obesity in its development. The meeting is highlighted by research presentations throughout the day and evening.
This year’s guest speakers include Vishwa Deep Dixit, the Waldemar Von Zedtwitz Professor of Pathology, Immunology and Comparative Medicine and director, Yale School of Medicine Center for Research on Aging; Jonathan D. Schertzer, an associate professor of biochemistry and biomedical sciences, Farncombe Family Digestive Health Research Institute Centre for Metabolism, Ontario, Canada; and Dr. Regina Benjamin, former U.S. Surgeon General and founder of the BayouClinic.
Registration and additional information are available now at www.vetmed.auburn.edu/boshell. The event is free for Boshell program members, students and postdoctoral fellows and $125 for non-members. Registration is open through April 19, and the deadline for abstraction submission is March 31.

Auburn University’s College of Veterinary Medicine will host the 14th annual Boshell Diabetes and Metabolic Diseases Research Day on Friday, April 28, at the Auburn-Opelika Marriott Resort at Grand National. Pictured: Robert Judd
Categories: Health Sciences, External Engagement, Life Sciences
Auburn researcher finds olive oil to improve brain health, memory in individuals with mild cognitive impairment
Extra virgin olive oil may have positive effects on individuals with mild cognitive impairment, according to a recently completed study by Amal Kaddoumi in Auburn University’s Harrison College of Pharmacy. Her findings, recently published in the journal “Nutrients,” suggest compounds found in olive oil impact brain health and improve the blood-brain barrier.
Kaddoumi, a professor in the college’s Department of Drug Discovery and Development, utilized 25 participants experiencing mild cognitive impairment in her study that included consuming 30 milliliters, or about three tablespoons, of olive oil per day for six months. Thirteen participants consumed extra virgin olive oil, or EVOO, and 12 consumed refined olive oil, or ROO. EVOO is rich in phenols, a class of organic compounds containing a hydroxyl group and a benzene ring, while the ROO has been purified of phenols.
“The participants were subjected to several tests before and after olive oil consumption, including MRI scans, a battery of cognitive tests and blood analysis for biomarkers related to Alzheimer’s disease,” said Kaddoumi. “Our findings showed that EVOO and ROO improved cognitive function as determined by the improved clinical dementia rating and other behavioral scores.
“Interestingly, the MRI scans results were not the same between EVOO and ROO. While EVOO enhanced the blood-brain barrier function and the functional connectivity between different brain areas, ROO increased the functional brain activation to a memory task in brain regions involved in cognition.”
The blood-brain barrier and its permeability are key indicators in her study. A network of blood vessels and tissue made up of closely spaced cells, the blood-brain barrier plays a vital role in maintaining a healthy brain by protecting the brain from exposure to blood-related neurotoxins and in the clearance of brain waste products. A functional blood-brain barrier is vital for a healthy brain.
“Regarding blood biomarkers, our findings showed that EVOO and ROO altered two major biomarkers related to Alzheimer’s disease, namely, beta-amyloid and tau phosphorylation, suggesting EVOO and ROO changed the processing and clearance of beta-amyloid,” said Kaddoumi. “These alterations collectively could have played role in improving the blood-brain barrier and improving function and memory.”
The results are consistent with Kaddoumi’s pre-clinical findings conducted in mouse models of Alzheimer’s disease. The pilot study on individuals with mild cognitive impairment is the first to look at what directly happens to the brain in humans when consuming olive oil.
“While we need additional studies to understand the mechanisms by which olive oil exerted such effects in humans, findings from our preclinical studies in the mouse models of Alzheimer’s disease showed that EVOO alleviated several pathological hallmarks of Alzheimer’s disease,” said Kaddoumi.
One surprising finding from the study was the results of the control group. The beneficial compounds found in olive oil are more prevalent in the unrefined EVOO, but those in the refined group saw improvement as well.
“We used ROO as the control or placebo group because it lacks the phenolic compounds in EVOO,” said Kaddoumi. “However, based on the findings from this pilot study, ROO could also provide health benefits suggesting the positive impact of oleic acid, the primary monounsaturated fat present in both EVOO and ROO, which could contribute to the observed effect. Indeed, additional studies are necessary to confirm these results.”
Even with the need for further studies, Kaddoumi is excited to see the results from her pilot study and what it could mean for those living with Alzheimer’s, dementia and other cognitive issues.
“These results are exciting because they support the health benefits of olive oil against Alzheimer’s disease,” said Kaddoumi. “Based on the findings of this study and previous pre-clinical studies by us and others, we can conclude that adding olive oil to our diet could maintain a healthy brain and improve memory function.”
While the study used participants experiencing mild cognitive impairment, Kaddoumi says next steps include a larger clinical trial that includes cognitively normal individuals. With the surprising results from the refined olive oil, she also envisions a trial with a variety of grades of olive oil.
“The research team and I would like to acknowledge and thank the project participants and relatives, without whom this research would have not been possible,” said Kaddoumi.
The pilot study and research were a collaborative effort among a variety of Auburn University units and outside organizations. Kaddoumi led the project, including conceptualization, methodology, data curation and supervision.
Collaborators from Auburn included the MRI Research Center, the Department of Psychological Sciences in the College of Liberal Arts and the Department of Pathobiology in the College of Veterinary Medicine. Others included the Edward Via College of Osteopathic Medicine-Auburn campus, Yale School of Public Health and the Alzheimer’s Center at Temple University.
This research was also funded by Auburn University Presidential Awards for Interdisciplinary Research.

Professor Amal Kaddoumi recently completed a study that found extra virgin olive oil may have positive effects on individuals with mild cognitive impairment.
Categories: Health Sciences
Auburn University, Tuskegee University create partnership to include research, academics, community engagement around health inequities
Auburn University and Tuskegee University initiated a Memorandum of Understanding, or MOU, to expand partnerships between the universities and collaborate on community outreach at a special signing ceremony on Monday afternoon.
The MOU is a commitment to blend resources and intellectual capacity to address racial and health disparities in communities across the state of Alabama. Through faculty research and outreach collaborations, both universities will work to address lack of health care access and other social and health inequities in the local areas.
“This partnership with Tuskegee University is a win-win for everyone, especially our students, researchers and outreach team,” Auburn University President Christopher B. Roberts said. “As a land-grant institution, it is important to work to eliminate disparities that limit opportunities for those in underserved areas. I am confident the collaboration that will emerge from this agreement will benefit students from both universities, as well as our neighboring communities.”
The agreement is the latest in a number of partnerships between Auburn and Tuskegee, and with the two universities united in a shared mission, the future is bright for all involved.
“This partnership demonstrates the capacity of our shared land-grant missions to improve the quality of life for Alabama’s citizens,” Auburn University Interim Provost Vini Nathan said. “Both institutions maintain a longstanding commitment to addressing health disparities across our state. Through these collaborations, we are bringing together our faculty, staff, students and programs to benefit our communities directly.”
The collaboration includes a 10-member committee to review and recommend proposals to the university presidents for prioritization in seeking state and federal support. The collaboration team will focus on academic programs, research and development, outreach and community engagement.
“The impact of this partnership will benefit the students of both schools and the surrounding communities where we are based,” Tuskegee Provost S. Keith Hargrove said. “By blending our resources, we will be able to have a broader reach in developing state-of-the-art academic programs and research and development opportunities, while deepening our community engagement and outreach.”
The MOU signifies a commitment to forge institutional resources and intellectual capacity to address racial and health disparities in communities across the state. With the understanding that communities of color lack adequate access to healthcare and other social determinates of health impact areas, Auburn and Tuskegee will address these issues through ongoing faculty research and outreach alliances.
“As we focus on innovative ways to expose our students to research and training opportunities to keep them in the forefront of their fields, partnering with Auburn University helps expand their experience,” Tuskegee President Charlotte P. Morris said. “This collaboration provides a formal structure to ensure that the common goals are met to support students of both institutions and partner with the community in meaningful ways.”

Auburn University President Christopher B. Roberts and Tuskegee University President Charlotte P. Morris signed a Memorandum of Understanding that will benefit the state of Alabama for years to come. (Photo by Stefan Smith/Tuskegee University)
Categories: Health Sciences, External Engagement
Auburn professor receives American Cancer Society grant to continue breast cancer research
Nancy Merner, assistant professor in the Auburn University College of Veterinary Medicine’s Department of Pathobiology, recently received a $791,808 grant from the American Cancer Society to continue her research into identifying and studying genetic factors associated with hereditary breast cancer in the African American community.
“African American women have higher breast cancer incidence rates before the age of 40 than other ethnic groups in the United States,” Merner said. “They are also more likely to be diagnosed with triple-negative breast cancer, a more aggressive subtype with a poor prognosis. These facts, coupled with reports of African American males having higher breast and prostate cancer frequencies than other ethnicities, suggest that hereditary factors are involved.”
Despite the higher incidence of these cancers in the African American community, Merner said there have been an insufficient number of studies to determine the causes.
In efforts to combat this insufficiency, the Merner research team has sought out families with a history of such cancers while traveling the state, spreading cancer awareness in a pink bus called the “Gene Machine” and using online resources.
“There is a critical need to identify and study genetic factors associated with African American hereditary breast cancer,” Merner explained. “Our group has established the Alabama Hereditary Cancer Cohort for genetic analyses. Alabama is a severely medically underserved state, with double the national percentage of African Americans. Therefore, we developed strategic recruitment protocols to break down research participation barriers to recruit African American hereditary breast cancer cases and families effectively.”
Utilizing data gathered from those participants and others, Merner and her team have conducted gene sequencing and identified protein-truncating variants, or PTVs, specific to African Americans that appear to increase inherited breast cancer risk. PTVs are genetic variants that shorten the protein-coding sequence of genes and may cause them to malfunction.
“We plan to identify these PTVs associated with breast cancer among African Americans and study how they increase risk,” Merner said. “The impact of this work will be substantial for this understudied and underrepresented group. Risk variant identification can lead to better risk assessment and tailored therapies, reducing breast cancer-related deaths.”
“Ultimately, this study will not only identify African American breast cancer risk variants, but generating and sharing this data on African American hereditary breast cancer cases will add to the limited resources currently impeding discoveries. And finally, by carrying out sub-type analyses, this proposal could specifically impact women diagnosed with triple-negative breast cancer, reducing the number of deaths from this aggressive breast cancer sub-type through better risk assessment and tailored therapies.”

Nany Merner and the "Gene Machine"
Categories: Health Sciences
Professor emeritus publishes book on sociology of mental health
A new book by L. Allen Furr, professor emeritus of sociology, explores sociology’s key contributions to the understanding of mental health, providing a counterpoint to the medical approach to the subject.
The Sociology of Mental Health and Illness, published by Sage Publishing in June 2022, uses both micro and macro-level theories to understand the social aspects of mental health and illness. The book shows the subjective nature of mental illness and systems of diagnosis and treatment. It also emphasizes how social conditions and relationships create life pathways toward mental health and psychological struggles and uses the concept of "patient career" to describe how individuals interact with mental health professionals. In addition, the text explores the connections between mental health and social problems such as terrorism, substance abuse, criminal violence, suicide and domestic violence.
Furr’s research focuses on the sociology of health, with a particular interest in mental health. Much of his work has investigated the psychosocial dynamics of facial disfigurement. He was part of the University of Louisville’s research team that pioneered facial transplantation. His work can be found in journals in psychiatry, medicine, nursing, social work, as well as sociology. Furr was awarded a Fulbright Scholarship to teach at Punjabi University in Patiala, India, and is currently on the Fulbright Specialist Roster.

Allen Furr
Categories: Health Sciences
Progress in the fight against GM1: Auburn research providing hope for children with deadly disease
Jojo is experiencing life like most 13-year-old girls: staying up later, watching movies, shopping and baking cookies. And now she has more liberty, but it’s a different kind of freedom.
She uses a walker, but she and her family see it as freedom, a remarkable accomplishment compared to her six months of not being able to walk prior to receiving a gene therapy treatment for her rare disease.
Jojo has GM1 gangliosidosis—an inherited disorder that progressively destroys nerve cells in the brain and spinal cord and is estimated to occur in one in 100,000 to 200,000 newborns. But her mother sees steady improvement in Jojo, who was the first child to participate in a clinical trial that has its origin in Auburn University research.
“Jojo was very ill when she was treated with gene therapy in 2019. She had great trouble swallowing and eating, and she wasn’t able to walk,” said Jojo’s mother, a family practice physician in Los Angeles. “Since treatment, Jojo eats normally and is at a normal weight for her age. She still has some challenges, but she’s made great improvements in many ways.”
The trial’s gene therapy treatment was created at Auburn’s College of Veterinary Medicine, where scientists for several decades have researched treatments to improve and extend the lives of cats affected by GM1 gangliosidosis.
GM1 gangliosidosis is caused by mutations in a gene known as GLB1, thus impairing production of the enzyme, beta-galactosidase. The treatment, administered intravenously, delivers a functional copy of the GLB1 gene that improves the enzyme activity, leading to improved neuromuscular function.
Auburn worked with the University of Massachusetts Medical School and the National Institutes of Health to move the research into helping children suffering from the disease. In 2019, Jojo became the first child to receive the one-dose treatment at NIH in Bethesda, Maryland.
“We had hoped to stop the disease’s progression, but she is showing real signs of improvement,” said Dr. Doug Martin, director of Auburn’s Scott-Ritchey Research Center in the College of Veterinary Medicine and a professor in the Department of Anatomy, Physiology and Pharmacology.
He says the treatment is very promising because it has worked well in GM1 mice and cats and is delivered by a single IV injection that takes less than an hour.
“As this trial and new trials progress, and as more patients are treated, we'll have a good idea of whether the gene therapy helps children as much as it has helped the animals,” he said. “This is certainly what we're hoping for.”
Martin says the NIH trial, which includes 11 children, is the first of three trials underway.
“Jojo actually was part of a sort of ‘pre-clinical’ trial at NIH,” Martin said. “Her condition was so poor at first that she was not qualified for the actual trial, but now she has improved enough with treatment that she would qualify.”
Clinical trials are being conducted also at the University of California-Irvine, which is using a spinal fluid injection, and one at the University of Pennsylvania, Martin said.
“Our research at Auburn has shown that GM1 in cats can be treated, so we are fortunate more institutions are seeing the possibility of moving it into cures for children.”
Martin and his fellow Auburn researchers are moving forward with additional research as well, hoping to add to the knowledge base for GM1 and the related GM2 disease, called Tay Sachs. They are testing higher doses of the treatment to help cats with GM1 and are checking the toxicity and clinical effects.
“This will provide valuable information to veterinarians and human physicians as we fight these diseases,” he said. “Additionally, because there are similarities in the pathology of GM1 gangliosidosis and Alzheimer’s disease, it is possible that the same platform being used for GM1 could someday be used to treat Alzheimer’s.”
For GM2, Auburn is testing a new generation of vector to be administered intravenously or in the spinal fluid. The current treatment for GM2 is given by an injection into the brain, but researchers are seeking a less invasive method.
History of Auburn’s GM1 research
Martin is leading Auburn’s effort, which was started by his mentor, Professor Emeritus Henry Baker, in the 1970s. To move the treatment toward human medicine, Martin developed a partnership with UMass Medical School researchers Drs. Miguel Sena-Esteves and Heather Gray-Edwards, an Auburn graduate, and they have worked collaboratively for 15 years, combining animal and human medicine studies to treat rare diseases that affect both animals and humans.
For Auburn graduates Sara and Michael Heatherly of Opelika, Alabama, whose son Porter was the first known case of GM1 in Alabama and died in 2016, the knowledge of a treatment is one of mixed emotions.
"We are excited to know there is hope for the future of children diagnosed with GM1,” Michael Heatherly said. “We are thankful for everyone who has dedicated their time, resources and careers to move this treatment forward.
“We understood early on the research would not help Porter, but we wanted to help spread the word of the research and the progress that was being made.”
Parents of a child with GM1 each carry one copy of the mutated gene, but they typically do not show signs and symptoms of the condition.
To honor Porter and his family—who held fundraisers for several years to support Auburn’s research—the Scott-Ritchey Research Center incorporated Porter’s likeness in a creative identity for the center.
Donations to help fund Auburn’s research into GM1 can be made online.
BY CHARLES MARTIN

Since receiving gene therapy treatment, Jojo is able to enjoy many of the simple pleasures of life.
Categories: Health Sciences
Auburn researcher works to improve capabilities for Brain-Computer Interface
Supported by a $175,000 grant from the National Science Foundation, or NSF, a researcher in Auburn University’s College of Sciences and Mathematics is working to improve the capabilities of Brain-Computer Interface, or BCI, an advancement that has wide potential for helping people with severe motor impairments, detecting and diagnosing health issues and providing new interfaces for gaming and other uses.
Jingyi “Ginny” Zheng, an assistant professor in the Department of Mathematics and Statistics, received her award from the NSF’s Division of Computing and Communication Foundations for her project “Towards A Manifold-based Framework for the Brain-Computer Interface.”
“We are working to improve the current statistical framework upon which BCI operates using a new measurement to quantify the differences in the connectivity of the human brain,” Zheng said.
BCI as a technology has existed for a number of years, Zheng says. However, it is limited in its current functionality by its mathematical framework.
“The current measurement used in BCI for quantifying the differences in brain connectivity is not robust and is inefficient,” Zheng said. “We are seeking to upgrade the BCI system by developing a statistical framework using a new mathematical measure for quantifying the differences in brain connectivity matrices.”
BCI works by linking the human brain to a mini computer. The user wears a special headset that picks up brain waves and transmits them to a computer-based recording device. This mini computer translates the human brain wave — essentially a thought — into a mechanical response.
“For example, a severely motor impaired person confined to a wheelchair, could operate and maneuver their chair by thought process using a BCI device,” Zheng said. “Over the past decades, numerous methods have been implemented in BCIs to decode and translate brain signals. However, BCIs still suffer from low robustness and low reliability as they are sensitive to artifacts, noise, outliers and require a long calibration process.”
Zheng’s research aims at constructing a manifold-based framework that will improve the robustness of BCI technologies and expand practical applications. The project is funded through 2024 and Zheng said, once BCI capabilities are enhanced, the technology has potential not only in the health and medical fields, but also in biology, neuroscience, agriculture, remote sensing, computer vision and other areas.
Zheng joined Auburn’s faculty in 2019. Her research interests are in areas of data science, machine learning and data-driven computing. She also teaches several statistics courses in the College of Sciences and Mathematics.
BY MITCH EMMONS

Jingyi “Ginny” Zheng
Categories: Health Sciences
Auburn showcases variety of university-developed technologies at BIO Alabama conference
Auburn University recently participated in the BIO Alabama conference at the Grand Bohemian Hotel in Mountain Brook, showcasing seven of its biotechnology research developments.
BIO Alabama is the trade organization for the state’s biosciences industry. This year’s event—the first meeting following a six-year hiatus due in part to the COVID-19 pandemic—featured approximately 200 scientists and their research developments April 25-26.
Melinda Richter, global head of Innovation at Johnson & Johnson, served as keynote speaker under this year’s theme, “Building Alabama’s Biohorizons,” focusing on the future of the industry’s participation in Alabama’s innovation economy.
Auburn’s presentations included:
-
Vivosphere cell encapsulation technology platform for drug development and discovery (Elizabeth Lipke; presented by co-inventor Yuan Tian) – This is a 3D cell encapsulation method and device for more accurate and cost-effective drug screening, bioinks and regenerative medicine.
-
Anti-cancer immunotherapy targeting CD47 (James Gillespie, joint project with VCOM) – Development of an anticancer treatment that could replace immunomodulatory therapies targeting CD47.
-
Computational tool for speeding discovery of natural beneficial compounds (Angela Calderon and Cheryl Seals; presented by Kabre Heck and Muhammad Gulfam) – A collaborative project about an automated method to analyze mass spectrometry data to identify potential bioactive compounds in complex mixtures.
-
Engineered bacteria for producing biofuels and other compounds (Yi Wang) – Engineering of bacteria to express record levels of butanol for biofuel or other industrial applications or to express record levels of butyl acetate for use in foods, consumer goods or industrial processes.
-
Computationally designed compounds for treating Alzheimer’s disease (Raj Amin; presented by Ian Steinke and Fajar Wibowo) – A custom-designed therapeutic compound for treating Alzheimer’s without the side effects seen with other drugs in this class.
-
Gene therapy vectors for therapeutic treatment of neurological disease (Doug Martin) – Engineered AAV vectors for treating neurological diseases such as rabies.
-
Medical device for improving diagnosis and monitoring of neuropathy in diabetic patients (Michael Zabala and Thomas Burch; presented by co-inventor Kenny Brock, VCOM) – A medical device for accurately monitoring and measuring loss of feeling in diabetic patients. (Jon Commander is also a co-inventor and is with VCOM.)
BIO Alabama is the leading advocate for Alabama's bioeconomy. The organization represents the state on a national and international stage, promoting the intellectual and innovative capital to make Alabama a premier place to invest, start and grow in bioscience.
Alabama’s bioscience industry provides a $7.3 billion impact on the state’s economy, according to BIO Alabama data. Auburn has participated in BIO Alabama events for a number of years.
"As presenting sponsor for this year’s BIO Alabama conference, Auburn University had an important opportunity to showcase some of our latest technologies during a reverse-pitch session to industry,” said Bill Dean, executive director of the Auburn Research and Technology Foundation.
“Auburn’s participation in events like the BIO Alabama conference speaks to our role in growing the region’s bioeconomy and demonstrates our commitment to the bio-sector in the form of industry collaboration and partnerships that will advance research and impact quality of life throughout the state.”
BY MITCH EMMONS

Liz Smith, College of Agriculture academic advisor, works at Auburn’s booth during the BIO Alabama conference. She talked with companies about opportunities for applied biotechnology graduates.
Categories: Health Sciences, Energy & the Environment, Food Systems, Engineering, Life Sciences, Manufacturing, Agriculture
Auburn psychology researcher seeking to improve treatment options for alcohol use disorder
Statistics suggest that more than half of the adult population in the United States reports regular use of alcohol, with nearly a quarter of the population reporting that they suffer from problematic drinking. A researcher in Auburn University’s Department of Psychological Sciences in the College of Liberal Arts is exploring ways to improve and expand the available treatment options for those suffering from Alcohol Use Disorder, or AUD.
Samantha Fede, a neuroscientist, has a background in the study of cognition, brain and behavior. She came to Auburn last fall from the National Institutes of Health, or NIH, in Bethesda, Maryland. She brought with her a nearly $250,000 NIH-funded research program that has as its core objective the treatment of AUD using Transcranial Magnetic Stimulation, or TMS, and MRI neurofeedback.
Alcohol misuse costs about $249 billion every year, Fede writes in her research abstract. Much of this cost is related to negative consequences of alcohol use.
There is an established relationship between excessive alcohol use and crime commission, financial difficulties, intimate partner aggression, poor work performance and homicide. In fact, according to a Bureau of Justice Statistics study, 3 percent of violent criminals report being under the influence of alcohol at the time of their offense, and more than 50,000 additional individuals are convicted of DUI/DWI and alcohol-related public order offenses per year.
“My background is mostly working with people who have been incarcerated or who have been in trouble in other ways due to the effects of AUD,” Fede said. “I am interested in better understanding this disorder and developing more and better tools for reducing harm associated with substance use.”
Fede’s research is a two-pronged study.
“Part one uses TMS to stimulate brain response with magnetic fields to alter alcohol cue response,” Fede said. “The second part of this research uses TMS in combination with another intervention, real-time fMRI neurofeedback, to provide reinforcement of healthier brain activity and to evaluate whether the two can create long-term improvements in people with AUD.”
Fede explains that TMS already is an FDA-approved method for treating depression; however, its use in treating AUD remains a mostly unexplored area.
Initial evidence suggests that interventions such as TMS that target neurocircuitry have promise for AUD treatment, Fede writes in her abstract. However, there remains a critical need to leverage neurostimulation techniques toward a sustained decrease in problem drinking and related antisocial and aggressive behaviors. The ultimate objective in this research is to identify a neuroscientific intervention that works to decrease alcohol drinking and antisocial behavior in individuals with AUD.
Fede’s research is funded through 2025. She currently is working with students in the pilot phase to establish the research methods and process. The second phase is projected to begin this summer, working with persons seeking treatment for AUD.
“In my previous work, we wanted to establish the methods and process for neurofeedback only,” Fede said. “In the current phase, here at Auburn, we are developing a TMS approach to change neural responses associated with negative drinking outcomes. In the second phase, we’re evaluating whether these two tools help patients to control those neural responses and change negative behaviors after they’ve left the lab and they’re not actively receiving treatment.”
Fede said it is important to recognize that AUD is a medical disorder and that people who misuse alcohol or suffer from AUD should not be stigmatized. Stigma often prevents people from seeking help and receiving high-quality treatment.
“AUD is a disorder that afflicts many people to varying degrees of severity,” Fede said. “It is associated with many negative outcomes, including sometimes antisocial and aggressive behaviors. Through this research, we are going to show that these negative outcomes have a neurobiological basis and that it can be changed through intervention. That way, we can improve understanding of the disorder and give people with AUD more tools to improve their lives and those around them through better treatment options.”
BY MITCH EMMONS

Samantha Fede, a researcher in Auburn University’s Department of Psychological Sciences in the College of Liberal Arts, is exploring ways to improve and expand the available treatment options for those suffering from alcohol use disorder.
Categories: Health Sciences
Aerospace engineering study encourages face mask redesign in the future
The COVID-19 pandemic brought about the use of face masks as a means of reducing the airborne transmission of diseases to the center of attention of people around the world. Researchers in aerospace engineering at Auburn University's Samuel Ginn College of Engineering are leading a study that will help improve our understanding of the science that can be expected to guide the design and use of masks in different situations and environments moving forward.
Their research has found that while basic surgical masks offer a first line of defense to both the wearer and the people around them, they are not foolproof as flow leakage occurs around the mask and their effectiveness under realistic coughing conditions is not known.
Assistant Professor Vrishank Raghav, Sarah Morris, a postdoctoral research fellow, and William McAtee, a graduate research assistant, found that repetitive ‘pulsatile’ coughs allow expiratory particles to escape through a surgical mask’s sides and above the nose in their co-authored paper, “Influence of expiratory flow pulsatility on the effectiveness of a surgical mask.”
Smoke from Gloria, a mannequin designed by Auburn's Applied Fluids Research Group, shows where basic surgical mask leakage can occur during a cough.
The study – part of a $464,846 National Science Foundation grant in collaboration with the University of Michigan funded in 2021 – was published as an invited article by the Journal of Exposure Science & Environmental Epidemiology, a Nature publication.
“Our research has found that if you are wearing a mask and you cough, the volume of air that leaks is reduced compared to not wearing a mask,” Morris said.
“However, the effect of pulsatility does influence the leakage volume and must be considered when this is modelled.”
Raghav said the source of the problem with basic surgical masks — the blue devices most-commonly sold to and used by the public during the COVID-19 pandemic — is pre-loosening as inhaling, exhaling, double, or even triple coughs provide gaps for germs to become airborne.
Laser imaging and high-speed photography were utilized to show mask leakage during simulated coughs on the top of the mask, above, and the sides of the mask, below.
“The main reason why surgical masks move, and open gaps, is because the air you are breathing in and out cannot easily travel through the tiny pores of the mask,” said Raghav, a recent NSF CAREER Award recipient. “Instead, it slowly pushes the mask out of the way and when you cough, air finds the path of least resistance out of the mask, which is outside the cheeks and above the nose.”
Raghav agreed that masks of higher quality than basic surgical masks can, if worn correctly, provide better protection. “Surgical masks allow significantly more protection than wearing no mask at all, cutting out roughly 85 percent of the expiratory flow,” he said. “Of course, N95s fit tighter, are secure and allow only a fraction of expired air to leak. Further innovations will be required before surgical masks are as effective as N95s.”
Raghav, Morris and McAtee utilized laser imaging, high-speed photography and a coughing simulator to determine surgical mask leakage. This wasn’t any coughing simulator. It was a custom-built mannequin named Gloria – decked out in a blue surgical mask – designed within Auburn’s Applied Fluids Research Group laboratory.
Using the device, a computer-controlled solenoid valve provides desired air flow rates by controlling a pressurized air source at the wall. From there, a pipe ‘throat’ inserted through the mannequin allows air flow from the wall to a one-inch diameter mouth, which is met by the surgical mask.
“We have a computerized control valve that opens and closes to let the air in and out. We control the pulsatility of the air,” Morris said. “We can create a single pulse, a double pulse, or a triple pulse.”
Two main techniques are used to make leakage measurements – flow visualization and particle image velocimetry. With flow visualization – the long pipe carries smoke with two-micron fog particles. When the mannequin coughs, smoke will follow the flow field. A Nikon mirrorless camera is used to capture the expiratory flow — leakage made visible by smoke.
Particle image velocimetry is where laser imaging comes into play.
“This is a quantitative measurement technique where we have these tiny, two-micron particles (representing leaked air) that follow the flow, and we are taking high-speed photos of them,” Morris said. “If we take images at pre-determined times apart, we can actually see where those particles are moving between image one and image two.”
A pulsed, high-speed laser combined with a laser arm and light sheet generating optics illuminates the 2D field of view, providing revealing imagery.
Though mask mandates have currently evaporated in many locations, Raghav pointed out that masks can continue to be useful in many settings.
BY JOE McADORY
Media Contact: Joe McAdory, jem0040@auburn.edu, 334.844.3447

Researchers, from left, William McAtee, assistant professor Vrishank Raghav, and Sarah Morris, used 'Gloria', a mannequin created by the Applied Fluids Research Group, to serve as a pulsatile coughing simulator.
Categories: Health Sciences, Engineering, Manufacturing
Auburn’s Boshell diabetes research program brings together faculty in fight against deadly disease
As America recognizes National Diabetes Month in November, Auburn University scientists are devoted year-round to researching this debilitating disease that affects one in 10 Americans.
Auburn’s Boshell Diabetes and Metabolic Diseases Research Program has 54 faculty members from 10 academic units across campus researching causes and treatments for diabetes and obesity-related health issues, principally focusing on the cardiac, neurological and metabolic aspects.
“We have excellent faculty seeking to improving the lives of all people with type 1 and type 2 diabetes,” said Professor Robert Judd, chair of the Boshell program and head of the Department of Anatomy, Physiology and Pharmacology in the College of Veterinary Medicine. “Our research will help people and pets, as dogs and cats can suffer from diabetes.”
Diabetes and obesity are associated with serious health conditions, including hypertension, coronary heart disease, stroke, non-alcoholic fatty liver disease, certain types of cancer, Alzheimer’s disease, asthma and musculoskeletal disease.
“We have strong interdisciplinary collaborations among professors who are researching the prevention, cure and management of diabetes and its complications,” Judd said. “We actively work together at Auburn and with faculty at other institutions to study the parallel epidemics of obesity and diabetes.”
Auburn’s program was established in 2001 through an endowment from the Birmingham-based Diabetes Trust Fund in honor of its founder, Dr. Buris R. Boshell, a 1947 graduate of Auburn, then Alabama Polytechnic Institute.
According to 2020 statistics from the Centers for Disease Control and Prevention, more than 34 million Americans have diabetes. Another 88 million adults are prediabetic, pushing the total number of those in danger of being afflicted with the disease to more than 122 million, or nearly one in every three people.
Examples of Auburn’s diabetes research include:
Rajesh Amin, Associate Professor, Drug Discovery and Development, Harrison School of Pharmacy
Amin’s research is focused upon drug discovery for metabolic-related diseases, including energy dysregulation associated with Alzheimer’s disease and liver disease. He has also teamed up with Feng Li and Tom Denney of Auburn’s MRI Center for developing novel targeted delivery of compounds to hepatic stellate cells for mitigating liver fibrosis.
Chris Easley, Professor, Department of Chemistry and Biochemistry, College of Sciences and Mathematics
Easley is leading a research team seeking to enhance biological measuring capabilities to better understand diabetes, heart disease and obesity. They are developing high-tech devices that could measure insulin or other hormones, like glucagon, in real time as a person takes insulin or a diabetes drug. The team is specifically studying how fat responds to stimuli like food or drugs, how fat secretes hormones and how that happens on a dynamic, short-time scale.
Emily Graff, Assistant Professor, Department of Pathobiology, College of Veterinary Medicine
Graff’s lab is looking at ways to help obese cats and humans. She says there are many similarities between human and feline obesity, such as insulin resistance, hepatic steatosis (fatty liver), reduced life span and cancer. There are distinct differences between cats and humans, as well. For example, cats do not develop clinical atherosclerosis associated with metabolic syndrome, which contributes to heart disease and stroke and is a major cause of mortality in people.
Michael Greene, Associate Professor, Department of Nutrition, Dietetics and Hospitality Management, College of Human Sciences; director, Metabolic Phenotyping Laboratory
Greene’s research is focused on metabolic diseases associated with obesity, including liver disease and colon cancer. The work in his laboratory spans from performing whole-body metabolism studies to RNA sequencing analysis. He is also collaborating with Elizabeth Lipke, professor in the Department of Chemical Engineering, to develop new models, such as 3D-engineered tissue cultures, to examine the link between obesity/prediabetes and colon cancer.
Ramesh Jeganathan, Professor, Department of Nutrition, Dietetics and Hospitality Management, College of Human Sciences
Jeganathan’s research is focused on investigating the molecular links between type 2 diabetes and Alzheimer’s disease, emphasizing aspects that have potential clinical significance. His lab explores genes, molecules and cellular processes that could cause and promote Alzheimer’s disease in type 2 diabetes patients. The aim is to discover novel agents to disrupt the connection.
Robert Judd, Professor, Department of Anatomy, Physiology and Pharmacology, College of Veterinary Medicine
Judd’s research is focused on the impact of obesity on adipose tissue physiology and how this newly recognized endocrine organ becomes dysfunctional during obesity development. In collaborative studies with Amol Suryawanshi of the College of Veterinary Medicine and Joseph Brewer of the Edward Via College of Osteopathic Medicine, Judd is expanding his research into the immunology of adipose tissue. Doug White of the College of Human Sciences is also studying adipose tissue physiology, looking at the role of leptin in type 1 diabetes.
Amarjit Mishra, Assistant Professor, Department of Pathobiology, College of Veterinary Medicine
Mishra aims to understand more about the regulatory pathways involved in airway inflammation. The Laboratory of Lung Inflammation, led by Mishra, is also interested in metabolic cues that coordinate immune cell activation and differentiation. Learning more about the link between obesity, inflammation and asthma is important for developing novel therapeutic treatments to prevent and treat asthma in people with obesity.
Ya-Xiong Tao, Professor, Department of Anatomy, Physiology and Pharmacology, College of Veterinary Medicine
Tao is studying naturally occurring mutations in two receptors expressed in the brain, melanocortin-3 and melanocortin-4 receptors. Both are involved in regulating energy homeostasis, with the melanocortin-3 receptor regulating fat storage and the melanocortin-4 receptor regulating both food intake and energy expenditure. His studies are seeking a better understanding of obesity from a genetic standpoint and potential therapeutics of monogenic obesity.
Geetha Thangiah, Associate Professor, Department of Nutrition, Dietetics and Hospitality Management, College of Human Sciences
Thangiah is studying disparities in childhood obesity between African Americans and the white population, with the long-term goal of improving the health of minorities by identifying appropriate interventions. The incidence of childhood obesity varies widely among races/ethnicity, with higher rates in African Americans (24%), making it one of the most profound disparities. Thangiah is looking at how socioeconomic status might influence eating habits, diet, parental beliefs, oxidative stress, microbiome and epigenetics.
The Boshell program also hosts an annual Boshell Research Day that brings in fellow researchers from around the country to share their research and develop new collaborations.
“We held our 13th annual event in September, with more than 175 scientists and supporters participating,” Judd said.
Financial donations to help support the Boshell Diabetes and Metabolic Diseases Research Program can be made online. The program also has the Jim Fyffe Diabetes Research Fund that helps support graduate students conducting diabetes research projects. Fyffe was a longtime Auburn football announcer who died in 2003 due to complications from diabetes. Information about both funds is available by contacting the College of Veterinary Medicine Advancement Office at giving@vetmed.auburn.edu or 334-844-1446.
Help support the Boshell Diabetes and Metabolic Diseases Research Program
BY CHARLES MARTIN

Robert Judd, chair of Auburn’s Boshell Diabetes and Metabolic Diseases Research Program, displays a blood glucose meter.
Categories: Health Sciences
Auburn University’s Boshell Research Day set for Sept. 17, features experts on diabetes, obesity
Auburn University’s 13th annual Boshell Research Day, scheduled for Sept. 17 at the Marriott Resort at Grand National in Opelika, Alabama, will bring together experts from around the U.S. to discuss current topics related to diabetes and the role of obesity in its development.
This year’s program will feature addresses from world-renowned speakers, including Dr. James G. Granneman, professor of molecular medicine, genetics and internal medicine and director of the Center for Integrative Metabolic and Endocrine Research, Wayne State University School of Medicine; Dr. Clayton E. Mathews, Sebastian Family Professor for Diabetes Research, University of Florida; and Ellen Gustafson, businessperson, social entrepreneur, sustainable food system activist, author and co-founder of FEED Projects and 30 Project.
In addition to these featured speakers, participants will attend both oral and poster presentations and have opportunities to network with fellow conference attendees.
Faculty from Auburn’s College of Veterinary Medicine and nine other colleges and schools across the university campus will join Boshell Research Day participants from the University of Alabama at Birmingham and Georgia State University for the one-day symposium.
The Boshell Diabetes and Metabolic Diseases Research Program, which aims to improve life for all people with diabetes, was established in 2001 through an endowment from the Diabetes Trust Fund in honor of its founder, Dr. Buris R. Boshell, a 1947 graduate of Auburn University, then Alabama Polytechnic Institute.
Through research focused on the prevention, cure and management of diabetes and its complications, Boshell researchers address many facets of both type 1 and 2 diabetes. Currently, more than 55 investigators from 10 different academic units across the Auburn campus hold Boshell membership and are actively involved in diabetes research, principally focused on the cardiac, neurological and metabolic aspects of the disease.
Dr. Robert Judd, chair of Auburn’s Boshell Diabetes and Metabolic Diseases Research Program and department head and professor in the Department of Anatomy, Physiology and Pharmacology, advances the Boshell mission of expanding and enhancing cross-disciplinary research opportunities, both on Auburn’s campus and at other institutions.
“We are attacking this disease from all directions through a variety of basic and clinical studies,” Judd said. “Research Day provides an important opportunity for us to bring together researchers and medical professionals from across the U.S. to discuss diabetes, obesity and their treatments.”
Registration for the 13th annual Boshell Research Day is now open. The conference is open to the public at a cost of $125 for all non-Boshell member attendees and no charge for current students, postdoctoral fellows and Boshell members.
Judd said Auburn is committed to providing the safest experience possible for all conference participants. To support this commitment, the university has implemented an indoor mask mandate, requiring all students, faculty, staff, visitors and event participants, including speakers, regardless of vaccination status, to wear face coverings when inside university buildings and while attending indoor events, except while dining or in private offices.
In addition to the university’s mask mandate, attendees are asked to self-monitor for COVID-19 symptoms, and, if symptoms are present, to stay home and contact their physician. Attendees should practice physical distancing when possible and sanitize their hands often.
For more information or to register for Boshell Research Day, visit the website at www.aub.ie/diabetes or email Judd at juddrob@auburn.edu.
BY JAYNE HART

The 13th annual Boshell Research Day is scheduled for Sept. 17 at the Marriott Resort at Grand National in Opelika, Alabama. The photograph is from a previous Boshell Research Day prior to the COVID-19 pandemic; this year, masks are required indoors at the event.
Categories: Health Sciences
New Auburn University internal awards programs name winners for 2021
Auburn University launched two new pilot internal awards programs in 2021 and has named the program’s first recipients.
The Research Support Program, or RSP, and the Creative Work and Social Impact Scholarship Funding Program, or CWSI, were established by the Office of the Vice President for Research and Economic Development. Both programs provide a competitive internal funding source to support faculty and to provide an opportunity for them to experience a small-scale pilot and refine their projects before competing for larger awards.
“This is a pilot version of a larger intramural award program,” said Bob Holm, associate director of Proposal Services and Faculty Support, the unit that administers the programs. “It enables faculty to participate in a competitive funding program and make improvements to their projects before a commitment to a long-term award program is made. The pilot provides a platform to test what works and what does not.”
The RSP is intended to be an annual cycle funding program to foster the development and growth of innovative and transformational research activities. It builds on faculty expertise, stimulates interdisciplinary collaborations and strengthens seed research activities. It is a strategically focused Auburn investment that promotes promising and impactful new lines of research as well as the growth of collaborative and interdisciplinary teams to build the foundations of science, to overcome scientific and societal challenges and to promote and enhance the quality of life and wellbeing of individuals, groups and communities.
The CWSIS funding program fosters innovation and discovery and builds faculty reputation and competitiveness. Examples of prestigious recognition for CWSIS include: the McArthur Genius Award, the Gates Foundation Award, appointment to the National Council on the Humanities or the National Council on the Arts and an NSF Senior Advisor for Public Access. Disciplines associated with CWSIS include design and the arts, humanities and applicable areas within business, education, social sciences and health and well-being.
As a form of research, creative work poses questions and searches for the answers through iterative processes that demand intellectual rigor and hard work. Related scholarship narrates, analyzes and evaluates the production and products of creative work, or proposes new and innovative approaches to that work, including interdisciplinary collaborations and explorations. The goals of creative work and scholarship are ultimately tied to making significant contributions to a meaningful and dignified quality of life.
Social impact scholarship involves research that is specifically aimed at societal challenges and values both theoretical and applied domains to produce core knowledge and address persistent and complex issues to create a better world and improve the lives of all individuals. Research in this domain often engages a diversity of stakeholders with the goal of bringing beneficial effects and valuable changes to the economy, society, education, public policy, health and quality of life.
This year’s recipients are:
Research Support Program
Brian Albanese, College of Liberal Arts, $24,999.34; “Neurobehavioral sensitivity to negative reinforcement in suicide”;
Benjamin Bush, College of Architecture, Design and Construction, $24,987; “EX4C: Next Generation Blood and Vaccine Transport for Combat, Austere and Challenging Environments”; co-investigators: Lorenzo Cremaschi, Samuel Ginn College of Engineering; Joellen Sefton, College of Education; David Crumbley, School of Nursing;
Nathaniel Hardy, College of Agriculture, $25,000, “The Evolution of Virulence in Xylella fastidiosa”; co-investigator: Leonardo De La Fuente, College of Agriculture;
Amal Khalil Kaddoumi, Harrison School of Pharmacy, $25,000; “Amylin role in Alzheimer’s disease”; Co-Investigator: Ahmed Hamid, College of Sciences and Mathematics;
Peng Li, Samuel Ginn College of Engineering, $25,000, “Probing Novel Quantum Phases in van der Waals Magnet Fe5GeTe2”; co-investigators: Masoud Mahjouri-Samani, Samuel Ginn College of Engineering; Wencan Jin, College of Sciences and Mathematics;
Panagiotis Mistriotis, Samuel Ginn College of Engineering, $25,000; “Bioengineering tools to uncover the mechanisms of human mesenchymal stem cell migration”;
Kristina Neely, College of Education, $25,000; “Inhibitory Motor Control in Adults with ADHD,” co-investigator: William Murrah, College of Education;
Janna Willoughby, School of Forestry and Wildlife Sciences, $24,998; “How do environmental and genetic effects interact to determine individual fitness?”; co-investigators: Avril Harder, School of Forestry and Wildlife Sciences; Lana Narine, School of Forestry and Wildlife Sciences; Kelly Dunning, School of Forestry and Wildlife Sciences.
Creative Work and Social Impact Scholarship Funding Program
Junshan Liu, College of Architecture, Design and Construction, $20,000; “Digitally Preserving and Re-presenting Alabama’s Rosenwald Schools”; co-investigators: Gorham Bird, College of Architecture, Design and Construction; Richard Burt, College of Architecture, Design and Construction;
Alicia Powers, College of Human Sciences, $19,191.92; “A clinical-community pediatric wellness initiative to manage and prevent cardiometabolic diseases in children with limited resources in Alabama”; co-investigators: Jeanna Sewell, Harrison School of Pharmacy; Felicia Tuggle, College of Liberal Arts, Sarah Watts, School of Nursing.
More information about these and other funding support programs supported by the AU Office of the Vice President for Research and Economic Development can be found by clicking here.
BY MITCH EMMONS
Categories: Health Sciences, Energy & the Environment, Food Systems, Engineering, External Engagement, OVPRED, Creative Scholarship, Life Sciences, Agriculture
Study finds bundling RFID with electronic data interchange increases hospital efficiency, reduces expenses
The National Academy of Medicine estimated the U.S. healthcare system wastes an average of $765 billion per year on misplaced or expired supplies.
Research published in Production and Operations Management “The Joint Use of RFID and EDI: Implications for Hospital Performance,” which included authors Kang Bok Lee, EBSCO Associate Professor of Business Analytics at the Harbert College of Business at Auburn University, and Harbert College alum Randy V. Bradley, who is currently Associate Professor in Supply Chain Management at the Haslam College of Business at the University of Tennessee, reveals a key strategy for hospitals to track equipment and supplies and increase performance, while reducing personnel expenses and readmission rates.
Specifically, the research shows the bundling of radio frequency identification (RFID) with electronic data interchange (EDI) provides a streamlined, all-in-one, technological database that yields greater organizational efficiency. RFID is the use of radio-frequency identification methods to tag and track items while electronic data interchange enhances visibility and communication through the use of electronically transferring information between organizations.Research published in Production and Operations Management “The Joint Use of RFID and EDI: Implications for Hospital Performance,” which included authors Kang Bok Lee, EBSCO Associate Professor of Business Analytics at the Harbert College of Business at Auburn University, and Harbert College alum Randy V. Bradley, who is currently Associate Professor in Supply Chain Management at the Haslam College of Business at the University of Tennessee, reveals a key strategy for hospitals to track equipment and supplies and increase performance, while reducing personnel expenses and readmission rates.
The best way to understand the benefits is to picture the technologies as bookends around the revenue cycle. RFID sits at the front end, where it can be used to track supplies and equipment. The result is a clean record of resource utilization in care delivery, which is useful on the backend when hospitals transmit claims to government and private insurance payers via EDI.
After examining 3,300 hospitals nationwide, the researchers conducting this study realized RFID/EDI bundles that capture the utilization of supplies, resources, and equipment at the point of care both aids in inventory visibility and creates a clean data stream that facilitates more efficient billing of third parties.
With an organized inventory and streamlined billing process, researchers believe this not only improves an organization’s bottom line by reducing expenditures, but overall patient care as well. Ensuring supplies are readily available – not misplaced – and tracked in real time, facilitates faster diagnostics and ensures timely medical interventions. These factors increase both the efficiency and expediency in which care can be delivered.After examining 3,300 hospitals nationwide, the researchers conducting this study realized RFID/EDI bundles that capture the utilization of supplies, resources, and equipment at the point of care both aids in inventory visibility and creates a clean data stream that facilitates more efficient billing of third parties.
Value-Based Purchasing, a federal program, recently shifted hospital reimbursements to a value-based model, placing a stronger emphasis on healthcare facilities to accurately track and document resources/supplies used in the delivery of care with note that supplies are a hospital’s second-largest expense, accounting for 35 to 45 percent of their operating budget, according to researchers.
The results of the research also led the researchers to conclude hospital administrators should not take a slow, piecemeal, or phased in approach when utilizing RFID and EDI simultaneously. Instead, they should go all in. “We found that hospitals that use RFID alone, or EDI alone, perform worse than hospitals that have neither solution in place,” researchers wrote—but like many good things, the real savings come to those who successfully combine the technologies together for maximum benefit.
Other authors in this study included Terry Esper of Ohio State University, Joonhwan In of Ulsan National Institute of Science and Technology, Bogdan C. Bichescu of the University of Tennessee and Terry A. Byrd (Retired Bray Professor Emeritus) from the Harbert College.
Kang Bok Lee is EBSCO Associate Professor of Business Analytics within Harbert College’s Department of Systems and Technology. He has published in journals such as the Academy of Management, International Journal of Research in Marketing, Physica A and Strategic Management Journal.
Randy V. Bradley is an Associate Professor of Information Systems and Supply Chain Management in the Haslam College of Business at the University of Tennessee. He holds a Ph.D. in Management of Information Technology and Innovation, an M.S. in Management Information Systems, and a B.S. in Computer Engineering, all from Auburn University. As a supply chain and IT strategist and researcher, Bradley's expertise includes digital business transformation, supply chain digitalization, and the strategic application of business analytics and IT in the supply chain.
BY JOE MCADORY

from left: Kang Bok Lee and Randy Bradley
Categories: Health Sciences, Cyber, Advanced Systems
Auburn study: Hospital annual net patient care revenue increases by $1.7 million, on average per unit, through new IT implementation
Recently published research from Auburn University’s Harbert College of Business found information technology plays a vital role in enhancing hospital revenue. In their paper, “Does IT Improve Revenue Management in Hospitals?” published in the Journal of the Association for Information Systems, Kangkang Qi and Sumin Han, assistant professors in the college’s Department of Systems and Technology, show implementations of new IT systems not only increase net patient revenue, but also reduce money lost in uncompensated care.
Using data from more than 5,300 health care providers, Qi and Han studied the relationships between clinical and business IT investments and revenue management performance. According to their findings, clinical and business IT implementations lead to short-term and long-term higher revenue generation. The combination of one additional unit of clinical IT implementation and one additional unit of business IT implementation increased a hospital’s annual net patient care revenue by $1.73 million on average.
Another mechanism through which hospitals manage revenue is via controlling uncompensated care for indigent patients who cannot be turned away, or patients who have not fully paid their medical bills. Why is this important? The American Hospital Association stated that hospitals have provided more than $660 billion in uncompensated care to patients since 2000. In contrast, the paper revealed that one more unit of clinical IT and one more unit of business IT adoption decreased uncompensated care ratios by 27.9% and 19.1%, respectively.
Improved information technology services were found to play an integral role in allowing hospitals to identify mechanisms to enhance revenues via billing, budget, scheduling, utilization management, debt collection, human resource and property management systems through improved efficiencies.
With note that U.S. hospitals will spend approximately $120 billion on information technology in the coming years, this Harbert College research finds such investments to be a wise business decision.

From left: Kangkang Qi is an assistant professor of information systems management and Sumin Han is an assistant professor in the Department of Systems and Technology in Auburn’s Raymond J. Harbert College of Business.
Categories: Health Sciences, Cyber, Advanced Systems
Hoang earns first NSF CAREER Award for Department of Mathematics and Statistics
Auburn University mathematics professor Thi-Thao-Phuong Hoang hopes to use applied and computational mathematics to help scientists better understand and potentially solve real-world problems like water contamination and climate change, and the department’s first-ever National Science Foundation, or NSF, CAREER Award could help her do exactly that.
“My job is to develop, analyze and implement numerical methods to solve the mathematical models of those real-world physical processes and phenomena,” said Hoang, just the second professor in the state of Alabama to receive an NSF CAREER award in mathematical sciences since it was created in 1995. “I am passionate about interdisciplinary research, and I want to do both the theoretical and practical things, and I find it more motivational when I see the application of my work and how it is used and applied to better understand our world.”
A rising star in Auburn’s Department of Mathematics and Statistics in the College of Sciences and Mathematics, or COSAM, Hoang was notified in February about the historic award that will provide the Vietnam native and her team nearly $440,000 in funding for the next five years. The prestigious honor—administered by the NSF’s Faculty Early Career Development Program—was both humbling and inspiring for Hoang, an assistant professor.
“I’m very excited about it, and it’s a great thing to know all of your hard work has paid off,” said Hoang, winner of the department’s Jack B. Brown Endowed Faculty Award for 2021-23. “You feel very motivated to continue with what you’re working on now that you have the resources and recognition. I am also grateful to my advisors, mentors and collaborators for their constant support and valuable advice.”
Hoang hopes to use the award to recruit and train undergraduate and graduate students, purchase state-of-the-art computer equipment, attend conferences and attract elite-level mathematicians to Auburn for discussions and speaking engagements. By increasing her team’s size and capabilities, Hoang will look to use her expertise in applied and computational mathematics, as well as numerical analysis, on a grander scale to help scientists and colleagues potentially solve real-world environmental problems.
In addition, she will bolster COSAM’s effort to attract and support high school students via the Auburn University Summer Science Institute, or AU-SSI, an educational enrichment program administered by COSAM’s Office of Outreach. It is designed for highly motivated rising 11th- and 12th-grade students from Alabama and Georgia with a high aptitude and interest in pursuing a degree in science, math or a related field.
“As part of the educational component of my CAREER project, I will develop curricular modules in computational mathematics at the AU-SSI to provide young students early exposure to applied mathematics and inspire them, especially girls, to pursue a career in mathematics,” said Hoang, recipient of COSAM’s 2020 Dr. Robert K. Butz Award for Excellence in Teaching.
Hoang earned her bachelor’s in mathematics from Ho Chi Minh City University in her native Vietnam, completed her master’s in applied math at University d’Orleans on Orleans, France, then lived in Paris for nearly four years while she completed her doctorate in applied mathematics from Universite Pierre et Marie Curie. After teaching at her alma mater in Vietnam from 2014-17, she completed a postdoctoral fellowship at the University of South Carolina—where she was part of a team working on a research project about climate and earth system modeling funded by the Department of Energy—before joining the Auburn faculty as a tenured-track professor in 2018.
Fluid dynamics—which provides methods for studying the evolution of ocean currents, weather patterns, plate tectonics and even blood circulation—and how it applies to real-world situations, is an area of interest for Hoang and her team. By designing algorithms to study how the ocean interacts with coasts and the rest of an area’s ecosystem, Hoang hopes to use math to contribute to scientists’ understanding of how the world is changing and the depth and breadth of everyday environmental dilemmas.
“Fluids are everywhere in our world, and I’m [particularly] interested in environmental science,” Hoang said. “So, I’ve been doing nuclear waste repository simulations, where you simulate the transport of radiation nuclides and where they’re buried in the ground. I do ocean modeling, so I simulate the movement of water in the ocean and things like that, water cycles and the interactions between surface and sub-surface flows.”
Hoang also has long-term goals for her research, including streamlining efficiency and accuracy of numerical methods and their parallel implementation.
“My research is Multiphysics and multiscale systems,” she said. “These systems are everywhere and are difficult to simulate correctly. The challenges come from the fact that you have different physics which occur on different spatial and time scales; moreover, they’re coupled together, so there’s some interaction between them which needs to be considered in the simulation.
“Our goal is to develop stable, accurate and efficient numerical methods based on domain decomposition and local time-stepping for solving large-scale Multiphysics multiscale problems.”
Department Chair Ash Abebe has been impressed with Hoang’s work ethic and is excited about what she has brought to Auburn, as well as what her team can achieve in the future.
“Dr. Hoang’s research program, focused on developing novel numerical methods and numerical analysis for partial differential equations, is a very important component of the department's research portfolio,” Abebe said. “Her research has broad applications from transport through porous media, to climate modeling, to solid mechanics and is supported by two concurrent NSF grants she has obtained since coming to Auburn in 2018 and for which she is the sole primary investigator. This award is an indicator of the growing profile of the Department of Mathematics and Statistics as a research leader in the state and the nation.”
Hoang said she and her husband, Tuan, and 6-year-old son, Minh, have thoroughly enjoyed living in Auburn and becoming part of the Auburn Family. She feels the community’s warm and welcoming nature will help provide a great environment for her research work to thrive.
“I think Auburn is such a great place to live, honestly,” she said. “I love being here, and the people around me are all friendly. I can feel the spirit, and so many people with the same interest is really awesome. The COSAM family is great, and I really feel a supportive environment from the people here.
“I feel very lucky.”

Auburn Assistant Professor Thi-Thao-Phuong Hoang has won the first National Science Foundation CAREER Award in the history of the Department of Mathematics and Statistics. She hopes to use applied and computational math to help solve real-world problems like climate change.
Categories: Health Sciences, Energy & the Environment, Science, Technology, Engineering and Mathematics (STEM)
Sixty-three students win awards at ‘Auburn Research: 2021 Student Symposium’
Sixty-three students took home awards for their research and creative scholarship posters and oral presentations during the recent, virtual “Auburn Research: 2021 Student Symposium.” Nearly 350 undergraduate and graduate students from Auburn and Auburn Montgomery participated in the annual symposium, which gives students an opportunity to share their work university-wide and with the general public.
Undergraduate Research Awards
The undergraduate first-place award in the Science, Technology, Engineering and Mathematics poster presentations went to Anna Solomonik of Drug Discovery and Development. Shalom Kim of AUM Chemistry and Biochemistry captured first place in the STEM oral presentations.
In the category for Human Sciences, Social Sciences, Creative Arts, Nursing and Humanities, Sally Ann Missildine of Interior Design won first place for her poster presentation, while Stanley Wijaya of Nutrition, Dietetics and Hospitality Management took first in the oral presentations.
Graduate Research Awards
The graduate first-place winner for the Science, Technology, Engineering and Mathematics poster presentations was Manjusha Annaji of Pharmaceutical Sciences, while first place in the STEM oral presentations went to Kaelyn Fogelman of Fisheries, Aquaculture and Aquatic Sciences.
In the category for Human Sciences, Social Sciences, Creative Arts, Nursing and Humanities, Kassandra Ross of Consumer and Design Sciences won first place in the poster presentations, while Juliana Parma of Kinesiology captured first in the oral presentations.
College-specific awards were also presented for undergraduate and graduate student categories. A complete list of winners, as well as titles of their projects, is available on the “Auburn Research: 2021 Student Symposium” website.
![orange and blue background graphic: Auburn Research: A Showcase of Research and Creative Scholarship Student Symposium 2021 Virtual Event march 29-April 2 [Auburn University logo]](https://cws.auburn.edu/shared/files?id=159&filename=RSRH%20-%202021%20Student%20Research%20Symposium%20Social%20Media%20Graphics_TW.jpg)
Sixty-three students have won awards for their research presentations given during the Auburn Research: Student Symposium 2021 virtual event held March 29 through April 2.
Categories: Health Sciences, Science, Technology, Engineering and Mathematics (STEM), OVPRED, Creative Scholarship, Life Sciences, Undergraduate Research, Agriculture
Auburn University heartworm research, soil study awarded LAUNCH funding
Two Auburn University research projects have been awarded a share of $100,000 from the LAUNCH Fund for Research and Innovation, a university program designed to bridge the gap between innovative research and the marketplace. The winners were selected from among five faculty teams that competed in a recent multistage competition.
A team of veterinary and public health researchers received $70,000 to study the reliability of a breath test it developed for the noninvasive diagnosis of heartworm disease in dogs.
“Our team greatly appreciates the support from the LAUNCH funding program, which will help us to robustly evaluate this novel technology in dogs for the diagnosis of heartworms,” said Assistant Professor Lindsay Starkey of the College of Veterinary Medicine’s Department of Pathobiology. “We also hope to look at the potential for this diagnostic to be used for other diseases in other species in the future.”
Fellow team members include Professor Byron Blagburn, also of the Department of Pathobiology; Associate Professor Sarah Zhody, a vector-borne disease expert from the School of Forestry and Wildlife Sciences who recently transitioned from Auburn to the Centers for Disease Control and Prevention in Atlanta; and Melissa Boersma, an analytical chemist and director of Auburn’s Mass Spectrometry Lab in the College of Sciences and Mathematics.
The test uses a chemical fingerprint found in a dog’s breath to determine if the dog is infected with heartworms. The researchers say initial results are encouraging and that LAUNCH funding will allow the team to fully establish the reliability of the test in dogs of different breeds, diets and backgrounds.
A final version of the technology could be similar to a breathalyzer for dogs, avoiding the need for drawing blood and possibly detecting the presence of heartworm earlier than current blood-based tests. This noninvasive approach to testing dogs could change the $1 billion heartworm testing market by expanding testing, as well as improving both safety and convenience for pets and veterinarians, according to the researchers.
Professor Kathy Lawrence and Research Associate John McInroy of the College of Agriculture’s Department of Entomology and Plant Pathology were awarded $30,000 to identify bacterial strains that could assist in expanding available farmland to include soils currently too salty and to increase drought tolerance of crops and grasses during changing climate.
Their project will expand Auburn’s probiotic libraries, isolate and study bacteria present in extreme conditions and identify microbes that will aid plant growth. It builds upon the successful commercialization of other libraries of bacterial strains assembled by Joseph Kloepper, professor emeritus of plant pathology, and Lawrence.
Established in 2015 by the Auburn University Research and Economic Development Advisory Board, the LAUNCH Fund was created with the support of the Office of the Vice President for Research and Economic Development as part of a commitment to advance entrepreneurship among Auburn’s research faculty.
Fund recipients have access to expert resources in Auburn Research Park’s New Venture Accelerator for startup advice and to the professional staff of the Office of Innovation Advancement and Commercialization for help in devising pathways to commercialization.
“The LAUNCH program is designed to be a catalyst to push forward promising technologies to the commercialization stage and provide critical solutions to global problems,” said Cary Chandler, director of the LAUNCH program and senior director of the Auburn Research and Technology Foundation. “The awardees this year are great examples of that in action.
“It is essential to our land-grant mission that we make investments in research and take it to market to provide real-world solutions and create jobs. Our goal is to find a way to increase the funding and frequency for this program to increase its success.”
More information about how Auburn supports experts through LAUNCH is available on the LAUNCH website.
BY LESLIE CHAPMAN
Categories: Health Sciences, OVPRED, Agriculture
SEC’s Auburn Faculty Achievement Award presented to child development researcher and sleep expert Mona El-Sheikh
Auburn University College of Human Sciences professor and world-renowned sleep expert Mona El-Sheikh has been named the recipient of the Southeastern Conference’s 2021 Faculty Achievement Award for Auburn, announced today by the SEC.
El-Sheikh, the Leonard Peterson & Co. Professor in the college’s Department of Human Development and Family Science, will receive a $5,000 honorarium from the SEC, and she becomes Auburn's nominee for the SEC Professor of the Year, who will be selected from 14 nominees representing SEC universities.
“Dr. El-Sheikh has profoundly expanded our knowledge of childhood development and adolescence, and in doing so, personifies Auburn’s mission of discovery and innovation,” said Bill Hardgrave, Auburn’s provost and senior vice president for academic affairs. “With a remarkable body of research and continued commitment to student success, she embodies what it means to be an extraordinary teacher and scholar.”
The SEC Faculty Achievement Awards, created to recognize faculty accomplishments, scholarly contributions and discoveries, were established by SEC presidents and chancellors and are administered by the SEC provosts. The awards were first presented in 2012.
Each recipient of the SEC Faculty Achievement Award must be a full professor at an SEC university, have a performance history of extraordinary teaching and a record of scholarship that is recognized nationally or internationally.
“I am honored and delighted to be chosen for this award, and I want to share credit with my colleagues, lab staff, graduate students and postdoctoral trainees, present and past, and the participating families, all of whom have been invaluable in my highly collaborative research,” said El-Sheikh, who received her master’s and doctorate in developmental psychology from West Virginia University. “I also wish to thank many administrators, present and past, at the department, college and university levels for their roles in supporting my research and facilitating its progress.”
Sleep may be the area El-Sheikh is best known for, but her research is transdisciplinary and concerns child and adolescent functioning in family and socioecological contexts and health disparities associated with poverty and race/ethnicity.
Collaboration with departmental colleagues, as well as those around campus, has been key for El-Sheikh, who said it has led to a body of knowledge, some of which can now be translated to real-world applications for the betterment of youths’ growth and development, and to addressing persistent and longstanding racial/ethnic and social class disparities.
El-Sheikh initially became interested in child development as an undergraduate student at The American University in Cairo in her native Egypt. Over the years, her interest grew as she incorporated questions from other disciplines, including pediatric sleep medicine, psychophysiology and racial/ethnic health disparities, leading to her current scholarship.
She has spent her entire academic career at Auburn, arriving on the Plains in 1990 after receiving her doctorate.
Of particular emphasis in El-Sheikh’s work is the assessment of youths’ physiological and biological reactivity and regulation examined through the autonomic nervous system and sleep regulation, which are examined as primary mechanisms of risk and vulnerability/protective factors. She said that these assessments have yielded discoveries about how early physiological reactivity and regulation establish risk for later outcomes in psychological adjustment, physical health, cognitive functioning and academic achievement.
“My goal all along has been to determine some factors that are responsible for health, educational and emotional outcomes in children and youth so that early detection, prevention and intervention can reduce the prevalence of those problems,” explained El-Sheikh. “The studies have resulted in discoveries that emphasize children’s sleep as a crucial determinant of health outcomes.
“Children who sleep well are better able to regulate their emotions, perform better academically and have better health in general. Moreover, the studies have led to the discovery that disparities in outcomes by social class are ameliorated when sleep is consistently sufficient over the course of childhood and youth.”
El-Sheikh’s work has been continuously funded by the National Institutes of Health and/or the National Science Foundation since 1996. She has also received support with internal grants from Auburn and the Alabama Agricultural Experiment Station.
El-Sheikh mentors many postdoctoral fellows and graduate students and collaborates with them on her research. Many undergraduate students from across campus work in her sleep lab and are trained in complex data collection protocols.
Her extensive list of awards includes Auburn’s Creative Research and Scholarship Award and the Research Advisory Board Advancement of Research and Scholarship Award. She is also a fellow in the Developmental Psychology Division of the American Psychological Association.
BY AMY WEAVER

Mona El-Sheikh, the Leonard Peterson & Co. Professor in Auburn University’s College of Human Sciences, has been named the recipient of the Southeastern Conference’s 2021 Faculty Achievement Award for Auburn.
Categories: Health Sciences, Auburn In the News
Three Auburn University projects among recipients of $1.05 million for breast cancer research
Three Auburn University research projects are among 14 recipients of $1.05 million in support from the Breast Cancer Research Foundation of Alabama, or BCRFA.
Nancy Merner, assistant professor in the Department of Pathobiology in the College of Veterinary Medicine, and Jingjing Qian, associate professor in the Department of Health Outcomes Research and Policy in the Harrison School of Pharmacy, are the principal investigators in projects funded by the statewide award, the BCRFA announced recently.
Merner is principal investigator on two projects—one underway with Assistant Professor Erica Stringer-Reasor of the O’Neal Comprehensive Cancer Center at the University of Alabama at Birmingham, and another with her colleague, Professor Clayton Yates, at Tuskegee University. Qian is the sole researcher in the pharmaceutical study.
“My projects are similar but distinct,” Merner said. “One is focused on inclusiveness, while the other is examining genetic risk factors associated with hereditary aspects of breast cancer in African American women.”
Merner previously had used Auburn’s Gene Machine bus to travel to underserved areas of the state to recruit participants in her studies.
“Since the COVID-19 pandemic started, we have been unable to travel and conduct our work in person,” Merner said. “Funds from this grant will enable us to conduct and continue this work virtually for enrolling participants and also support a pilot study with UAB.”
Merner’s second project employs the Alabama Hereditary Cancer Cohort that was established to reach underrepresented individuals in the state for cancer genetics research. This is being conducted in collaboration with Tuskegee University.
“African American hereditary breast cancer is understudied,” Merner said. “These funds ultimately allow us to investigate inherited breast cancer risk in African Americans, aiming to identify the genetic risk factors associated with early-onset and aggressive African American breast cancer.”
Qian’s research examines how medications shown to reduce breast cancer risks have been used in Alabama and their impact on breast cancer cases.
“For my work, I am using the Alabama Medicare and Medicaid insurance claims data,” Qian said. “About one woman in eight will be diagnosed with breast cancer during her lifetime. Evidence has shown that a few medications, including selective estrogen receptor modulators, such as tamoxifen and raloxifene, and aromatase inhibitors, such as anastrozole and exemestane, might help lower breast cancer risk, especially in women who are at high risk.
“However, the impact of these medications on breast cancer risk among women in Alabama is unknown. I am learning how these drugs have been prescribed in Alabama and about associated attributes such as dosage, duration and patient characteristics. I also am investigating the potential impact of those drugs on breast cancer risk among Alabama women.”
The BCRFA supports a comprehensive approach to battling breast cancer through support of collaborative and innovative research to help diagnose, treat, prevent and eradicate the disease. Since its inception in 1996, the BCRFA has raised almost $11 million to fund research at the O’Neal Comprehensive Cancer Center and with their collaborative partners. All funds raised stay in the state of Alabama, but the research will have a global, life-saving impact.
BY MITCH EMMONS

Nancy Merner (left), assistant professor in the Department of Pathobiology in Auburn’s College of Veterinary Medicine, and Jingjing Qian, an associate professor in the Department of Health Outcomes Research and Policy in Auburn’s Harrison School of Pharmacy, are leading breast cancer research projects that were named among among 14 recipients of $1.05 million in support from the Breast Cancer Research Foundation of Alabama.
Categories: Health Sciences
Auburn University professor looks at cheaper, more efficient solution in fight against COVID-19
While the rapid development and distribution of vaccines for preventing COVID-19 is a phenomenal advancement in the continuing battle against the virus, there are drawbacks, says an Auburn University professor.
“Vaccine production is costly and time-consuming,” said Jacek Wower, a professor of biochemistry in the College of Agriculture’s Department of Animal Sciences. “Vaccinations take time and money, require assistance from medical personnel and may be required every year.”
A cheaper and simpler solution, Wower said, is antiviral drugs.
Wower is the first co-author of a paper published recently in the journal, Communications Biology, that explores the use of an antiviral drug against SARS-CoV-2, the virus responsible for the coronavirus disease outbreak that originated in Wuhan, China, and has developed into a global pandemic.
“Antiviral drugs likely will work on many variants of the virus because the virus cannot readily modify the part of its components that are responsible for viral reproduction,” he said. “We need to remember that nature needed millions of years to develop the principal protein activities of SARS-CoV-2.”
Antiviral drugs—usually very small compounds that inhibit enzymatic functions—are one of three ways, including vaccines, of protecting people from the virus, Wower said. The third is by using monoclonal antibodies (produced in the laboratory, not in human bodies) to fight the virus at very early stages of infections.
The virus, he said, has an RNA genome that is protected by an “envelope” composed of a lipid bilayer and three structural proteins.
“The viral RNA genome encodes 28 proteins,” explained Wower. “Most of these proteins have specific functions that reproduce the virus and protect it from the human immune system. These proteins are called non-structural proteins.”
If you interrupt the functions of non-structural proteins with an inhibitor, you may be able to stop the virus reproduction and stop the progression of the disease, he said.
“Nsp15 protein is one such non-structural protein,” Wower said. “It protects virus production by interfering with the human’s innate immune response. The human body uses it immediately or within several hours after exposure to virus.”
In simple words, nsp15 activity allows the SARS-CoV-2 virus to hide from the cells that can trigger defensive actions of the human immune system.
“If nsp15 activity is blocked by an antiviral drug, the human innate immune system will destroy the virus and stop its reproduction,” Wower said. “Nsp15 is a protein, and like almost every other protein, it adopts a specific three-dimensional structure. The key to defeating nsp15 activity is finding a small molecule that will bind strongly to this protein and sit just right into one of its nooks and crannies.”
X-ray crystallography carried out by Andrzej Joachimiak and collaborators at the Argonne National Laboratory has revealed the detailed structure of nsp15.
There are two approaches to developing an antiviral drug, Wower said.
One can design and synthesize an antiviral drug from scratch, which is a costly proposition that not always produces a good drug. Or, an alternative and quicker approach is to find an existing drug and see whether it can do the job.
“We decided to use the second approach,” he said. “People expect results to come quickly, but research takes time.”
Computer-guided searches of drug databases suggested tipiracil, a compound approved by the FDA as a combination drug. It protects trifluridine that is used for the treatment of colorectal cancer.
Further studies demonstrated that tipiracil indeed can bind to nsp15, but the binding itself does not guarantee inhibition.
“My role was to devise an assay that would demonstrate that tipiracil inhibits nsp15 activity,” Wower said. “Relying on my 40 years of experience in RNA biochemistry, I synthesized a suitable RNA substrate necessary for the assay.”
The results of these studies were satisfactory but not satisfactory enough, he said. In vitro (in the tube), tipiracil inhibited the nsp15 activity but not extremely well.
The next question to be answered was: Would tipiracil inhibit reproduction of the virus in human cells? Since Auburn University does not have the lab facilities to grow SARS-CoV02, researchers turned to Professor Glen Randal from the University of Chicago’s Department of Microbiology.
Randal demonstrated that tipiracil alone may only slow down the progress of COVID-19.
“Not every research ends with an absolutely great outcome,” Wower said. “Often, more work is needed to achieve the desired result.”
This knowledge does, however, provide the insights necessary to produce an improved version of tipiracil that binds stronger to nsp15, is more easily delivered to infected cells and, in the end, inhibits progression of the COVID-19 pandemic.
The research project will continue, Wower said, with a focus on understanding the potential of the tipiracil binding site in nsp15 and analyzing complexes of the protein with other compounds.
“Once we know more about the inhibitor-binding site, then we can rationally add new parts to tipiracil to build a better drug,” he said.
BY PAUL HOLLIS

Jacek Wower, professor of biochemistry in the Auburn University College of Agriculture’s Department of Animal Sciences, is the first co-author of a paper published in the journal, Communications Biology, that explores the use of an antiviral drug in the fight against COVID-19.
Categories: Health Sciences
Auburn researcher makes significant discoveries in scope of disease, parasite spread by feral cats
Kayleigh Chalkowski, a doctoral student in the Auburn University School of Forestry and Wildlife Sciences, is leading a research study that’s making important discoveries about the scope of disease caused by a deadly parasite spread by feral cat populations—not just in Kauai, Hawaii, where the study took place—but worldwide.
The study, published recently in Pacific Conservation Biology, has public health policy implications for wherever feral cats can be found.
Researchers sampled sentinel feral chickens on Kauai as environmental indicators of the parasite Toxoplasma gondii, or T. gondii, which is spread by cats. The parasite is a leading cause of mortality among endangered species, including the monk seal, and can cause serious neurological symptoms in humans.
While the implications are for feral cats and other animals, Chalkowski’s study focused on the prevalence of T. gondii among the research area’s chicken population.
“In our study, we found that nearly 40% of chickens were positive for this parasite, and there were positive chickens at nearly every sampled site with positive correlation with proximity to the coast,” Chalkowski said.
“Our findings of positive chickens at community centers and public beach parks suggest a public health risk, and our findings of positive chickens at wildlife refuges and coastal areas suggests exposure risk to endangered birds and marine mammals.”
Chalkowski has spent years in Kauai conducting on-the-ground conservation work. The island’s wide-ranging topography, variety of ecosystem types and abundance of feral chickens offer optimal model systems to examine the parasite’s prevalence. The feral chicken is an ideal sentinel species for this research, recent evidence that T. gondii contributes to local declines of Hawaii’s endemic bird and mammal species.
Chris Lepczyk, a professor in the School of Forestry and Wildlife Sciences, was a coauthor on the study.
“Kauai, and the Hawaiian Islands more broadly, are really a focal point in the world for understanding how the parasite is spread across the landscape and how it is affecting ecosystem health,” Lepczyk said.
Chalkowski’s longtime field experience in the Hawaiian Islands led to a strong appreciation for effective predator control and an interest in diseases that impact endangered species as well as humans. Identifying this and other environmental factors that predict or impact T. gondii exposure is important for mitigating disease risks.
The one-year project involved collaboration with the Kauai Invasive Species Committee, Fish and Wildlife Service, and the University of Hawaii’s College of Agriculture and Human Resources Cooperative Extension.
“Given the dual interests of all these organizations in outreach and either public health agriculture or wildlife health, I think it was a good example of how partnerships can develop to work toward understanding an issue that can address concerns that relate to both conservation and public health,” she said.
Next steps for mitigation
There is a long road of research ahead before the health impacts of T. gondii are mitigated. And after that, public health policy change will be necessary.
“Our study is absolutely not the last step in this process of mitigating the health impacts of this parasite,” she said. “Detection and understanding how parasites like this may vary with environmental and landscape features are important to inform and direct mitigation efforts, but of course policy change is a crucial next step.
“Our hope is that in addition to guiding mitigation efforts, this study will also improve awareness of just how widespread and common this parasite is in public land-use areas.”
She and her team also hope this widespread awareness will result in more public support for animal control measures, such as prohibiting feeding of feral cats anywhere on the island, since the parasite is widespread—not site-specific or clustered in specific locations—and increasing trapping efforts to control feral cats.
“Stronger legislation on cat ownership would be helpful too: stricter fines for dumping or abandonment, requirements to spay or neuter and improving access for spay and neuter services, for a start,” she said.
Health risks far beyond the islands
These implications for public health policy are becoming clearer on islands such as Kauai, but they are hardly limited to that part of the world.
“Could these control efforts benefit other regions? Absolutely,” Chalkowski said. “T. gondii is not just a problem in Hawaii. This parasite is spread by domestic cats—which are found pretty much anywhere humans are found—and can infect any bird or mammal. This parasite can be found on every single continent, literally even Antarctica in marine mammals.
“This sounds crazy—clearly there are no populations of cats living in Antarctica—but it’s an example of the ability of this parasite to move through the environment and through chains of hosts.
“It is both fascinating and horrible, given how little we know about the health impacts of this parasite in many species,” she said. “This parasite is a problem worldwide, there's a lot we still don't know, and efforts to control or understand this parasite in one region may very well be helpful somewhere else.”
BY TERI GREENE

Kayleigh Chalkowski, a doctoral student in the Auburn University School of Forestry and Wildlife Sciences, is leading a research study that’s making important discoveries about the scope of disease caused by a deadly parasite spread by feral cat populations.
Categories: Health Sciences, Life Sciences
Auburn-developed disinfectant technology finds new potential during COVID-19 pandemic
An Auburn University-developed disinfectant technology—related to one that had early commercial success as a water purification and filtration product during the 1990s and early 2000s—has advanced to achieve new patent-protected licensing potential in the battle against the ongoing COVID-19 pandemic.
Medesol LLC, a medical technology firm in Bellevue, Washington, has entered into a technology licensing agreement with Auburn to commercialize an N-halamine-based technology developed by S.D. “Dave” Worley, a professor emeritus in Auburn’s Department of Chemistry and Biochemistry, Roy Broughton, a professor emeritus in the Department of Mechanical Engineering, Tung-Shi Huang, a professor of microbiology in the Department of Poultry Science, and others.
Following the success of their initial N-halamine-based technology, Worley’s research team has since reformulated it to have effective antimicrobial applications in textile products.
The technology is based on chlorine as an N-halamine. N-halamines have been used in various applications for years with no bacterial resistance mechanism yet identified. But the chlorine base that enables its disinfecting properties is slowly lost once the formula comes into contact with water. By combining the chlorine base with various polymers, the Auburn research team developed a solid that proved effective as a water treatment and filtration product.
“This worked very well,” said Worley, “but we found by further work that we could make a similar N-halamine into an antimicrobial formulation that is effective when incorporated into non-woven textiles.”
By exposing the chlorine N-halamine to an alcohol solution instead of water, Worley explained, the formulation forms a solid bond with the fabric.
“The alcohol evaporates, leaving the N-halamine bonded solidly to the fabric,” Worley said. “Thus, it has great potential for being applied as an antimicrobial to such things as wound bandages, surgical materials and other garments—particularly, medical protection masks. The idea is that these products are one-time use and disposable.”
“We have worked with Dr. Worley and Auburn for more than 20 years,” said Simon Johnston, chief executive officer for Medesol. “When we learned about this new potential for the technology, we jumped to enter a licensing agreement with Auburn.”
“We are very excited to be working with Medesol to commercially develop and market this technology,” said Jan Dowdle Thornton, executive director of Auburn’s Office of Innovation Advancement and Commercialization.
“Auburn’s N-halamine-based system is very inexpensive as compared to existing current alternatives, such as silver or biguanide-based systems. Moreover, it has been proven effective against bacteria and viruses and is biodegradable. This should be a significant improvement for disposable non-woven products to help prevent the spread of infection.”
Medesol presently is pursuing FDA approval to market the Auburn development in the United States as a more effective medical face mask and other forms of protective medical clothing, according to Johnston. The firm hopes to gain FDA approval within the next six to nine months. Meanwhile, Johnston believes they will find quicker marketing success internationally.
“We firmly believe that this technology can be a significant factor in providing better protection against infections and the spread of diseases,” Johnston said. “We know from its earlier applications that it is a very effective antimicrobial medium. We believe that we are very close to proving its worth in the efforts to battle COVID-19 and future disease outbreaks.”
BY MITCH EMMONS
Categories: Health Sciences, Engineering
Auburn University research projects among recipients of $2.57 million state award
Two Auburn University research projects are among the recipients of a $2.57 million award by the Alabama governor’s office to five of the state’s research institutions, Gov. Kay Ivey announced recently.
Brian Via and Beatriz Erramuspe, director and research fellow, respectively, of the Forest Products Development Center in the School of Forestry and Wildlife Sciences, were awarded $247,142 to research development of a paper-based device for a cost-effective method to detect dangerous formaldehyde emissions in wood panels.
Sabit Adanur, professor in the Department of Mechanical Engineering in the Samuel Ginn College of Engineering, was awarded $75,374 to conduct research relating to the design, fabrication and testing of novel medical face masks to prevent the spread of COVID-19 or future contagious viruses.
The grants are from the Alabama Research and Development Enhancement Fund, or ARDEF, a state-funded program created in 2019 under the Alabama Innovation Act and administered by the Alabama Department of Economic and Community Affairs, or ADECA.
The funding provides support and encourages new and continuing research that will result in products and services to improve the lives of Alabamians either from the products themselves or from new job opportunities.
“This funding from the Alabama Research and Development Enhancement Fund will help Auburn researchers continue to solve real-world problems through discovery and innovation,” said James Weyhenmeyer, Auburn’s vice president for research and economic development.
“The research being performed at our universities and institutions offers strong evidence that innovation is alive and well in Alabama," Ivey said when making the announcement. “These grants will help provide the needed resources to bring even more ideas and research to light, eventually resulting in new products and new job opportunities.”
Other institutions named in the award announcement include the Basham Institute of Science in Dadeville, Alabama, and various campuses of the University of Alabama. This is the second round of ARDEF funds awarded in this program in 2020.
Ivey earlier this year awarded $2.27 million in grants to state research institutions and programs. Three Auburn research projects were recipients in that earlier announcement.
BY MITCH EMMONS

From the left: Brian Via, Beatriz Erramuspe and Sabit Adanur
Categories: Health Sciences, Engineering, Auburn In the News, Manufacturing
Auburn University industry-academic technology commercialization venture sparked by student job search
Researchers develop small-volume diagnostic assays that could be useful for variety of diseases, conditions
We often hear the stories about industry joining with academia to turn research developments into commercially viable and marketable products. Most of those relationships develop through the promotional efforts of the university’s technology and intellectual property advancement program. Sometimes, though, they can happen when companies become interested in a graduate’s qualifications for employment.
Such is the story behind a partnership formed between Auburn University and a Philadelphia-based biotech firm to commercialize technologies developed by Christopher Easley, the C. Harry Knowles Professor in the Department of Chemistry and Biochemistry in the College of Sciences and Mathematics.
InnaMed, based in Philadelphia, is a new firm devoted to the development of easy-to-use, fast-and-accurate home blood testing and health monitoring systems for the individual patient. Alongside their work applying microfluidic methods to help understand diabetes and obesity, Easley’s research team also develops small-volume diagnostic assays that could be useful for a variety of diseases and conditions. When InnaMed learned about Easley’s research in electrochemical assay development through the interview process with one of his graduate students, the company not only wanted to hire the student, but also acquire the technology for commercial development.
InnaMed was started in 2016 by co-founders Anup Singh and Eshwar Inapuri.
“We met while students at the University of Pennsylvania,” said Inapuri, who serves as the CEO. “Anup was pursuing a degree in biophysics, and I in bioengineering. We became friends while working in the Issadore Lab on technologies to advance diagnostics and enable early detection of diseases like traumatic brain injury and pancreatic cancer in a non-resource intensive manner.”
The two formed InnaMed with the goal to bridge the clinical communication gap between health systems and their patients, and, in 2017, learned of Easley’s research in microanalytical sensing techniques while conducting a job interview with one of Easley’s graduate students, Subramaniam “Mani” Somasundaram.
InnaMed optioned the Auburn technology to test it out and visited Easley’s lab to learn how to use it. They soon decided to license the technology and found the expertise that Mani gained while at Auburn to be a great asset to the company.
“After visiting with Auburn’s Office of Innovation Advancement and Commercialization, we entered into a licensing agreement on Dr. Easley’s technology and ultimately hired Mani shortly afterwards,” Inapuri said.
Easley describes his research as developing super-sensitive, very small instruments capable of detecting and measuring many types of biomarkers.
“Electrochemistry can be used to make very small instruments,” Easley said. “One of our inventions is a generalized assay that can work for small-, medium- or large-sized molecules, giving us the possibility for rapid ‘dip and read’ methods that are attractive for point-of-care settings. However, for some clinically relevant analytes at low concentrations, background interferences can be an issue, so we also invented a modified electrochemical instrument that removes background and increases sensitivity. These unique measurements not only help my laboratory with sensing on microfluidic devices, but they also are well-suited for InnaMed’s realm, clinical readouts in human blood.”
“The pharma industry has indicated a keen interest in commercial products that can do what Dr. Easley’s technology has made possible,” Inapuri said.
The company is in the process of taking Easley’s technology from the laboratory to a marketable product that can simplify the individual patient’s health journey for a variety of conditions that require frequent, rapid and accurate testing of various types of biomarkers in the blood. Inapuri says they hope to have the product ready to seek FDA approval within the next nine months.
“This is an example of a very good industry-academia commercialization partnership,” said Troy Brady, licensing officer in Auburn’s Office of Innovation Advancement and Commercialization. “It not only shows how the commercialization process evolves and develops, but it also is a great example of how student involvement can lead to solid, real-world partnerships.”
BY MITCH EMMONS

Auburn Professor Christopher Easley and his research team have developed super-sensitive, very small instruments capable of detecting and measuring many types of biomarkers.
Categories: Health Sciences, Engineering
Auburn Vet Med Ph.D. candidate receives national awards
Francesca Mowry, a Ph.D. candidate in the Auburn University College of Veterinary Medicine, working in the research lab of Dr. Vinicia Biancardi, assistant professor of neurosciences in the Anatomy, Physiology and Pharmacology department, has been honored as the recipient of two prestigious competitive research awards in 2020.
The awards include the 2020 Van Harreveld Memorial Award, American Physiological Society’s Central Nervous System Section, recognizing outstanding neuroscience research by a graduate student. One award is presented annually in the Experimental Biology meeting. Although Mowry was announced as this year’s winner, due to the COVID-19 pandemic, she will be formally recognized with the award at the group’s 2021 meeting.
Mowry’s second award is the New Investigator Travel Award, presented by the Council of Hypertension, American Heart Association, which encourages new investigators to undertake or continue hypertension research. Applications are judged primarily based on the scientific ranking of the candidate’s abstract selected for presentation at the Hypertension Scientific Sessions, to be held online in September 2020. The award is competitive and presented annually to up to 10 new investigators among graduate students, postdoctoral fellows, residents, and instructors.
“Francesca is an incredibly hard worker,” says Dr. Biancardi of Mowry’s exceptional double recognition. “Her work aims to understand the central nervous system mechanisms involved in hypertension, a disease affecting one-third of the adults in the U.S. She is driven and passionate about what she does, and these awards are a well-deserved recognition of her accomplishments by the scientific community.”
BY MIKE JERNIGAN

Francesca Mowry
Categories: Health Sciences
Harrison School of Pharmacy assistant professor studying psychological factors related to genetic testing
A recent trend in health care is the increase in genetic testing as part of a precision-medicine approach. Dr. Natalie Hohmann, assistant professor in the Harrison School of Pharmacy’s Department of Pharmacy Practice, is seeking out the psychological factors that affect the decision to pursue genetic testing.
The project titled “Psychosocial Factors Affecting Genetic Testing Decisions in Cancer,” was recently funded by the Pharmaceutical Research and Manufacturers of America Foundation, or PhRMA, with a $100,000 Research Starter Grant in Health Outcomes.
The funding from PhRMA over one year supports work that spans a broad spectrum of issues related to health care delivery, studies evaluating effectiveness of a pharmaceutical intervention and the impact of reimbursement policies on outcomes of care. Potential projects also range from the development and use of patient-level real-world data and tools to perform patient-based assessments to analyses of ways in which results of Health Outcomes Research are disseminated to providers or consumers to encourage behavior change.
“The goal of this project is to investigate which psychosocial factors affect the public’s decisions to undergo genetic testing for precision cancer medicine,” said Hohmann. “Psychosocial factors may include humanistic factors like peace of mind, value of hope and social norms; and patient-experience factors like attitudes towards uncertainty and acceptable benefit-to-risk trade-offs.”
Working with Hohmann on the project are co-investigators Dr. Surachat Ngorsuraches, associate professor in the Harrison School of Pharmacy’s Department of Health Outcomes Research and Policy, and Dr. Winson Cheung, professor at the University of Calgary. Ngorsuraches has also served as Hohmann’s research mentor through the process.
The group will also explore how the humanistic and patient-experience values change among different demographic populations. The findings can be used to design targeted education materials and decision aids that help the public clarify their values related to genetic testing in cancer.
“The primary positive impact of study findings would be an increase in the implementation of precision cancer medicine due to better understanding of the holistic value of genetic testing in cancer,” said Hohmann.
Precision medicine, sometimes referred to as personalized medicine, involves using genetic testing to tailor medical decisions, practices and therapies to a specific patient.
“As technology advances, the role of genetic testing in prevention and treatment of health conditions also advances,” said Hohmann. “It is one more tool in healthcare providers’ toolbox, that can help providers identify and discuss the most effective and safe prevention and treatment options with each individual.”
With any new testing or treatment related to health care, there can be apprehension or anxiety when it comes time to make decisions related to cancer therapies.
“As genetic testing becomes more common, we need to think about how people interpret the results of genetic tests and how they make decisions based on these results,” said Hohmann. “More information and education are needed for both healthcare providers and patients to really understand and feel comfortable with genetic testing.”
While attacking the tumor or cancer cells, many current cancer treatments also incidentally attack healthy cells. This can cause undesirable side effects or complications as patients go through treatment.
Hohmann hopes that with processes like precision medicine and the results of her work that patients can make informed decisions with ease of mind and improve their health outcomes.
“Psychosocial factors are important to study so we can get an idea about what types of things impact people’s psychological wellbeing,” said Hohmann. “This is especially important for health conditions like cancer, where patients are faced with difficult and confusing decisions about treatment.
“I wanted to learn more about how things like value of hope, trust in your doctor, and family members’ opinions affect these difficult decisions. At the end of the day, I hope that the results of this study can help spotlight the importance of treating the whole person, not just treating the cancer.”
--------------
About the Harrison School of Pharmacy
Auburn University’s Harrison School of Pharmacy is ranked among the top 25 percent of all pharmacy schools in the United States, according to U.S. News & World Report. Fully accredited by the Accreditation Council for Pharmacy Education (ACPE), the School offers doctoral degrees in pharmacy (Pharm.D.) and pharmaceutical sciences (Ph.D.) while also offering a master’s in pharmaceutical sciences. The SchoolÕs commitment to world-class scholarship and interdisciplinary research speaks to AuburnÕs overarching Carnegie R1 designation that places Auburn among the top 100 doctoral research universities in the nation. For more information about the School, please call 334.844.8348 or visit http://pharmacy.auburn.edu.
Making Medications Work Through Innovative Research, Education and Patient Care

Dr. Natalie Hohmann, assistant professor in the Harrison School of Pharmacy’s Department of Pharmacy Practice, is seeking out the psychological factors that affect the decision to pursue genetic testing. The project titled “Psychosocial Factors Affecting Genetic Testing Decisions in Cancer,” was recently funded by the Pharmaceutical Research and Manufacturers of America Foundation, or PhRMA, with a $100,000 Research Starter Grant in Health Outcomes.
Categories: Health Sciences
Auburn College of Veterinary Medicine partners with Humane Genomics Inc. on COVID-19 vaccine development
Researchers from the Auburn University College of Veterinary Medicine are partnering with Humane Genomics Inc. to develop a potential vaccine for the COVID-19 virus currently at the heart of the ongoing global pandemic.
According to Dr. Bruce Smith, director of the Auburn University Research Initiative in Cancer, professor in the Department of Pathobiology and scientist in the college’s Scott-Ritchey Research Center, the collaboration between Auburn and Humane Genomics is an outgrowth of cooperation between the two in the field of cancer research. Much of the science used in this particular vaccine development is adapted from the company’s cutting-edge research into precision virus-based cancer therapies.
“We had previously worked with Humane Genomics in the area of cancer treatment,” said Smith, “specifically an attempt to custom synthesize viruses to target tumors. The same basic concept can also be used to develop a vaccine. All that is necessary is to have the virus’ genome—a genetic map of its DNA—in order to create a vaccine to target it.”
The COVID-19 genome is available, so the custom development of a vaccine tailored to its specific vulnerabilities, a so-called “synthetic vectored vaccine,” was a relatively rapid process. In this case, that process involved genetically synthesizing via computer modeling a harmless virus called vesicular stomatitis virus, or VSV, and giving it the same “spike” protein characteristic of COVID-19. This spike protein binds with so-called ACE2 receptors on human lung cells to allow the harmful virus to infect them. But if the vaccine functions as hoped, the immune system would be triggered to produce antibodies to recognize this spike protein and block infection, but in a harmless virus. That same triggered immune reaction—in theory—would then protect against COVID-19.
“The idea of developing vectored vaccines by ‘cutting and pasting’ virus DNA to alter its characteristics is a proven method of vaccine development and has been in use for more than a decade,” Smith said. “In the case of animals, vectored vaccines have been successfully developed for rabies and fowl pox. In human medicine, a vaccine approved in 2019 for the deadly Ebola virus was developed using the same technique.
“What makes the Humane Genomics approach unusual,” added Smith, “is that they are skipping the traditional cutting and pasting process of removing and substituting DNA and instead synthesizing their targeted viruses using computer modeling. It allows for a much quicker process. If they have the target’s genome, they can develop a vaccine in about a week.”
It is the testing phase that takes time, and currently the company’s COVID-19 vaccine is in the safety testing phase, which is where Auburn’s contribution comes in. The Auburn College of Veterinary Medicine is testing the vaccine on rats to see if they develop the proper antibodies or become ill due to unforeseen side effects. Later, another vaccine partner will perform similar tests with guinea pigs, and if all goes well, the vaccine can then move on to human testing.
Smith says that, while he is cautiously optimistic a working vaccine will eventually be developed, there is still a long road ahead despite the urgent need.
“With a tremendous amount of luck, we could have a vaccine by the end of the year,” he said, “but more likely, we won’t know for sure if a vaccine is going to be successful until some time in 2021.”
BY MIKE JERNIGAN

Dr. Bruce Smith is the director of the Auburn University Research Initiative in Cancer; professor in the College of Veterinary Medicine’s Department of Pathobiology; and scientist in the college’s Scott-Ritchey Research Center.
Categories: Health Sciences
Auburn University awarded $1.31 million in research project funds from state of Alabama
Three Auburn University research projects have received a combined $1.31 million award, through a new program administered by the Alabama Department of Economic and Community Affairs, or ADECA.
Gov. Kay Ivey announced the grants this week through the new Alabama Research and Development Enhancement Fund. The state-funded program was created in 2019 under the Alabama Innovation Act.
The multidisciplinary projects are funded as follows:
-
$245,865 to develop an advanced biosensor using forest and agricultural products that will have a wide variety of uses dealing with contaminant detection, like determining if pesticides are present in water. The project is conducted by Samuel Ginn College of Engineering faculty members Virginia Davis, Alumni Professor, and Robert Ashurst, the Uthlaut Family Associate Professor from the Department of Chemical Engineering; and Soledad Peresin, an assistant professor of forest biomaterials in the School of Forestry and Wildlife Sciences.
-
$868,145 to develop a lightweight material that blocks mosquito bites while retaining coolness in hot weather. The research is being done by John Beckmann, an assistant professor in the Department of Entomology and Plant Pathology in the College of Agriculture.
-
$193,960 to develop a filtering process to remove perfluoroalkyl and polyfluoroalkyl substances from water and landfill runoff. The manmade substances are used in food packaging, stain repellants, cookware and firefighting foam and do not readily break down. The investigator for this project is Dongye Zhao, the Auburn Alumni Engineering Council Professor in the Department of Civil Engineering.
“This fund will enable our universities, hospitals, research institutions and others to develop and bring to fruition ideas that will improve lives and create jobs,” Ivey said about the grant program in the announcement. “I am tremendously encouraged by this program and its potential in Alabama.”
Jan Thornton, executive director of Auburn’s Office of Innovation Advancement and Commercialization, or IAC, said the ADECA grants are now an annual funding opportunity for researchers, with proposal submissions for the next award cycle currently open through July 29.
Faculty who wish to learn more and want to ensure that their research is protected as technology that might be potentially commercialized should contact the IAC by visiting iac.auburn.edu.
BY MITCH EMMONS

Categories: Health Sciences, Energy & the Environment, Engineering, Auburn In the News
Auburn researchers receive $1.7 million grant to study effects of marijuana use during pregnancy
Auburn University researchers have received a $1.7 million grant to study the effects of marijuana use during pregnancy. Funded by the National Institutes of Health-National Institute on Drug Abuse, the project will look at the prenatal effects of THC while also investigating treatment options.
The study is led by Miranda Reed and Vishnu Suppiramaniam, both of the Department of Drug Discovery and Development. Titled “Elucidation of molecular mechanisms of prenatal cannabinoid exposure: Identification of targets and therapies,” it is funded for five years with $352,843 in the first year for a total of more than $1.7 million.
With increased legalization of marijuana in recent years, a rising trend has been its use by expectant mothers as a way to ward off nausea and morning sickness. While many recognize the dangers of smoking, tetrahydrocannabinol, or THC, is still found in other forms like vaping, gummies and brownies and can have an effect on neuronal communication.
“Marijuana has shown to have some potential medicinal properties, which can alleviate nausea in patients undergoing cancer chemotherapy and help with appetite in patients with AIDS-associated wasting syndrome,” said Suppiramaniam. “These effects have led to the popular belief that marijuana can also help with nausea and reduced appetite associated with morning sickness during pregnancy.
“With more and more states legalizing the medicinal and recreational use of marijuana, its use during pregnancy is also rising. Nonmedical personnel at marijuana dispensaries are also currently recommending marijuana to pregnant women for nausea in some states, while medical experts strongly warn against it.”
As part of the study, the duo plans to look at how prenatal cannabis/marijuana exposure affects adolescent offspring. In particular, they are studying the communication among neurons, synaptic functioning and the resulting consequences in cognition, learning and memory.
“The effect of THC on neurons is complex and is shown to have both excitatory and inhibitory effects on neurons,” said Suppiramaniam. “It can lead to impaired learning and memory and also affect mood and emotions.”
Use during pregnancy can impact almost all the major neurotransmitters in the brain, including glutamate, adrenalin, serotonin and dopamine. This can lead to a variety of behavioral and memory issues, as well as future drug use, anxiety and depression.
“Marijuana use during pregnancy is associated with elevated risk for miscarriages, birth defects, developmental delays and learning disabilities, including lasting harm to intelligence, attention, executive functioning skills and memory,” said Reed.
The second part of the study is identifying therapeutic targets for the treatment of cognitive deficits associated with prenatal marijuana exposure. Reed and Suppiramaniam have already identified one target, the polysialylated neural cell adhesion molecule, or PSA-NCAM, which plays a critical role in learning and memory.
“For the current studies, we are examining alterations in the prefrontal cortex and hippocampus, brain regions that mediate executive functioning skills and memory,” said Reed. “We are focusing initially on alterations in the glutamatergic neurotransmitter system as it plays a critical role in these processes and the endocannabinoid system is a critical master regulator of glutamatergic signaling.”
The information will be used to test whether increasing PSA-NCAM with a novel drug can stabilize neuronal communication and improve the cognitive deficits observed after prenatal cannabis/marijuana exposure.
“Currently, we are exploring postnatal therapeutic options,” said Suppiramaniam. “We are exploring novel drugs and molecules that can be delivered to the offspring during the early adolescence period to stabilize the synaptic transmission and improve learning and memory.”
Reed and Suppiramaniam work out of the Harrison School of Pharmacy’s state-of-the-art Pharmacy Research Building and are co-directors of the Auburn University Center for Neuroscience Initiative, or CNSi.
“The Pharmacy Research Building has allowed for easy integration of our collaborative work and personnel,” said Reed. “The in-house vivarium has allowed for a reduction in time spent traveling to off-site buildings, thereby increasing productivity.”
Additionally, bringing investigators together under the umbrella of the CNSi has fostered collaboration and innovation in pursuing and receiving grants, such as this R01 grant from the National Institutes of Health.
“We are very grateful that the CNSi has partially provided support to enhance the existing infrastructure and to recruit expertise needed to carry out this project,” said Suppiramaniam. “It certainly provides a conducive and collaborative environment for exchange of ideas between faculty, staff and student scientists and is a catalyst for cutting-edge research.”
BY MATT CROUCH
Auburn University's Harrison School of Pharmacy is ranked among the top 20 percent of all pharmacy schools in the United States, according to U.S. News & World Report. Fully accredited by the Accreditation Council for Pharmacy Education (ACPE), the School offers doctoral degrees in pharmacy (Pharm.D.) and pharmaceutical sciences (Ph.D.) while also offering a master's in pharmaceutical sciences. For more information about the School, please call 334.844.8348 or visit the Harrison School of Pharmacy website.
Categories: Health Sciences
Auburn Engineering faculty collaborating on COVID-19 sensing device
An assistant professor in the Auburn University Samuel Ginn College of Engineering has received a $200,000 grant from the National Science Foundation to develop a biosensor that will rapidly detect COVID-19.
COVID-19 belongs to a family of similar viruses known as beta coronaviruses. There have been two other such viruses that have emerged over the past two decades – Middle East respiratory syndrome (MERS) and severe acute respiratory syndrome, commonly referred to as SARS.
“There are similarities between the viruses that cause MERS, SARS and COVID-19 to the point where the name of the current virus is SARS-CoV-2,” said Robert Pantazes, assistant professor in the Department of Chemical Engineering and the principal investigator on the project. “What we’re doing is using computational tools and experimental methods to try to take advantage of all the resources that were already in existence for these other coronaviruses and convert them into tools that will work with COVID-19 and potential future coronavirus outbreaks.”
The research project, titled “Antibody-Based Nanoplasmonic Barcode Biosensors for COVID-19 Detection,” is led by Pantazes in collaboration with Pengyu Chen, assistant professor in the Auburn University Department of Mechanical Engineering and Jennifer Maynard, the Henry Beckman Professor of Chemical Engineering at the University of Texas.
Specifically, the team of researchers are developing an inexpensive, near-real-time, point-of-care diagnostic device that would meet the need to more quickly and more conveniently diagnose COVID-19 and understand its spread.
“My lab has a long history in developing nanomaterial-based biosensors for immune detection,” said Chen, a co-investigator on the project. “This biosensor design originated from a multiplex barcode sensor for high throughput sensitive cytokine measurements in human serum samples and can be further applied to saliva and throat swabs.”
The team plans to screen and select optimized antibodies that can target the spike protein on the surface membrane of the virus. They will then immobilize the selected antibodies on glass substrates to capture the virus.
“We will flow in signaling nanoparticles functionalized with detection antibodies that can attach to the captured virus to form a so-called ‘sandwich’ structure,” Chen said. “These nanoparticles can emit strong scattering light with specific color and can be visualized under microscope or even by human eyes. So if we have a positive response, we will observe a brightened barcode or colored test strip.”
The team is progressing toward a proof-of-concept device that can be used for lab testing to be followed by a prototype of an integrated test strip that could be potentially used at home or in clinics.
“The academic research community is working rapidly to reduce the impact that this pandemic has on our daily way of life,” Pantazes said.
BY CASSIE MONTGOMERY
Media Contact: Cassie Montgomery, cmontgomery@auburn.edu, 334.844.3668

Assistant professors Pengyu Chen and Robert Pantazes
Categories: Health Sciences, Engineering
Auburn-developed microscope technology finds use on COVID-19 battlefront
An Auburn University-developed light microscope technology that has been on the market since the early 2000s has found new potential as a research tool on the COVID-19 battlefront.
CytoViva Inc., a subsidiary company of the Auburn Research Park-based firm Aetos Technologies Inc.—and the registered name for the patented microscope technology developed by Professor Vitaly Vodyanoy of Auburn’s College of Veterinary Medicine—has partnered with Joanna Sztuba-Solinska, an assistant professor of biological sciences in the College of Sciences and Mathematics, to aid in her research efforts.
A molecular virologist, Sztuba-Solinska has focused her research on the herpesviruses, but with the current COVID-19 pandemic, she has begun to expand her research focus to studying SARS CoV-2, the virus that causes the COVID-19 disease.
“This is a dramatically different type of virus,” she said. “I study Kaposi’s sarcoma-associated herpesvirus, which is a DNA virus that as most herpesviruses, coevolved with human population for very long time, thus, it is much less virulent.
“SARS CoV-2 is a newly emerged virus with probably the largest RNA genome, and the unique capacity of proofreading its mistakes—which you usually don’t see with RNA viruses. However, because it’s an RNA virus it has more so to speak evolutionary flexibility, meaning, it can undergo mutations, and go from animal reservoir to unfortunately human reservoir. Also, because it is a newly emerged virus, it has a much greater virulence, that is, the capacity to cause the disease or even death.”
While Sztuba-Solinska says she is optimistic that efforts underway to produce an effective COVID-19 vaccine will be successful, the process takes many months to develop, test and confirm the effectiveness and human safety of a new vaccine.
Meanwhile, her immediate research in the area of coronaviruses and COVID-19 is focused on working collaboratively with researchers in the Samuel Ginn College of Engineering on polymers to be used in antimicrobial materials for protective face masks, and in determining if the differences in types of coronaviruses can be detected visually by observing changes in their spectra.
“This is where I will be able to use the CytoViva microscope and its high-resolution capabilities,” she said, adding that she should have a unit set up and in operation in her lab within two weeks.
Introduced in 2004, CytoViva technology has been installed in hundreds of research laboratories. This includes leading national research laboratories, academic institutes and private industrial labs across the Americas, Asia and Europe.
CytoViva had principally focused on the use of its technology in the engineered nanomaterials world associated with drug delivery. In 2008, CytoViva integrated its proprietary hyperspectral imaging technology with the patented microscope developed by Vodyanoy to provide quantitative data analysis.
“Interestingly, though, viruses are nanoparticles, too,” said Byron Cheatham, CytoViva vice president for marketing. “Given CytoViva’s capability to detect live viruses like coronavirus, we have reached out to the biomedical community. We firmly believe that this technology can be an effective and efficient tool on the front against COVID-19 and other infectious diseases research.”
Vodyanoy, who was named a fellow of the National Academy of Inventors in 2013, added that “hyperspectral imagery of a single cell” would allow identification of the coronavirus infection.
The CytoViva microscope has won several major national awards: R&D Magazine's top 100 most technologically significant products introduced in 2006 and 2007 and the Nano 50 Award by NASA Tech Briefs, which recognizes the most exceptional new products in the nanotechnology field.
BY MITCH EMMONS

Joanna Sztuba-Solinska, assistant professor in Auburn’s College of Sciences and Mathematics, will use the CytoViva microscope to research SARS CoV-2, the virus that causes the COVID-19 disease.
Categories: Health Sciences, Engineering
Virologist discusses SARS-CoV-2 vaccine development, challenges for scientific community
Dr. Constantinos Kyriakis, assistant professor in the College of Veterinary Medicine’s Department of Pathobiology, discusses the role of vaccines in protecting against COVID-19 and helping prevent the spread of the novel coronavirus, as well as the unique challenges scientists are facing in developing safe, effective vaccine candidates. His research, primarily focused on zoonotic influenza viruses and novel vaccine technologies for more than a decade, will soon involve a minimally invasive study of a variety of COVID-19 vaccine candidates’ ability to trigger an immune response in swine when used alone or in combination with adjuvants.
Will social distancing, quarantine and isolation alone help control and eradicate SARS-CoV-2?
When applied at the right time, social distancing combined with quarantine and isolation of infected individuals are the most efficient non-pharmaceutical intervention tools that can slow down an epidemic and help the healthcare system cope with increased numbers of patients. This is what epidemiologists describe as “flattening the curve.” However, considering that SARS-CoV-2 might become an endemic seasonal pathogen like influenza, other tools, specifically vaccines and, to a lesser extent, antiviral drugs, will be required to reduce virus transmission, morbidity and mortality.
What is a vaccine and why is it important for this novel coronavirus pandemic?
A vaccine is a biological product delivered to humans or animals which provides immunity to a specific infectious disease. While there are several vaccine technologies, viral vaccines usually contain or generate parts of a given virus, known as antigens, that the immune system will recognize and then produce neutralizing antibodies against the target virus. Developing and deploying safe and effective vaccines against SARS-CoV-2 is of paramount importance. Mass vaccinations will help built what is known as “herd immunity,” the cornerstone of infectious disease control. This will not only protect individuals from the virus but the entire community and, importantly, high risk groups, including the elderly and people with preexisting health conditions.
How does development of a vaccine for SARS-CoV-2 differ from the development of other vaccines like the flu vaccine?
Unlike influenza vaccines, there are no licensed vaccines against any coronavirus in humans. In 2009, when the H1N1 influenza pandemic virus emerged, there were influenza vaccine platforms already established that had been in use for decades and that were proven very safe and effective. It was therefore relatively easy to produce and deliver vaccines against that influenza virus within a few months. With SARS-CoV-2 there are only limited data from experimental vaccines designed against SARS-CoV-1 and MERS-CoV, two related coronaviruses that emerged in 2002 and 2013, respectively, and caused limited epidemics. These experimental vaccines were tested in animal models and only one vaccine was tested in a phase I human clinical trial. Therefore, developing a safe and efficacious vaccine against SARS-CoV-2 is a major challenge for the scientific community. Testing vaccines in animal models is extremely important. Using reliable animal models allows us to identify target antigens, optimize the vaccine dose and formulation and, thus, move to human clinical trials with only the best vaccine candidates.
As universities and pharmaceutical companies work around the clock to find a vaccine for SARS-CoV-2, what is the likely timeframe for a vaccine to become available for the public?
As Dr. Anthony Fauci, director of the National Institute of Allergy and Infectious Diseases, has been explaining in recent statements, a vaccine will not be available for at least twelve to 18 months. This is a realistic timeframe, as long as at least one of the current vaccine candidates is proven to be safe and effective. It is important to understand that the established licensing procedures are exhaustive and time consuming to ensure the vaccine that will be deployed is very safe and highly efficacious.
What is the process for vaccine approval? Is it possible to amend this process to lessen the time needed to develop a vaccine to stop the spread of SARS-CoV-2?
Typically, the development of a new vaccine from concept to approval consists of the following stages: (a) the exploratory stage during which the specific antigen and vaccine type are identified and developed; (b) the pre-clinical stage, in which the safety and efficacy of the product are tested in cell culture systems and in animal models; and (c) three clinical trial phases (I, II and III) during which the vaccine is tested in humans. In a phase I clinical trial, a small group of healthy individuals receive the vaccine and are monitored to confirm the safety of the product and determine if it elicits the appropriate immune responses. A phase II clinical trial is conducted using a larger number of participants, which includes individuals with increased risk of contracting the disease. During this phase, participants will be randomly selected to receive a placebo in place of the vaccine candidate. This critical step offers information about both the safety and, importantly, the efficacy of the vaccine. Finally, a phase III clinical trial is the most extensive step in this process. There are thousands of participants during this randomized and double-blinded study, with some participants receive a placebo instead of the vaccine. This is the longest, most critical stage that will offer extensive information about the safety and efficacy of the vaccine. Every phase of this procedure is extremely important, must be conducted carefully and in a timely fashion. Considering sufficient time is needed to produce the vaccine once these development and testing phases are complete, it is easy to understand why it will take so much time for a vaccine to become available. All of these steps take time and are critical to ensuring safety and effectiveness of the final product. It would not be wise to abbreviate the process.
About Dr. Constantinos Kyriakis
Dr. Constantinos Kyriakis, an assistant professor in the College of Veterinary Medicine’s Department of Pathobiology, holds both a doctor of veterinary medicine degree and doctorate in virology and vaccinology.

Dr. Constantinos Kyriakis, left, assistant professor in the Department of Pathobiology in Auburn’s College of Veterinary Medicine, is leading a team of researchers that will soon begin testing SARS-CoV-2 vaccine candidates in swine to determine if the vaccine can trigger the required immune response to combat the novel coronavirus. Pictured, right, is graduate student researcher Fletcher North.
Categories: Health Sciences
Auburn virologist to test potential vaccines that could protect against COVID-19
An Auburn University College of Veterinary Medicine assistant professor, Dr. Constantinos Kyriakis, will soon commence testing of new vaccine candidates that could offer protection against COVID-19 and help prevent the spread of the novel coronavirus.
Working with Professor Ted Ross, director of the Center for Vaccines and Immunology at the University of Georgia, Kyriakis will begin animal trials to investigate the immunogenicity of different vaccine doses and adjuvant combinations against SARS-CoV-2, the virus which causes COVID-19. Ross’ research team is designing and generating multiple vaccine candidates as part of global efforts to combat SARS-CoV-2 that has infected more than 1 million people worldwide.
Kyriakis and a team of Auburn veterinary medicine researchers will test the vaccine candidate’s ability to trigger an immune response in swine, when used alone or in combination with other ingredients. These additional ingredients, called adjuvants, are often used in vaccines to help the body create a greater immune response. Identifying the correct combination is vital to the effectiveness of any vaccine.
Having earned both a doctor of veterinary medicine degree and doctorate in virology, Kyriakis’ research has primarily focused on influenza viruses and novel vaccine technologies for more than a decade. In his previous work at the Center for Vaccines and Immunology, he studied immune responses to influenza infection and vaccination in various animal models.
“Mass vaccinations will help build what is known as ‘herd immunity,’ the cornerstone of infectious disease control,” said Kyriakis. “This will not only protect individuals from SARS-CoV-2 infection and reduce virus spread, but it will protect the entire community and, importantly, high risk groups such as the elderly and people with preexisting health conditions.”
Developing and deploying a safe and efficient vaccine against SARS-CoV-2 is paramount to saving lives, yet poses a major challenge for the scientific community. Unlike influenza vaccines, effective and approved coronavirus vaccines do not currently exist for humans. Only limited data are available from experimental vaccines designed to protect against the SARS-CoV-1 and MERS-CoV. These two zoonotic coronaviruses emerged in 2002 and 2013, respectively, causing extensive severe respiratory illness that spread between animals and people. Several experimental vaccines were tested in animal models, but only one was tested in a phase one human clinical trial.
Kyriakis is one of several Auburn veterinary medicine faculty members engaged in work related to the COVID-19 pandemic. Auburn’s veterinary specialists study the linkages between animal and human health in a broad spectrum of fields such as genomics, virology, immunology and epidemiology, and a variety of clinical practices. This intersection of human and animal medicine is vital to the creation and testing of many life-saving medical advances.
“Using reliable animal models allows us to identify target antigens, optimize our vaccine dose and formulation, and select the most promising vaccine candidates for human clinical trials,” said Kyriakis. “These steps are critical in identifying safe, effective vaccines and moving them into production as quickly as possible.”
BY JAYNE HART

Leading a team of researchers, Dr. Constantinos Kyriakis, assistant professor in the Department of Pathobiology in Auburn’s College of Veterinary Medicine, will soon begin testing SARS-CoV-2 vaccine candidates in swine to determine if the vaccine can trigger the required immune response to combat the novel coronavirus.
Categories: Health Sciences
SEC's Auburn Faculty Achievement Award presented to neurological disease researcher Doug Martin
Auburn University College of Veterinary Medicine professor and noted neurology researcher Dr. Doug Martin has been named the recipient of the Southeastern Conference’s 2020 Faculty Achievement Award for Auburn, announced today by the SEC.
Martin, a professor in the college’s Department of Anatomy, Physiology and Pharmacology and the Scott-Ritchey Research Center, will receive a $5,000 honorarium from the SEC, and he becomes Auburn's nominee for the SEC Professor of the Year, who will be selected from 14 nominees representing SEC universities.
“In a conference known for triple-doubles, triple plays and three-peats, Dr. Martin scores big in each of our three-part mission of groundbreaking research, innovative instruction and impactful service,” Auburn President Jay Gogue said. “He personifies the best of Auburn faculty, and we’re grateful for his dedication.”
The SEC Faculty Achievement Awards, created to recognize faculty accomplishments, scholarly contributions and discoveries, were established by SEC presidents and chancellors and are administered by the SEC provosts. The awards were first presented in 2012.
“Through his commitment to pioneering discovery and saving lives, Dr. Martin exemplifies how profoundly Auburn University cares about, invests in and is transforming research to advance our society,” said Provost and Senior Vice President for Academic Affairs Bill Hardgrave. “By inspiring future generations of scholars, Dr. Martin continues to make a difference in the lives of students, both at Auburn and around the world.”
Each recipient of the SEC Faculty Achievement Award must be a full professor at an SEC university, have a performance history of extraordinary teaching and a record of scholarship that is recognized nationally or internationally. Martin’s life-changing research has garnered over $10 million in external funding to Auburn from sources including the National Institutes of Health.
“It is a remarkable and unexpected honor to receive this award,” said Martin, who received his biology degree in 1989 and his doctorate in biomedical sciences in 1999, both from Auburn. “The award signifies the hard work and expertise of my many collaborators and lab members, and I hope to represent Auburn well among the SEC universities.”
Martin has 25 years’ experience in developing therapies for fatal neurologic disorders such as Tay-Sachs disease, Sandhoff disease and GM1 gangliosidosis. He and his colleagues have demonstrated the profound therapeutic effect of engineered viruses as gene transfer agents, dramatically improving the quality of life and lifespan of affected animals. Their results have led to the first-in-human gene therapy clinical trials for children with GM1, currently underway at the National Institutes of Health.
“Our treatment is extremely promising because it has worked well in cats suffering from GM1, and it is delivered by a single IV injection that takes less than an hour,” Martin said. “We hope the therapy helps children as much as it has helped the animals.”
Parents of a child with the disease each carry one copy of the mutated gene, but they do not show signs and symptoms of the condition. Porter Heatherly, the son of Auburn graduates Sara and Michael Heatherly of Opelika, Alabama, was the first known case of GM1 in Alabama and died in 2016 at age 4.
“I have been inspired by heroic families like the Heatherlys and Porter who fought the disease,” Martin said.
In his teaching role, Martin works with numerous veterinary, graduate and undergraduate students. Among his chief accomplishments, he says, is helping to train the next generation of researchers who are shaping a better, healthier world through their own careers.
Martin has served on numerous review panels for the National Institutes of Health and international foundations and he has received many awards, such as the Above and Beyond Award from the National Tay-Sachs and Allied Diseases Association and the Zoetis Award for Veterinary Research Excellence.
He and his wife, and numerous pets, reside in Opelika and he has two step-daughters who live in Phoenix and New York City.
BY CHARLES MARTIN

Auburn Professor Doug Martin has been named the recipient of the Southeastern Conference’s 2020 Faculty Achievement Award for Auburn. He and colleagues developed a gene therapy treatment for GM1 gangliosidosis that is in clinical trials at the National Institutes of Health.
Categories: Health Sciences, Auburn In the News
Auburn design adapts CPAP machines into emergency ventilators
A team of Auburn engineers has developed a way to quickly and inexpensively convert CPAP machines into ventilators, one of the most important tools hospitals have for helping COVID-19 patients.
Continuous positive airway pressure, or CPAP, machines are commonly used to help people with obstructive sleep apnea breathe more easily during sleep. The Auburn design, called RE-INVENT, is an accessory that would safely repurpose a CPAP into a functional ventilator.
Ventilators are in short supply at hospitals across the nation as the number of patients requiring respiratory assistance due to COVID-19 rises.
Tom Burch and Michael Zabala, faculty in the Samuel Ginn College of Engineering’s Department of Mechanical Engineering, and Hayden Burch, a sophomore in mechanical engineering, initiated the project. Additional engineering faculty and alumni helped refine the mechanical design, control system, user interface and alarms. Critical respiratory care medical professionals contributed to the design of RE-INVENT.
“What started as pure intellectual curiosity quickly grew into an emotional race against time to potentially save lives,” said Zabala, an assistant professor. “We wanted to know if we could design a solution to solve the ventilator shortage problem.”
The RE-INVENT team focused on a design that would reliably ventilate a patient for an extended period. They also considered affordability and ease of manufacture given the urgent, national need for ventilators. The device can be assembled in as little as four hours using approximately $700 in readily available component parts in addition to a standard CPAP machine. A ventilator typical in many hospitals costs as much as $25,000, often more.
“I use a CPAP machine, and it does 90 percent of what a ventilator does,” said Burch, who initially proposed incorporating continuous positive airway pressure into the RE-INVENT design.
“These are difficult times,” he said. “Everybody who understands the gravity of the situation wants to do something to help, so it feels good to think you’ve helped with something that may have an impact.”
Auburn officials are exploring options for sharing the design with health care providers and potential manufacturers. The U.S. Food and Drug Administration has provided guidance to health care providers that may allow them to use RE-INVENT to help increase the availability of ventilators and other respiratory devices during the COVID-19 pandemic.
Health care providers interested in collaborating with the Samuel Ginn College of Engineering during the current public health emergency can learn more online about RE-INVENT.
BY JEREMY HENDERSON
Media Contact: Jeremy Henderson, jdh0123@auburn.edu, 334-844-3591
 Michael Zabala and Tom Burch, faculty in the Samuel Ginn College of Engineering’s Department of Mechanical Engineering, and Hayden Burch, a sophomore in mechanical engineering, helped design RE-INVENT, an accessory that would safely repurpose a CPAP into a functional ventilator.
Michael Zabala and Tom Burch, faculty in the Samuel Ginn College of Engineering’s Department of Mechanical Engineering, and Hayden Burch, a sophomore in mechanical engineering, helped design RE-INVENT, an accessory that would safely repurpose a CPAP into a functional ventilator.
Categories: Health Sciences, Engineering, Auburn In the News
Raj Selected as 2020 Sloan Research Fellow
Monika Raj is on a mission to revolutionize the process of researching, diagnosing and treating cancer, with an ultimate goal of saving lives. It’s a drive that recently received $75,000 in funding support as Raj—an assistant professor in Auburn University’s Department of Chemistry and Biochemistry—became the only researcher in the state of Alabama selected into the 2020 cohort of Sloan Research Fellows.
“I am honored to have been selected and am excited for how this support will help advance my lab’s work in improving cancer diagnosis and treatment,” Raj said, adding that the Sloan Research Fellowship is not only valued for its prestige but also for its flexibility in providing research funding support.
The Alfred P. Sloan Foundation awards two-year, $75,000 fellowships to early-career scholars to advance their research in various fields. Winners of the 2020 Sloan Research Fellowships included 126 researchers across eight different fields. Raj was one of 23 chemists selected. The 2020 recipients were chosen from 60 colleges and universities across the United States and Canada.
Raj said it is quite a privilege to be named into a fellowship that through the years has included “many towering figures in the history of science.” Among that list, she said, are such physicists as Richard Feynman and Murray Gell-Mann, and game theorist John Nash. She said that 47 fellows have also received a Nobel Prize in their respective field, and 17 have won the Fields Medal in mathematics. A total of 69 fellows have received the National Medal of Science, and 18 have won the John Bates Clark Medal in economics, including every winner since 2007.
Raj has dedicated her career to discovering new drugs that might stop the progression of, and ultimately cure, such terminal diseases as cancer. In her lab, she is assisted by a postdoctoral researcher and a combination of graduate and undergraduate students, developing new chemical reactions, catalysis and ligation methodologies of biological molecules. In addition to her research, Raj also teaches biochemistry classes at Auburn.
“I believe that over the next three years, more advancement in cancer diagnosis and treatment will occur than in the past 100 years, and that my research can help achieve these goals,” she said.
Raj’s work has been included in numerous independent and doctoral publications, as well as in books and patents. Her past awards include:
-
A $1.9 million, five-year Maximizing Investigator’s Research Award (MIRA) (R35) from the National Institutes of Health (NIH), National Institute of General Medical Sciences, awarded in 2019
-
An American Peptide Society (APS) Early Career Lectureship in which she presented her work at a symposium in Monterey, California, in June 2019
-
A $650,000 National Science Foundation (NSF) Faculty Early Career Development Program (CAREER) Grant: Secondary Amine Selective Petasis, awarded in 2018
BY MELANIE VYNALEK
 Monika Raj
Monika Raj
Categories: Health Sciences, Auburn In the News
Start-up company licenses Auburn-developed, germ-killing technology
Building on a research career that started in the late 1970s and following on the heels of some 40 patents owned by Auburn University, S.D. Worley is credited with another development that may soon become a commercially available germ-killing technology with multiple applications. This is all thanks to a licensing agreement with a small New York-based firm, Halomine Inc.
Halomine has obtained a license to incorporate Worley’s technology into products of its own, which Halomine Chief Executive Officer Ted Eveleth hopes will be marketed in late this year.
Halomine formed in 2018 with the intent to commercialize an antimicrobial disinfecting spray technology developed at Cornell University. “We found the N-halamine technology, developed by Worley, to be superior to others and we want to incorporate it into our rechargeable, long-lasting antimicrobial product,” Eveleth said.
Halomine entered into the licensing agreement with Auburn in fall 2019 according to Brian Wright, director of commercialization at Auburn’s Office of Innovation Advancement and Commercialization. Halomine has the rights to incorporate Auburn’s technology into their HaloFilm™ products, which will be a rechargeable, long-lasting surface disinfecting spray that has potential in several market areas.
“We are exploring four major market areas,” Eveleth said. “We believe this product can have applications in food safety, healthcare, industrial settings and settings in the home.”
Worley’s contribution is based on N-halamines, compounds containing one or more nitrogen-chlorine covalent bonds. N-halamines provide antimicrobial effects by transferring their positively charged chlorine to appropriate receptors in microorganisms, leading to death of the microbes. In other words, they kill germs by exposing them to an anti-microbial agent.
“I first started my research in this area in 1978 after I came to Auburn,” said Worley, who retired in 2009 and is a professor emeritus in the Department of Chemistry and Biochemistry. Worley has applied the technology to water purification, surface disinfecting, gauze medical bandages, as well as purification and filtration. The technology is based on the development of polymers that contain chlorine, or alternatively bromine, as the disinfecting agent. Worley explains that while both chlorine and bromine are excellent germ-killing agents, their effectiveness does not last long in their basic state.
“By developing various polymers that contain these disinfecting agents, they are capable of holding the antimicrobial properties for a much longer time,” Worley said. “Moreover, they are easily recharged by exposing them to simple household bleach.”
Halomine says their HaloFilm™ can make any surface an antimicrobial surface. By incorporating Auburn’s N-halamine technology, they hope to bring to market a product that not only can effectively kill harmful surface pathogens, but that also lasts longer than presently available products. Once on the market, Eveleth says the product will initially be available through e-commerce channels.
BY MITCH EMMONS
Categories: Health Sciences
Study finds increasing racism linked to cell aging in African Americans
An Auburn University-led study indicates that racism may result in tolls related to premature biological aging among African Americans. African Americans who reported more racial discrimination over a 10-year period showed signs of faster aging at the cellular level during the same time frame.
The study, led by Dr. David H. Chae, an associate professor at Auburn, is the first to examine how changes in racial discrimination are related to changes in telomere dynamics over time. Findings from the study were recently published in Health Psychology.
A common underlying risk factor across many diseases of aging is the length of telomeres—the repetitive sequences of DNA at the ends of chromosomes that protect the cell. Short telomeres increase people’s risks of developing diseases, such as heart disease, stroke, diabetes and dementia. Because telomeres get progressively shorter as people get older, they are considered to be an indicator of cell aging.
“One of the factors that can lead to more rapid telomere shortening is high levels of stress,” Chae explained. “Racial discrimination is a particular type of stress experienced by African Americans that contributes to well-documented health disparities. We investigated one particular mechanism through which this occurs, namely, its impact on the telomere maintenance system.”
Participants in the study were 391 African Americans who were in the Coronary Artery Risk Development in Young Adults, or CARDIA, Telomere Ancillary Study and from Birmingham, Alabama, Chicago, Minneapolis and Oakland, California. Baseline data were collected in 2000 when participants were on average 40 years old and follow-up data were from 2010. At both time points, participants were asked whether they had experienced discrimination in various situations. Most commonly reported were experiences of racial discrimination “on the street or in a public setting,” followed by “at work” and in “getting a job.”
Previous studies on racial discrimination and telomere length have looked at their associations at a single time point, and findings have been mixed. A major strength of this study, according to Chae, was that the investigators “were able to explicitly look at how changes in African Americans’ experiences of racial discrimination over time are directly related to rates of telomere shortening,” thus providing more evidence for a cause and effect relationship between the two.
“We found that greater accumulating experiences of racial discrimination during this midlife period was associated with a faster rate of telomere shortening,” said Chae.
Although the study makes several advances, Chae noted its limitations. The unique characteristics of the CARDIA cohort could limit the generalizability of their findings. Furthermore, there are concerns about the accuracy of retrospective reports of racial discrimination. Chae indicated the need for additional long-term research to study the biological consequences of racial discrimination and their implications for clinical health outcomes.
Despite these caveats, Chae said that their study is important because it “provides compelling evidence for a particular biological pathway through which racial discrimination may drive health inequities.”
He indicated that findings from the study are particularly relevant to the current socio-political climate which is characterized by increasing incidents of racial discrimination.
“Our results point to how racial discrimination, a particular type of social toxin that disproportionately impacts African Americans, becomes embedded at the cellular level,” Chae explained. “Racism continues to be a pressing social and moral dilemma, as well as a public health issue.”
Authors of the “Racial Discrimination and Telomere Shortening Among African Americans: The Coronary Artery Risk Development in Young Adults (CARDIA) Study,” are Chae, Connor D. Martz and Thomas E. Fuller-Rowell, Auburn; Nancy E. Adler, Jue Lin and Elissa S. Epel, University of California, San Francisco; Yijie Wang, Michigan State University; Natalie Slopen, University of Maryland, College Park; Tiffany Yip, Fordham University; Karen A. Matthews, University of Pittsburgh; Gene H. Brody, University of Georgia; Erica C. Spears, University of North Texas Health Science Center; and Eli Puterman, University of British Columbia–Vancouver.
The study was supported by grants from the National Institute on Aging and the National Heart, Lung and Blood Institute.
BY AMY WEAVER
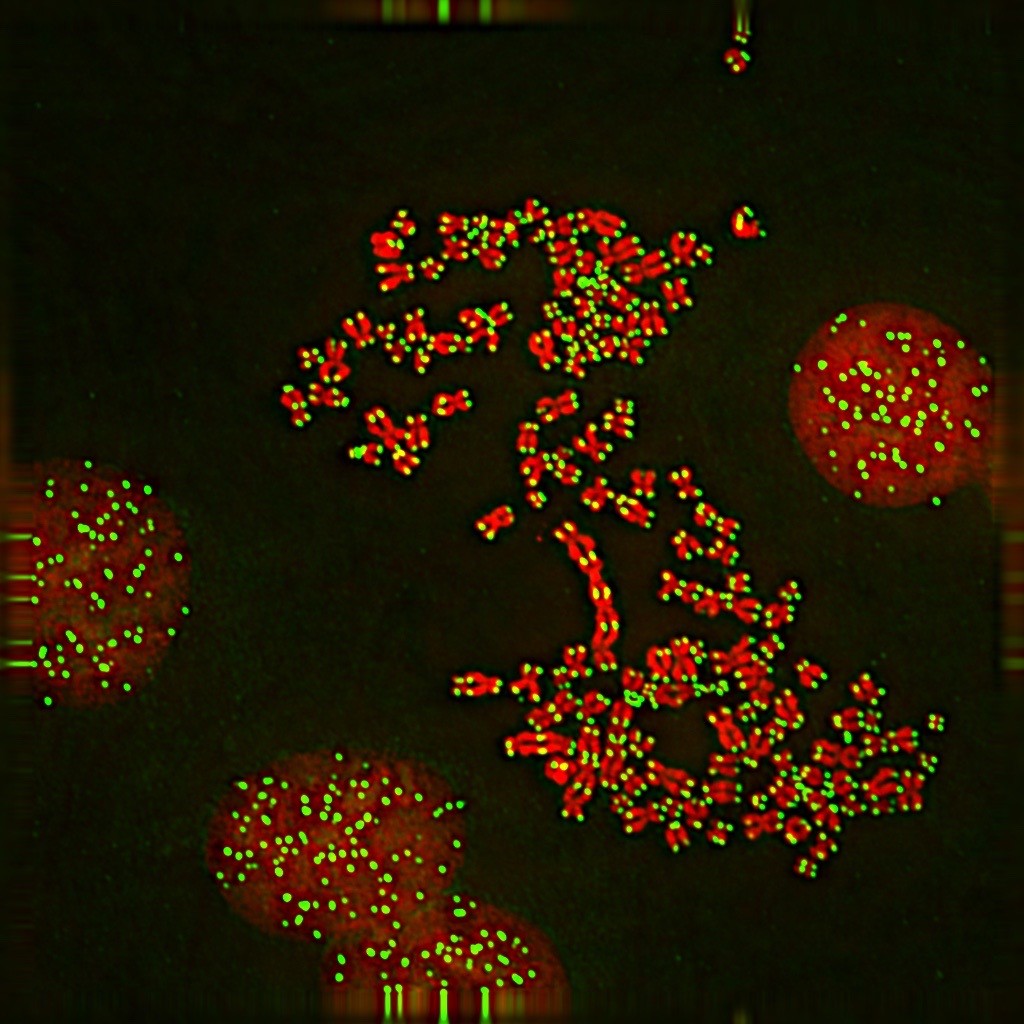
Telomeres are DNA caps that protect chromosomes. The length of telomeres reflects cell aging. (Image source: UCSF)
Categories: Health Sciences
Auburn sleep expert offers advice on better sleep
Mona El-Sheikh is the Leonard Peterson Inc. Professor in the Department of Human Development and Family Studies in the College of Human Sciences at Auburn. She is world renowned for her research on sleep and adolescents’ development. El-Sheikh has been on faculty at Auburn since 1990, first in the Department of Psychology and then the Department of Human Development and Family Studies. Between falling back an hour in November for daylight saving time and people making quality sleep a goal in 2020, El-Sheikh shares her expertise.
With the recent time change making night come earlier in the winter day, how are people to cope and get into a new rhythm for proper sleep?
Related to the regularity suggestion, our bodies function best with a regular rhythm of sleep and wake periods. When traveling across several time zones, we experience jet lag. Adapting to changes to and from daylight savings time is a case of mini jet-lag. A one-hour change does not disrupt one’s circadian cycle drastically, but some people are affected more than others. If it has taken you several days to adapt to changes in the past, one thing you can do is set your own schedule to go through the change more gradually. Let’s say you routinely go to bed at 10 p.m. In the fall, time “falls back” one hour, but you may not feel ready to sleep at the new 10 p.m., which your body is sensing as only 9 p.m. You could try to go to bed a few minutes earlier in the days leading up to the change. For jet lag, the recommendation is to expose yourself to early morning light to reset your circadian cycle. If you routinely get up at 7 a.m., that was the time of sunrise in Auburn on Nov. 2. The next day, the sun rose at 6 a.m., so to get as much early morning light, you would need to get up a few minutes earlier over the preceding days. Times of morning light and twilight establish our body’s diurnal cycle. Adapting our sleep and wake schedules to those times are the keys to coping with the changes.
What advice or tips would you recommend for people who want to get better sleep in the new year and maintain it through 2020?
Every January, many individuals make resolutions for the upcoming year. These typically have to do with improvements they want to make related to their health and well-being. A resolution for improving sleep habits is one that many ought to consider. The overall goal is to make improvements in sleep habits that improve sleep duration, quality and regularity. Examples of specific goals are: (1) Establish a bedtime early enough to get sufficient sleep; (2) Decrease or eliminate caffeine and other stimulants especially during the afternoon and evening; (3) Evaluate and improve the bedroom environment. Are your pillow and bedding comfortable? Are you able to keep the temperature and humidity at a comfortable level? Is your bedroom dark and quiet enough?; (4) Decrease the frequency and duration of activities before bedtime that interfere with getting to sleep like watching TV or using social media; (5) Establish and maintain a relaxing bedtime routine. Changing sleep habits can be monitored and tracked with sleep diaries that can be found on the National Sleep Foundation website or ones that you can custom make for yourself.
What does your sleep research involve?
The core of my research mission is to understand factors that contribute to positive and negative outcomes in children, adolescents and young adults. We focus on several domains of outcomes, including cognitive functioning and academic achievement, behavioral and emotional problems and physical health. Ultimately, the knowledge that we gain will be used to help prevent problems in those domains or at least mitigate the damage caused by them.
What have you learned from your research?
My projects have involved studying several large groups of different families from the community and following them over the course of many years (ages 7–23 years). We have been able to identify which factors present in childhood are related to problems that occur later in development. While there are many factors earlier in life that have been historically been found to relate to problems later on, we have discovered that the amount, quality and regularity of sleep play critical roles in either increasing risk of problems or protecting against those problems. One of our important discoveries is that poor sleep is especially associated with negative outcomes in children and adolescents in families of lower socioeconomic position. Conversely, when children and adolescents in those families get sufficient sleep, their good sleep serves as a protective factor against those negative outcomes.
What advice do you have for children? For adults?
Our work, along with a large body of research by others, indicates that improving sleep has significant benefits. Improving sleep should help children and adolescents perform better academically, have better emotion regulation and better health. Improving sleep, like improving people’s nutrition and exercise, requires a multi-pronged approach. One area we emphasize is for parents to assess the quality of the physical environment for sleep. Ideally, it needs to be a place where one feels safe and secure, is quiet and dark, with a comfortable temperature and humidity. Besides the physical environment, we stress the importance of parental monitoring of such things as screen use in the evenings, consumption of caffeinated drinks and providing a regular comforting bedtime routine. Going to bed early enough to get sufficient sleep is important, especially for children and adolescents on school nights. And one recommendation deriving from our research is that regularity of bedtimes and wake times during the school week and even on weekends are extremely important. These suggestions apply equally to adults.

Mona El-Sheikh
Categories: Health Sciences
Auburn researcher receives $1.9 million grant for rapid immune diagnostics
An Auburn Engineering faculty member has received a $1.9 million National Institutes of Health grant – the largest NIH grant the Samuel Ginn College of Engineering has ever received.
The grant will support Pengyu Chen, assistant professor of materials engineering, in his project to develop next-generation, rapid diagnostic tools for the health care industry.
For doctors, having real-time data on the health and function of a patient’s immune system is critical to treating cancer and autoimmune diseases. However, one of the main diagnostic tools in use today, the enzyme-linked immunosorbent assay, must be sent to a lab and takes hours to days for results to return.
By then, the dynamics of the immune system may have completely changed, leaving the clinician to make treatment decisions based on outdated information.
Chen is aiming to change that by developing optofluidic nanoplasmonic biosensors for rapid analysis of the immune system. The research study seeks to better understand and measure cytokines – tiny proteins vital to signaling between cells – for rapid diagnostics.
“The ultimate goal is to develop a biomedical device based on nanoparticles that we can use to take one droplet of the patient’s blood and, in a short period of time, we can accurately tell if the patient’s immune system is healthy or not,” Chen said.
The research project has three primary goals: to integrate nanoplasmonic structures into biosensors for higher performance and faster response time; to fabricate microfluidic devices for target cell isolation and on-chip measurements and analysis; and to develop nanoplasmon ruler biosensors – two nanoparticles linked with one DNA – to visualize cytokines secreted from a single immune cell and eventually map out its secretion profile. Previous research suggests that measuring cytokine-based immune fingerprints provides useful information related to infectious diseases, cancer and other diseases.
“We are trying to provide real-time feedback of the immune system for personalized immunomodulatory therapies,” Chen said. “Currently, there is no technology that can serve as a real-time diagnostic tool to tell if the dosage and timing of a therapy is good or not. Our hope is that we can develop a point-of-care technology that can be used at bedside so that physicians can make decisions based on these measurements more quickly and accurately, and then potentially change the outcome of the therapeutics.”
The grant is funded through the NIH’s R35 Maximizing Investigators' Research Award for Early Stage Investigators program. The five-year grant will allow Chen to hire up to three doctoral students and two postdoctoral researchers to assist with the study.
BY CHRIS ANTHONY
WEB.jpg)
Pengyu Chen, PhD, assistant professor of materials engineering
Categories: Health Sciences, Science, Technology, Engineering and Mathematics (STEM)
Pharmacy researchers find mom’s marijuana use may impair baby’s memory
Auburn University Harrison School of Pharmacy researchers have found more and more expectant mothers are turning to marijuana and subsequently putting their baby’s memory at risk.
With a recent report claiming the number of women using marijuana during pregnancy had doubled in the last 15 years, Auburn doctoral student Priyanka Pinky sought to examine what effect it would have on the developing baby.
A medical doctor from Bangladesh, Pinky studied tetrahydrocannabinol, or THC—the active ingredient in marijuana—on rodent models to see what effect there was on the offspring’s memory. Pinky served as the lead graduate student on the project, under the direction of Drs. Vishnu Suppiramaniam and Miranda Reed, and assisted by fellow graduate students Jenna Bloemer, Yifeng Du, Sharay Setti, Ryan Heslin and Warren Smith.
The research team administered THC to pregnant rodent mothers and found that THC could cross the blood placental barrier—meaning it could transfer from the mother’s blood to the baby—and subsequently impact the growing fetus.
“Research in our lab has shown that using marijuana during pregnancy has long-lasting effects on learning and memory and it can continue throughout adolescences,” said Pinky.
The team conducted several behavioral experiments and observed the young offspring to be forgetful.
“They could not perform the given task as efficiently as normal offspring of the same age,” Pinky explained. “This made us to think ‘what is the reason behind this?’ We investigated further in the molecular level and we identified the culprit.”
The Neural Cell Adhesion Molecule—a protein in the brain—works like an adhesive, maintaining the connection between neurons in the brain’s hippocampus, where memories are formed. The adhesive connection facilitates the formation of memory and keeps memory intact.
“We found that this protein is significantly reduced in the brain of the THC-exposed animals,” said Pinky. “Since there is reduced adhesion between neurons, memory is impaired.”
Why pregnant women?
Suppiramaniam and Reed have extensive experience in prenatal research and expected THC to have deleterious effects on the brains of the offspring.
“This study is timely because marijuana use among pregnant women is increasing,” Suppiramaniam said.
Reed said the popularity among pregnant women could be because “everybody’s talking about legalizing.” To date, 33 states and the District of Columbia have legalized the drug in some form, making it more accessible to the masses.
A 2018 study out of Colorado—where recreational marijuana has been legal since 2014—found the majority of Colorado dispensaries—69 percent—recommended pot as treatment for morning sickness.
Whether it’s to cope with morning sickness or not, “a lot of people assume it’s okay to smoke during pregnancy,” Reed added, especially if they hear a baby was born with no deficiencies.
Suppiramaniam said it’s difficult to counteract the culture because the mothers “assume it can’t be passed on” to the fetus.
While smoking marijuana is the most prevalent method of consumption, it can also be eaten in tasty edible form, such as gummy bears and chocolates. Reed said some people—such as pregnant women—likely think an edible is less harmful than smoking a joint.
Maybe it makes sense to these expectant mothers since marijuana reportedly helps cancer patients cope with the side effects of the disease and its treatment.
But, medical experts have claimed for decades that smoking cigarettes and drinking alcohol are detrimental to the health and well-being of the baby. How could marijuana be an exception? Experts say it’s not.
The American Medical Association demands that taking marijuana during pregnancy is dangerous, and the American College of Obstetricians and Gynecologists discourages pregnant women from using marijuana and other substances.
The Auburn researchers certainly agree that the potential threats to a growing fetus are far too high, yet they have more work to do.
Suppiramaniam said they hope to do more extensive research once a 5-year grant from the National Institutes of Health begins this fall.
Pinky has presented the study findings at the Society for Neuroscience annual meeting—the largest conference for neuroscience in the world—and during the 2019 Experimental Biology meeting of the American Society for Pharmacology and Experimental Therapeutics annual meeting.
BY AMY WEAVER
---
Auburn University's Harrison School of Pharmacy is ranked among the top 20 percent of all pharmacy schools in the United States, according to U.S. News & World Report. Fully accredited by the Accreditation Council for Pharmacy Education (ACPE), the School offers doctoral degrees in pharmacy (Pharm.D.) and pharmaceutical sciences (Ph.D.) while also offering a master's in pharmaceutical sciences. For more information about the School, please call 334.844.8348 or visit the Harrison School of Pharmacy website.

Priyanka Pinky, a doctoral student in Auburn University’s Harrison School of Pharmacy, has found that expectant mothers who turn to marijuana to combat morning sickness are harming their baby’s memory.
Categories: Health Sciences
Auburn University study on viruses spread by outdoor domestic cats drawing national attention
An Auburn University study on viruses spread by cats is gaining national attention after it showed that cats allowed to roam freely outdoors are 2.77 times more likely to have parasitic infections than indoor-only cats.
The study, “Who let the cats out: A meta-analysis on risk of parasitic infection in indoor versus outdoor domestic cats (Felis Catus),” appeared in the April 17 Biology Letters scientific journal and has been covered by major outlets such as The New York Times.
Kayleigh Chalkowski, a doctoral student in the School of Forestry and Wildlife Sciences, led the study.
“I was pretty excited,” Chalkowski said. “Academic research is frustrating sometimes. You stare at a computer screen and work through coding errors and data streamlining issues for hours on end, and it feels like the work, in some parts of the process, isn't going to have any real impact.
“I'm very happy to know that my research is getting out there, but even more so the important message that cats—even a pet cat at home—can serve as a parasite reservoir and threaten human and wildlife health.”
Chalkowski’s co-authors were Associate Professor Sarah Zohdy and Professor Christopher Lepczyk, her advisors at the School of Forestry and Wildlife Sciences, and Associate Professor Alan E. Wilson of the School of Fisheries, Aquaculture and Aquatic Sciences.
Wilson is also pleased with the paper’s international impact.
“I think the best part of this is that it’s a student project,” he said. “To take a project, publish it and then have so much interest around the world—I don’t think I’ve ever seen a student publish a paper that’s had an impact so quickly.
“That has really blown me away, and I hope Kayleigh is enjoying this. What she showed in her data really resonates with people. People are crazy about their animals.”
Chalkowski said the group sought to quantify the effect of parasitic infection in indoor cats as compared to outdoor cats because of the potential of pet cats to transmit parasites to humans and surrounding wildlife. The research is the first of its kind.
“Cats are an underappreciated reservoir of infectious pathogens, and we saw a useful dichotomy in cat ownership—free-roaming outdoor access vs indoor-only—that we thought is important to quantify,” Chalkowski said. “Although it’s widely understood that keeping cats indoors prevents other obvious risks like getting run over by cars, the effect of indoor/outdoor on parasitic infection hadn't been quantified yet on a broad scale of geographic locales and pathogen types.”
School of Forestry and Wildlife Sciences Dean Janaki Alavalapati said the international attention the study has garnered is significant.
“Because this research addresses aspects of a commonly debated topic, it can serve as a guide for cat owners who may not have realized the serious health risks inherent in allowing their cats to roam outdoors,” Alavalapati said.
“This meta-analysis is part of an ongoing study that is likely to yield even more insights on this subject.”
In the study’s acknowledgements section, the authors thanked the Auburn School of Forestry and Wildlife Science SQUAD, or Solving Quantitative, Unusual and Awesome Dilemmas, Auburn professors Todd Steury of the School of Forestry and Wildlife Sciences, Ash Abebe of the Department of Mathematics and Statistics and Biology and Forestry and Wildlife Sciences and Math Librarian Patricia Hartman.
WRITTEN BY TERI GREENE

Auburn University School of Forestry and Wildlife Sciences doctoral student Kayleigh Chalkowski takes samples of soil-borne parasites at a cat colony feeding site in the U.S. Virgin Islands.
Categories: Health Sciences
Nearly 600 Auburn students showcasing their research and creativity April 9 at Auburn Research Student Symposium
Nearly 600 Auburn University students with a flair for research and creativity will showcase their talents when they gather for the annual Auburn Research Student Symposium.
With projects ranging from chemical engineering to plant pathology to architecture and design, the symposium on April 9 will provide Auburn and Auburn Montgomery students an opportunity to share their discoveries university-wide. The daylong event will take place in the Student Center.
Undergraduate and graduate students from almost every department have registered to participate through posters, oral presentations and creative scholarship displays. Approximately 400 of the young researchers will present posters and displays more than 180 will give 10-minute talks, all under the watchful eyes of judges who will award top honors in a variety of university-wide and college-specific categories.
An awards ceremony and reception will be held April 18 at 5 p.m. in the Student Center ballroom. The keynote speaker will be Michael Zabala, assistant professor of mechanical engineering, who earned his bachelor’s degree at Auburn in 2007.
Steve Taylor, chair of the Research Symposia Committee and associate dean for research in the Samuel Ginn College of Engineering, said, “Our students’ innovative research covers many areas, from projects in STEM disciplines [science, technology, engineering and mathematics] to the arts and humanities. They are working with our world-class faculty on life-changing projects that could shape new developments in many fields.”
Following the April 9 symposium, Nobel Laureate in Chemistry George P. Smith will visit Auburn University and the College of Veterinary Medicine April 10-11. Professor Smith will present a public lecture at 2 p.m. April 10 in The Hotel at Auburn University and Dixon Conference Center auditorium, which will be followed by a reception. On April 11, he will be available to meet with faculty and students at the College of Veterinary Medicine.
A fall event, the Auburn Research Faculty Symposium, will be held in September to recognize faculty excellence in research and creative scholarship.
More information about the student symposium is available at www.aub.ie/researchstudentsymposium or by contacting Taylor at taylost@auburn.edu.
WRITTEN BY CHARLES MARTIN
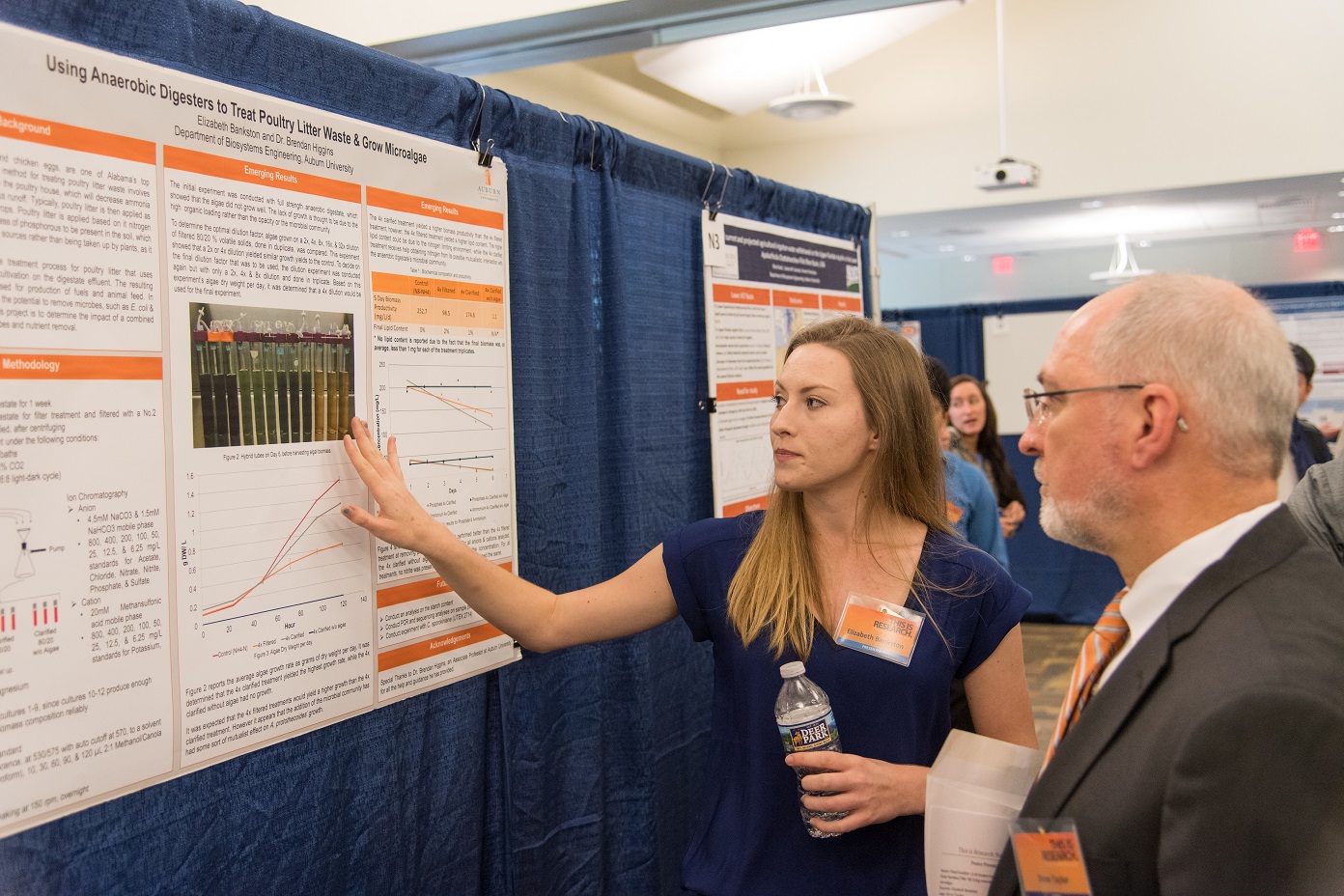
Auburn students with a flair for research and creativity will showcase their talents when they gather April 9 in the Student Center for the annual Auburn Research Student Symposium. Pictured, student Elizabeth Bankston discusses her research poster with Steve Taylor, chair of the Research Symposia Committee, at last year’s symposium.
Categories: Health Sciences, Cyber, Energy & the Environment, Transportation, Food Systems, Security, Engineering, Creative Scholarship
Auburn University achieves research milestone with ‘R1’ Carnegie classification
In another affirmation of its drive forward to excellence, Auburn University achieved a research milestone Monday - being elevated to an “R1” institution by the Carnegie Classification of Institutions of Higher Education.
The announcement follows a concerted effort by Auburn to elevate its commitment to life-saving research, beginning with an announcement by Auburn President Steven Leath in December 2017 and subsequent awarding of $5 million for three years toward the Presidential Awards for Interdisciplinary Research, or PAIR. An R1 designation by Carnegie is reserved for doctoral universities with the highest levels of research activity.
Among 120 institutions to receive the R1 designation Monday, Auburn was listed in the top 100 of such universities, raising its classification from an already lofty “high research” R2 classification to Monday's “very high research activity” R1 label.
“This tremendous designation acknowledges the hard work involved in the pioneering discoveries happening at Auburn every day,” said Leath, who was recently named one of seven new members appointed by President Trump to the National Science Board, a policy-making body of the National Science Foundation. “We are grateful to the university’s faculty and staff, especially Graduate School Dean George Flowers, for their unwavering commitment to elevating Auburn’s profile as a world-class academic institution.
“Auburn is on the move, and this prestigious distinction recognizes Auburn’s critical role in creating new knowledge and helping others live better lives.”
Universities considered for the R1 designation must have awarded at least 20 research/scholarship doctoral degrees and had at least $5 million in total research expenditures, according to Carnegie’s classification website. Auburn has grown its research efforts in both STEM and non-STEM areas, furthering its institutional commitment to offer solutions to real-world problems and grow its reputation as a go-to university in providing results that transform and inspire.
“Auburn University is known for its innovative and transformational research, and receiving the R1 classification is a significant accomplishment,” said Jennifer Kerpelman, interim vice president for research. “This classification recognizes the dedication, commitment and hard work of Auburn’s faculty and student researchers across all disciplines.”

Dr. Amal Kaddoumi, left, a professor in Auburn’s Department of Drug Discovery and Development, works in a lab with graduate research assistant Sweilem Al Rihani. Kaddoumi is leading a multi-disciplinary team in an investigation of oleocanthal, a molecule that appears naturally in extra-virgin olive oil, as a novel preventative treatment for such diseases as Alzheimer’s or dementia.
Categories: Health Sciences, Cyber, Energy & the Environment, Science, Technology, Engineering and Mathematics (STEM), Transportation, Food Systems, Engineering, Auburn In the News, Creative Scholarship
Auburn, partner organizations sign agreements for additive research centers
Auburn University, ASTM International and other partner organizations on Monday celebrated the launch of two new centers of excellence in additive manufacturing aimed at accelerating research and development, standardization and innovation in that field, also known as 3-D printing.
Global standards developer ASTM International launched its Additive Manufacturing Center of Excellence with Auburn University, NASA, manufacturing technology innovator EWI and the UK-based Manufacturing Technology Centre. Auburn and NASA also formally launched the National Center for Additive Manufacturing Excellence.
ASTM International President Katharine Morgan said, “The synergy among EWI, MTC, Auburn and NASA will help fill the gaps in technical standards that this industry needs to drive innovation. As a result, we’ll empower industries that are eager to apply additive manufacturing to aerospace, auto, medical and more.”
AMCOE’s advisory board comprised of U.S. and international public and private sector leaders met for the first time today while other meetings involved research and development as well as education and workforce development teams. The events come on the heels of AMCOE’s international launch on July 13 at the MTC, where European industry and government officials gathered to celebrate this initiative.
Auburn University President Steven Leath said, “Auburn is committed to growing research, solving real-world problems and establishing partnerships that support these transformative initiatives, such as our thriving additive manufacturing program. By investing in skilled researchers and first-rate facilities, we aim to drive additive technology forward and unleash its full potential. We look forward to continuing to work with our industry and government collaborators.”
Auburn University is in the final stage of renovations to the Gavin Engineering Research Laboratory, which will in part house additive manufacturing research funded through the centers.
Auburn was selected for the two research partnerships in March.
Media Contact: Chris Anthony, chris.anthony@auburn.edu, 334.844.3447

Components made through additive manufacturing are shown in the additive manufacturing lab in Wiggins Hall at Auburn University.
Categories: Health Sciences, Transportation, Engineering, External Engagement
Presidential Awards for Interdisciplinary Research (PAIR) Announced
Auburn research teams are tackling local and global challenges ranging from housing affordability to advanced manufacturing of medical implants, thanks to a new $5 million investment in 11 groundbreaking projects designed to deliver practical, life-changing solutions.
“Auburn research is on the move,” said Auburn President Steven Leath. “Our world-renowned faculty are leading Auburn in our drive to solve problems, provide real-world benefits and serve the social good.”
Today’s announcement is part of an initiative funded through the Presidential Awards for Interdisciplinary Research, or PAIR, that Leath created last year to propel Auburn to new levels of research and development distinction. The PAIR funding will span three years. Additional research topics include rural health disparities in poverty-stricken areas, treating the hallmarks of Alzheimer’s disease, neuroscience research and graduate education, reducing carbon dioxide emissions or using them for other means, and other critical areas of human and environmental health.
Project teams were selected from three award tiers: Tier 1 for new teams, with funding up to $100,000 per year; Tier 2 for established teams, with funding up to $250,000 per year; and Tier 3 for high-impact teams, with funding up to $500,000 per year. All proposals received an in-depth evaluation from Auburn’s associate deans for research, and Tier 3 proposals were also externally evaluated. Top-evaluated proposals were those that most closely aligned with the goals of PAIR as stated in the program guidelines. From 101 proposals received, 11 project teams will receive funding (the two top-evaluated proposals per tier for up to three years of funding, as well as five additional, top-evaluated Tier 1 proposals for two years of funding with a third-year no-cost extension available).
Project teams to receive funding are:
Project: Creating better bio-medical implants for patients in need using additive manufacturing, or “3D Printing” (Tier 3; $1,275,000 total funding over three years)
The issue: Auburn researchers plan to develop improved implants/orthotics for those with neuromuscular and skeletal system needs through the process of additive manufacturing. This process, also known as “3D printing,” allows for more customizable implants for small animals and humans and the possibility of embedded drugs in implants to ward off infections that can sometimes follow implant surgeries.
The Auburn solution: Research will take place to ensure “3-D printed” biomedical implants will remain durable during use and conform well to a patient’s needs while serving as a reliable drug-delivery source that can offer injury-triggered pain relief. The additive manufacturing process also helps reduce implant production costs.
Project: Unlocking Home Affordability and Prosperity in Rural America (Tier 3; $1,275,000 total funding over three years)
The issue: Auburn researchers are focusing on helping those in poor, rural areas gain greater access to resources that will ultimately lead them to finding affordable housing options.
The Auburn solution: Auburn researchers will work toward the creation of a National Institute of Rural Prosperity that will foster partnerships to help rural residents more easily overcome barriers to home ownership, including mortgage lending, home insurance and local ordinances and policies.
Project: Reducing the burden of neurological disease by increasing fundamental knowledge about the brain and nervous system (Tier 2; $637,500 total funding over three years)
The issue: Auburn researchers will work to mitigate against mental, neurological and substance use disorders, which make up a substantial proportion of the world’s disease burden.
The Auburn solution: A team of experts in chemistry, physiology, development, degeneration, and imaging of the brain will collaborate to develop a neuroscience center to increase fundamental knowledge about the brain and nervous system and to use that knowledge to reduce the burden of neurological disease.
Project: A Mobile Mitochondria Laboratory (AU MitoMobile) to Lead the World in Measuring Bioenergetics in Natural Settings (Tier 2; $636,941 total funding over three years)
The issue: Because the successful study of genetic and environmental impacts on mitochondria (the energy-providing part of the cellular makeup of plants and animals) can be severely limited in a laboratory setting, Auburn researchers will collaborate to build a mobile laboratory to bring this research to field sites.
The Auburn solution: A team of evolutionary biologists, environmental biologists, exercise physiologists and engineers will develop a mobile laboratory for measuring mitochondrial energy production of vertebrates at remote locations, such as oil spill sites and other places where environmental disturbances have damaged the health of local wildlife.
Project: Rural African American Aging Research (Tier 1; $255,000 total funding over three years)
The issue: Auburn researchers will assess the psychosocial stressors that can contribute to the problem of rural African Americans having a lower life expectancy and a faster progression of age-related diseases. Research in this area has the potential to inform health-promoting interventions and polices and lead to health and social equity.
The Auburn solution: PAIR funding will be used to establish a sustainable research structure in east-central Alabama focused on improving health in that community and beyond by partnering with surrounding communities. The ultimate goal is to grow the scientific knowledge of how psychosocial risk factors can accelerate aging among African Americans.
Project: Reducing and reusing carbon dioxide emissions for useful means (Tier 1; $255,000 total funding over three years)
The issue: Auburn researchers seek to combat the dire environmental effects of carbon dioxide emissions through a plan to reduce such emissions and store or utilize them for other useful means.
The Auburn solution: Researchers will work toward the development of an Alabama CO2 Utilization and Storage Center at Auburn University, with a goal of establishing Auburn as a leader in carbon dioxide utilization and storage research focused on best ways to capture CO2 emissions and convert them into helpful forms such as green fuels.
Project: Extra-virgin olive oil examined for uses in treating hallmarks of Alzheimer’s (Tier 1; $150,000 total funding over two years)
The issue: Auburn researchers are examining the consumption of extra-virgin olive oil for its potential to have a positive effect on the disease hallmarks of Alzheimer’s Disease. The research team is seeking to conduct more research into this area to determine the viability of findings for humans.
The Auburn solution: A multidisciplinary team will be assembled to conduct a pilot study on the positive effects of extra-virgin olive oil and to produce data for a strong human clinical trial to be submitted to funding agencies.
Project: Drugs from Dirt: Development and Characterization of Novel Antimicrobial Compounds (Tier 1; $150,000 total funding over two years)
The issue: Because many disease-causing organisms are resistant to current drug therapies, Auburn scientists are pursuing new approaches to the development of antibiotics.
The Auburn solution: Researchers will test and develop new therapeutic strategies for treating infectious diseases, through the study of antiobiotic-producing bacterial cultures they have discovered in soil. These are potentially life-saving antibiotics that could have application in human medicine, agriculture, and veterinary practice.
Project: Creating a Climate Information System to aid in planning for climate-related disasters (Tier 1; $150,000 total funding over two years)
The issue: Auburn researchers will create a climate service model that will help guide decision making in planning for climate-related disasters that can cause great economic and social damage.
The Auburn solution: A cross-disciplinary team of investigators will develop a science-based, Unified Climate Information System to better inform planning, policy and practices at regional, national and global scales. In addition to exploring emerging climate data, the research will seek to improve and integrate impact models for water quantity, water quality, crop growth and disease transmission simulations. The project also will include the creation of an interactive website platform, with all work being focused on the southeastern U.S. and being easily adaptable to other locations worldwide.
Project: Emerging Contaminants Research Team (Tier 1; $150,000 total funding over two years)
The issue: Auburn experts are conducting research into newly recognized environmental contaminants, such as per- and polyfluoroalkyl substances, which have not been studied sufficiently to determine their impact on the environment and their possible health risks to humans and wildlife.
The Auburn solution: This Auburn research team will use its expertise in civil engineering, pharmacology, aquatic sciences, and other key areas to collaborate on focused research into the effects of these and other previously understudied contaminants, to increase knowledge and public awareness of risk factors.
Project: Development of the AU-NASH Research Program (Tier 1; $150,000 total funding over two years)
The issue: Auburn researchers are seeking solutions to the problem of nonalcoholic steatotic hepatitis, or NASH, the most severe form of non-alcoholic fatty liver disease and perhaps the most significant form of chronic liver disease in the world today, which has no current approved therapies available.
The Auburn solution: The research team will work to address this urgent, unmet medical need by developing a disease therapy program to increase positive outcomes for those suffering from liver disease.
For more details on each PAIR project and how Auburn is inspiring as a leading provider of life-changing research, creative scholarship and community engagement, visit auburn.edu/auburninspires.
BY JONATHAN CULLUM AND PRESTON SPARKS
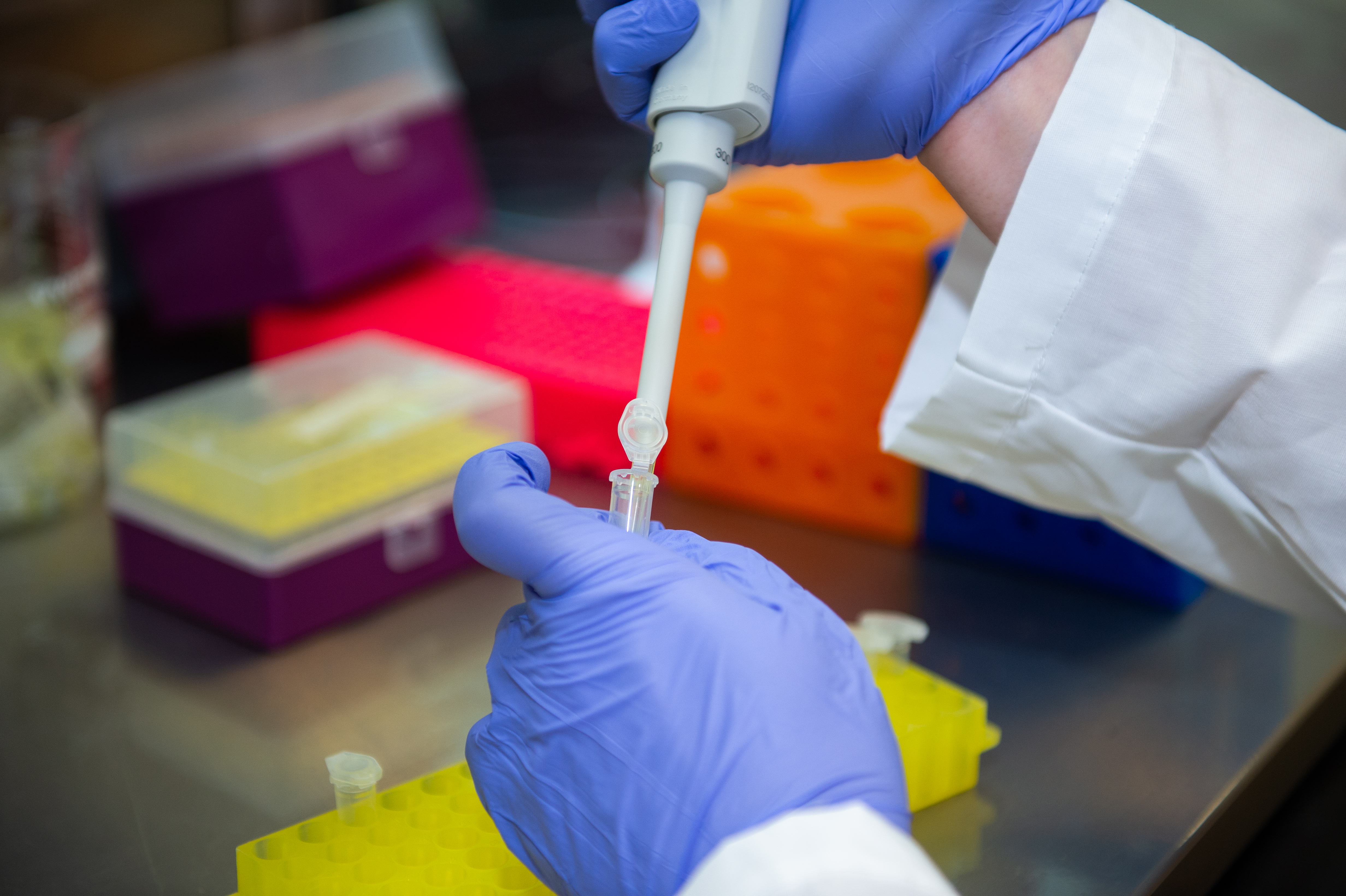
Categories: Health Sciences, Energy & the Environment, Science, Technology, Engineering and Mathematics (STEM), Food Systems, Engineering
Auburn’s College of Veterinary Medicine conducting clinical trial on new melanoma drug
Dogs, like their human companions, can be susceptible to skin cancer, and the Oncology Service at Auburn University's College of Veterinary Medicine could use the help of man's best friend in launching a clinical trial to test a new melanoma treatment drug.
"This study is designed to test a new drug that may be useful in treating melanoma, or skin cancer, which most commonly occurs in the mouth in dogs," said Dr. Bruce Smith, a professor in the Department of Pathobiology and director of the Auburn University Research Initiative in Cancer, or AURIC.
"The drug, called MMX, is a peptide, which is a chain of amino acids, the basic building blocks of all proteins," Dr. Smith said. "This study seeks to measure the effect of this drug on these tumors. We are currently taking patients to participate in the clinical trial."
Dog owners who are interested in enrolling their pets into this clinical trial must do so through the Oncology Service at the college's Wilford and Kate Bailey Small Animal Teaching Hospital.
They can be referred by their primary veterinarian, according to Dr. Smith. The treatment, as well as surgery to remove any tumor left at the end of the trial, will be provided at no cost to the owner.
The trial initially is about a five-week program, Dr. Smith said. It involves the dog owner bringing the animal in for an initial evaluation.
"The melanoma is measured, the drug is administered, and we begin a series of treatment and monitoring the tumor to measure its response," Dr. Smith said. "The dog will need to visit Auburn weekly for five weeks. In addition, owners will administer the peptide daily at home and keep a logbook about their dog while it is being treated."
Dr. Smith said this drug is not chemotherapy, but rather, a protein-based medication that has been tested on dogs in a clinical setting with no known side effects.
"It appears to act quickly to shrink the tumors," Dr. Smith adds. "It has been under testing in a clinical setting for about 10 years and now, it is ready to be tested for FDA approval."
Dog owners who believe their pet might be a candidate for participating in this clinical trial can contact the Oncology Service at the Bailey Small Animal Teaching Hospital at 334-844-6000. More information about this clinical trial can be found on the Oncology Service website.
The study is an example of Auburn faculty working toward life-changing solutions to meet pressing global health issues.
BY MITCH EMMONS
 The Oncology Service at the Auburn University College of Veterinary Medicine is launching a clinical trial to test a new melanoma treatment drug for dogs. Dr. Annette Smith, left, the Robert and Charlotte Lowder Distinguished Professor in Oncology with the Department of Clinical Sciences, and Dr. Bruce Smith, a professor in the Department of Pathobiology and director of the Auburn University Research Initiative in Cancer, or AURIC, are shown with a canine patient in an exam room at the Wilford and Kate Bailey Small Animal Teaching Hospital. (Photo by Mitch Emmons)
The Oncology Service at the Auburn University College of Veterinary Medicine is launching a clinical trial to test a new melanoma treatment drug for dogs. Dr. Annette Smith, left, the Robert and Charlotte Lowder Distinguished Professor in Oncology with the Department of Clinical Sciences, and Dr. Bruce Smith, a professor in the Department of Pathobiology and director of the Auburn University Research Initiative in Cancer, or AURIC, are shown with a canine patient in an exam room at the Wilford and Kate Bailey Small Animal Teaching Hospital. (Photo by Mitch Emmons)
Categories: Health Sciences
El-Sheikh receives 2017 Research and Economic Development Advisory Board Advancement of Research and Scholarship Achievement Award
At its recent fall meeting, Auburn University’s Research and Economic Development Advisory Board presented Dr. Mona El-Sheikh, a professor in the College of Human Sciences, with the 2017 Research and Economic Development Advisory Board Advancement of Research and Scholarship Achievement Award. The award recognizes El-Sheikh’s contributions to public health, and particularly to sleep research, over the course of her 27-year career at Auburn.
Composed of more than 40 industry professionals from across the country who actively support Auburn’s research efforts, the board established the award in 2014 to recognize significant research and scholarly activity that exemplifies and advances Auburn’s research and scholarship mission. The recipient of the annual award receives a $25,000 grant to further his or her research.
“I am thrilled that Dr. Mona El-Sheikh has been named the recipient of the 2016-2017 Advancement of Research and Scholarship Achievement Award. Noted for being one of the world’s leading scholars in the area of sleep regulation and its physiological and socio-cultural correlates, Dr. El-Sheikh continues to advance the field with her transdisciplinary lines of creative inquiry, continuous pursuit of excellence, and commitment to mentoring the next generation of scholars,” said Dr. June Henton, dean of the College of Human Sciences.
El-Sheikh, the Leonard Peterson & Company, Inc. Professor in the Department of Human Development and Family Studies, was honored for innovative research that links socio-economic adversity, family risks and well-being, with physical health, sleep processes, and brain function. Supported by the National Institutes of Health and the National Science Foundation among others, El-Sheikh and her colleagues’ groundbreaking work on the role of sleep and sleep problems in child development has expanded to include sleep regulation in adults and adolescents. Her findings help identify and address insufficient sleep as an important public health issue.
“Dr. El-Sheikh is one of Auburn’s most accomplished health science researchers and has earned this recognition through her strong track record of impactful research,” said Dr. John Mason, vice president for research and economic development.
BY LESLIE PARSONS

Dr. Mona El-Sheikh receives Auburn University's 2017 Research and Economic Development Advisory Board Advancement of Research and Scholarship Achievement Award at the board's fall meeting. Also pictured: Dr. John Mason, vice president for research and economic development; Dr. Lori St. Onge, board member; and Charles Pick, board member.
Categories: Health Sciences
Pharmacy faculty, engineering student find common ground in research collaboration
Rusty Arnold, an associate professor in Auburn’s Harrison School of Pharmacy, believes in academic units working together and crossing departmental lines to further research.
That collaboration does not stop at the faculty level as Arnold, a recipient of the President’s Collaborative Units Award, also benefits from the work of undergraduate students such as chemical engineering major Christy Pickering.
Pickering, a senior from Hazel Green, Alabama, was recently awarded a $5,000 Gateway to Research Scholarship from the American Foundation for Pharmaceutical Education for her work in Arnold’s lab, called “Development and Application of Gold‐Lipidic Nanocomposites to Enhance Chemotherapeutic Delivery and Release.” She was one of seven recipients nationally.
The purpose of the scholarship is to support faculty-mentored research in the pharmaceutical sciences. For Pickering, an active student who has been a member of the Auburn University Marching Band the last four years, the funding will assist with tuition and research expenses in her final year at Auburn.
“Christy is very intelligent, extremely motivated and very thorough. What is unique about her is that most of the undergraduate honor students that I work with are pre-med and she is chemical engineering,” said Arnold. “She has a clear vision that she wants to go into research, she wants to go into academia.”
Pickering is in her second year in Arnold’s lab, coming on board shortly after he arrived on campus. For someone who knew she wanted to work in the medical field, it was a perfect match.
“I applied because I thought what Dr. Arnold did sounded really cool – working with cancer, looking at chemo – it just sounded like a project I would really be interested in,” said Pickering. “So I sat down with him and talked about the project, and he took on me and four other undergrads. My project, from the start, was set up to be a very engineering-based pharmaceutical project. It has been a really neat experience getting to work with him.”
For Arnold, Pickering stood out right away as someone who would bring a new approach and think outside of the box in his lab. Bringing on someone with a chemical engineering background has added a new perspective to his research.
“What immediately caught my interest in Christy is when I described some of the challenges with the formulations, she was asking have you tried composites, have you tried these other things. She was immediately thinking about how to solve the problems,” said Arnold. “She has been able to take a system we are working with and propose changes that are actually going to allow us to deliver more than one drug, use more than one imaging modality, and hopefully be able to improve therapy. Using her background in engineering, she is able to add value in an area that my lab did not have expertise in. Even though she is an undergraduate, some of the ideas she has are very different than some of the approaches we would use.”
Part of Pickering’s research is working with liposomes, small spherical particles commonly used for chemotherapeutic delivery because they capitalize on a unique quality of tumors called the enhanced permeability and retention effect, or the EPR Effect. In order for tumors to grow quickly, they stimulate the production of blood vessels, but the quick growth causes them to not be as organized as they are in the rest of the body and the cell wall is more porous.
“The cells aren’t fully connected in some places, which means there are holes that things can transport through,” said Pickering. “The holes are very small, but big enough that liposomes or drugs can pass through into the tumor cells.”
Liposomes, like the ones that Pickering works with in Arnold’s lab, can circulate the body for a long time. When they get to a tumor, holes in the tumor vessels allow the liposomes to pass from the blood into the space outside the blood vessel where the tumor is located.
“We can put these long-circulating liposomes into the body and just let them go through the blood stream until they passively accumulate in the tumor site,” said Pickering. “The treatment called Doxil is a liposome with the chemotherapeutic drug doxorubicin encapsulated within it.
“So, using the EPR Effect is a passive means of targeting a tumor because you are just relying on the liposomes to naturally accumulate there by passing through the blood vessel. What we are trying to do is use active targeting where there will be something on the liposomes that actually targets the cancer cell and not the other cells in the body.”
Specifically, what Pickering has been working on is using the liposomes with the doxorubicin as a treatment method, but also incorporating gold nanoparticles as an imaging contrast agent to be able to look at the tumors.
“If we can put drug and gold nanoparticles in a liposome at the same time and send it to the tumor cell, then we can image the tumor cell at the same time as we are killing the tumor cell, so it gives us combined diagnostic and therapeutic capabilities in one particle,” said Pickering.
“It is an exciting experience to work on a project that has the potential to help people fighting cancer, and I have learned so much though the challenges involved with this research. I am very grateful to Dr. Arnold for the opportunity to work in his lab and to AFPE and the Office of Undergraduate Research for the fellowships that allow me to continue my research.”
By: Matt Crouch
To learn more about the Office of Undergraduate Research, visit: http://www.auburn.edu/undgres/

Categories: Health Sciences
Auburn University hosting forum: Additive Manufacturing – The Next Industrial Revolution
On July 30, 2015, Auburn University will be hosting a by invitation only forum on industrialized additive manufacturing.
Experts will discuss the application of this advanced technology for industries ranging from aerospace to biotechnology. Industry leaders from GE Aviation, GKN, NASA, Carpenter Technology, Alabama Laser, U.S. Army Aviation and faculty from Auburn University, University of Alabama, UAH and University of Memphis will describe the role their organizations are playing in developing, implementing and utilizing new processes and computer-aided hardware and software to produce components from material and composites once considered exotic.
A keynote address will be given by Greg Morris, the General Manager of Additive Technologies for GE Aviation.
To learn more about this day-long forum and networking reception to follow, or if you are interested in attending, please email forum organizers at auees@auburn.edu.

Categories: Health Sciences, Cyber, Energy & the Environment, Science, Technology, Engineering and Mathematics (STEM), Transportation, Food Systems, Engineering
Auburn University celebrates Olympic Training Designation
Elite athletes from across the nation can now train and receive science-based assessments and personalized feedback from kinesiology experts at Auburn.
The College of Education unveiled signage on Sept. 25 marking Auburn University's official designation as a U.S. Olympic training site by the United States Olympic Committee, or USOC, following a ceremony at the School of Kinesiology. Auburn is one of 18 Olympic training sites in the country and one of only five universities nationwide to receive the designation.
The Kinesiology Building, Beard-Eaves-Memorial Coliseum and Watson Fieldhouse were designated U.S. Olympic training sites as the university assists Team USA on its journey to the 2016 Rio de Janiero Olympic Games.
"USA Team Handball is one that competes at the highest level in the Pan American Games and Olympic Games," said retired Brig. Gen. Harvey Schiller, president of USA Team Handball and USOC representative. "I think it's a unique opportunity for the community and the university to have an Olympic sport housed in its environment."
The ceremony, which was hosted in conjunction with the College of Education's centennial anniversary celebration and the Auburn University Board of Trustees' quarterly meeting, included remarks from Jay Gogue, Auburn University president; Betty Lou Whitford, dean of the College of Education; David Benedict, chief operating officer for Auburn University Athletics; Schiller; Sarah Gascon, doctoral candidate in the School of Kinesiology; Sarah Newton, member of the Auburn University Board of Trustees; and Dave Pascoe, a Humana-Germany-Sherman Distinguished Professor and the assistant director of the School of Kinesiology.
Administrators from the university and USA Team Handball, along with several athletes were also honored on Sept. 26 before the Auburn vs. Mississippi State football game.
"This designation brings together the recognizable logos of the USOC, Auburn University and USA Team Handball," said Pascoe. "People across the country will want to connect with this unique collaboration of spirit, science and top training facilities."
Since the summer of 2013, Auburn has hosted elite training and competition for the men's and women's USA national team handball programs.
The USA Team Handball members are also a part of a long-term residency program at Auburn through the School of Kinesiology. This program allows the school to provide expertise in assessment and performance of human movement, including biomechanics, basic and applied physiology, neuroscience, behavior, conditioning, health and motor learning and development.
"The Auburn School of Kinesiology has been instrumental in providing a new home for USA Team Handball athletes and we appreciate the support of the Auburn-Opelika community in welcoming our athletes and coaches," said Alicia McConnell, USOC director of training sites and community partnerships. "We look forward to a fruitful relationship with Auburn University as an official U.S. Olympic training site."
For more information about the United States Olympic Committee, go to www.teamusa.org. For more information about USA Team Handball, go to www.teamusa.org/USA-Team-Handball.
By: Sarah Phillips

Categories: Health Sciences, Auburn In the News
Human pacemaker giving older dogs new ‘leash’ on life at Auburn University
Older dogs with slowing hearts are getting a new "leash" on life at Auburn University's College of Veterinary Medicine, where advanced technology and new treatment protocols have created an emerging cardiology program.
Dr. SeungWoo Jung, assistant professor and clinician in the Cardiology Service of the Wilford and Kate Bailey Small Animal Teaching Hospital, recently placed one of the most advanced pacemaker systems used in humans in Joe, a seven-year-old bulldog owned by Wayne and MaryAnn Swift of Meridian, Mississippi.
Because of the technology and faculty expertise, procedures once considered complicated are now becoming routine.
"Pacemaker implantation is not new to veterinary medicine, having been done for the last 30 years," Jung said. "What is relatively new, and the first one at Auburn, was the use of the same type of pacemaker used in human cases, which we implanted in Joe."
During Joe's recent checkup, tests showed the pacemaker was keeping his heart beating normally. "He's really doing quite well and from this point on, Joe will only need to be seen on a yearly basis," Jung said.
For the Swifts, Joe is a loyal family member, and they had no hesitation to bring him from Mississippi for treatment.
"We were shocked and frightened when they told us what they would have to do," MaryAnn said. "We love that dog dearly, and we know he loves us."
Joe began experiencing fainting episodes and collapsing this past September, and after visits to a Mississippi veterinarian, they determined the next stop was Auburn's College of Veterinary Medicine.
The Swifts were impressed with the treatment and care Joe received, saying, "we cannot praise Auburn enough. They reassured us at all times and kept us informed about what would happen and why. Even if this only gave Joe another two years or so, it would be well worth it."
Pacemakers help monitor and control the heartbeat. A pacemaker will send electrical impulse to the heart to keep the beating rhythm in sync and pumping correctly.
The procedure is similar to the one done in humans. Under anesthesia, a pacemaker wire is threaded through a dog's vessel in the neck to the correct place in the heart. A small incision, made in the back of the shoulder, then allows for insertion of the pacemaker under the skin and connection to the wire.
In the past, Jung said, pacemakers for dogs were older, human models, which only regulated the beating of the heart's bottom chamber. Today's human pacemaker regulates the heart's top and bottom chambers, but because of technical challenges, was not typically used in canine patients.
In the last two years, manufacturers have started donating human pacemakers, or offering them to the veterinary cardiology community at reduced costs. "We are able to offer the device at no additional cost to the owner," Jung said. "Dogs are now able to get the most up-to-date pacemaker on the market."
by Janet McCoy

Categories: Health Sciences
Auburn professor develops cost-effective, staph-resistant bandage
Staph infections affect thousands of people each year, often occurring as a person recovers from surgery or a wound. But an Auburn University professor has developed a better bandage that could keep you from becoming infected.
Professor Emeritus Dave Worley of the Department of Chemistry and Biochemistry in the College of Sciences and Mathematics is applying his patented N-halamine chemistry to gauze bandages to kill any bacteria that might contact a wound.
"A 2-inch-square bandage would cost only 3-4 cents more than a regular bandage," Worley said. "We tested it on Staphylococcus aureus and Pseudomonas aeruginosa. It kills them before they can infect the wound. Once a person becomes infected, the bacteria are hard to kill, especially if they are resistant to antibiotics."
Worley's process works by soaking the gauze in a solution of alcohol and an N-halamine compound containing chlorine. When the alcohol evaporates, the remaining solid, bacteria-killing compound adheres electrostatically to the bandage.
"You can shake the bandage, but the compound won't come out," said Worley, who says current bandages with silver also kill bacteria, but they are costly at up to $500 each. "We are at least as effective as silver at only a fraction of the cost."
Worley's research shows that N-halamine bandages should be kept away from light prior to use. "Our stability is good if you keep the bandages in opaque packages," he said. "Most wound dressings are replaced every one to two days, so ours are effective throughout the time they are worn."
The technology also works for air filters, surgical masks or any other disposable fibrous structure.
Worley's proof-of-concept research was funded by Auburn University's LAUNCH program that helps faculty move research ideas closer to the marketplace. He conducted the research with Professor T.S. Huang of the Department of Poultry Science, College of Agriculture; Professor Emeritus Roy Broughton of the Department of Mechanical Engineering, Samuel Ginn College of Engineering; and postdoctoral fellow Buket Demir of the Department of Chemistry and Biochemistry, College of Sciences and Mathematics.
Auburn's Office of Innovation Advancement and Commercialization has filed a U.S. patent application for the bandages, and is in the process of filing in multiple foreign territories, including Europe and several countries in Asia. The office is also pursuing licensing, including the possibility of forming a start-up company. Worley currently has 40 patents for developing the N-halamine chemistry, which was used to help form the HaloSource company in 1998 for bacteria-killing, rechargeable water filters.
"We are excited about licensing his bandage technology," said Brian Wright, associate director for commercialization. "This technology has application in health care as well as consumer products. The market potential is tremendous, but so is the possible positive impact on public health."
BY CHARLES MARTIN

Categories: Health Sciences
Auburn’s Boshell Diabetes and Metabolic Diseases Program’s 10th annual Research Day March 3
The Boshell Diabetes and Metabolic Diseases Research Program at Auburn University is holding its 10th annual Research Day March 3 at The Hotel at Auburn University and Dixon Conference Center.
The event, which has grown each year, brings together more than 175 researchers from throughout the Unites States for a day of learning and sharing information about research related to diabetes and the role of obesity in its development.
"We have three widely renowned speakers for this year’s event," said organizer Dr. Robert Judd, a professor in the Department of Anatomy, Physiology and Pharmacology at the College of Veterinary Medicine. Judd also serves as chair of the Boshell program at Auburn.
The mission of the program is to enhance the opportunities for diabetes research at Auburn by facilitating cross-disciplinary scientific discussion, supporting the study of new ideas, fostering the development of investigators new to the field of diabetes and expanding the overall base of diabetes investigation at the university, Judd says. Specifically, these investigators are addressing many facets of both types 1 and 2 diabetes, with particular focus on the cardiac, neurological and metabolic aspects of the disease.
"There are more than 45 faculty members here at Auburn who are involved in some form of diabetes-related research," Judd said. "This event gives all of us an opportunity to get together for a day of learning and sharing, and also, it brings colleagues from many other research programs and universities."
This year’s keynote address will be given by Dr. E. Dale Abel, chair of the Department of Internal Medicine at the University of Iowa Carver College of Medicine. Dr. Sabrina Diano, director of the Reproductive Neurosciences Group at the Yale University School of Medicine, is the plenary lecturer and Billy Mills, Olympic gold medalist, is the banquet speaker.
Registration for the Research Day is open through Feb. 24. The event is free for Boshell program members and $125 for nonmembers. Deadline for abstract submission is Feb. 6. Registration and additional information, including an event itinerary and travel and lodging information can be obtained from the Boshell Diabetes and Metabolic Diseases Research Program website, www.auburndiabetes.com.
Speaker bios:
Abel is the chair and departmental executive officer of the Department of Internal Medicine, director of the Fraternal Order of Eagles Diabetes Research Center, director of the Division of Endocrinology and Metabolism in the Department of Internal Medicine at Iowa and head of the Interdisciplinary Diabetes Clinic at Iowa River Landing, University of Iowa Hospitals and Clinics. He is a professor of medicine and biochemistry and currently holds the John B. Stokes III Chair in Diabetes Research. Prior to moving to Iowa, Abel was chief of the Division of Endocrinology, Metabolism and Diabetes and senior investigator in the program in molecular medicine at the University of Utah where he held the H.A. and Edna Benning, Presidential Endowed Chair in Diabetes and Endocrinology.
Diano is a professor in obstetrics, gynecology and reproductive sciences, as well as neuroscience and comparative medicine at Yale. She is also part of the Integrative Cell Signaling and Neurobiology of Metabolism and Interdepartmental Neuroscience Program. She graduated with honors from the University of Naples Federico II, Naples, Italy, and conducted her postdoctoral studies at Yale where she became faculty in 2000.
Mills is the only American to have ever won the Olympic gold medal in the 10,000-meter run. A Lakota Sioux raised in one of the poorest communities in America, the Pine Ridge Indian Reservation in South Dakota, Mills was orphaned as a young boy, facing prejudice and cultural discrimination most of his childhood life. It was through a running scholarship to the University of Kansas that he was able to leave the reservation.
While in college, Mills accepted a commission as an officer in the U.S. Marine Corps, which allowed him to cultivate his winning spirit and rich heritage. He began by running 30 miles a week and eventually worked up to 100 miles every week. Basic training and an excellent track and field program helped Mills qualify for the 1964 Olympics in the 10,000-meter run and the marathon. His victory in the 10,000-meter is often called one of greatest upsets in Olympic history.
BY MITCH EMMONS

Categories: Health Sciences
Research on diabetes and metabolic disease highlight of Boshell Research Day Feb. 26
The ninth annual Boshell Research Day will showcase research in the fields of diabetes and metabolic disease Friday, Feb. 26, at The Hotel at Auburn University and Dixon Conference Center.
The conference brings together experts to present current topics related to diabetes and the role of obesity in its development. It is an annual event of the Boshell Diabetes and Metabolic Disease Research Program at the Auburn University College of Veterinary Medicine and includes more than 40 researchers from across Auburn University.
Speakers and presentations include:
- Keynote speaker Dr. Christopher Newgard, director of the Sarah W. Stedman Nutrition and Metabolism Center at Duke University's School of Medicine.
- A plenary lecture by Dr. Jacqueline Stephens, the Claude B. Pennington Jr. endowed chair in Biomedical Research at the Pennington Biomedical Research Center.
- Distinguished banquet speaker Mick Cornett, mayor of Oklahoma City, Oklahoma. His efforts to address the culture of obesity in his city have resulted in a collective drop of a million pounds by Oklahoma City citizens. Banquet-only tickets can be purchased for $30 per person or $200 for a table of eight. Tickets can be purchased online.
Other highlights of the conference include morning and afternoon oral and poster presentations by experts and researchers.
"Cases of diabetes and obesity have reached epidemic proportions in the United States, and this conference allows investigators from Auburn and other universities the opportunity to get together and discuss significant ongoing research," said Dr. Robert L. Judd, chair of the Boshell program and an associate professor of pharmacology at the College of Veterinary Medicine.
The Boshell Diabetes and Metabolic Disease Research Program was established in 2001 through an endowment by the Birmingham-based Diabetes Trust Fund in honor of founder Dr. Buris R. Boshell. A 1953 graduate of Harvard Medical School, Boshell joined the faculty at the University of Alabama at Birmingham Medical Center in 1959 and became the chief of the Division of Endocrinology and Metabolism in 1963. During this time, he established the Diabetes Research and Education Hospital and the Boshell Diabetes and Endocrine Center in Birmingham.
Online registration is live. Registration is free for Boshell research members and is $100 for non-members. Students and postdoctoral fellows can attend at no cost. To register for the conference and to view a brochure and itinerary, visit www.auburndiabetes.com/researchday.html.
A limited number of rooms are available at The Hotel at Auburn University and Dixon Conference Center. Reservations can be made by calling (800) 228-2876 or (334) 821-8200. Ask for the Boshell Room Block. Transportation from the Atlanta Airport is available through Groome Transportation by calling (334) 821-3399.
For questions about Research Day, email Judd at juddrob@auburn.edu.
By Edward Brown
Categories: Health Sciences, External Engagement
Auburn researchers using ‘awake-dog’ MRI scanning to seek neural marker that would predict a dog’s detection ability
A dog's remarkable nose has helped mankind for ages, from the hunting of game animals to more recently sniffing out explosives and contraband.
However, the field of neuroscience knows very little about how the canine brain works, particularly when it is using the sense of smell. Auburn University researchers are shedding light on this aspect through functional MRI brain scans of awake, non-anesthetized dogs.
"We are the first group in the world to use functional MRI of awake dogs to study how their brains process odorant information," said Assistant Professor Gopikrishna "Gopi" Deshpande of the Department of Electrical and Computer Engineering in the Samuel Ginn College of Engineering.
"This lets us see their brains in action when they are smelling odors. Best of all, the dogs don't have to be anesthetized."
Auburn's College of Veterinary Medicine developed the unique awake-dog training system that Deshpande is using in his research to establish an MRI baseline test, which would determine a dog's ability to become a good detector before it goes through training.
"The dogs are not restrained in any way," said Paul Waggoner, co- director of Canine Performance Sciences in the veterinary college. "We trained them to get up on the scanner; place their head in the correct position; and then remain still while the scanning occurs. We're really the first ones to have dogs scanned in this awake fashion. Previously dogs had to be scanned while anesthetized."
Deshpande's project, "Functional Imaging for Developing Outstanding Service Dogs," is being conducted in collaboration with the iK9 company, the College of Veterinary Medicine and the Department of Psychology in the College of Liberal Arts.
Auburn and iK9 are using a $1 million grant from the Defense Advanced Research Projects Agency, or DARPA, to do the study. iK9, which has an office in the Auburn Research Park, is providing the dogs and training while Auburn researchers conduct the MRI scans at Auburn's Magnetic Resonance Imaging Research Center.
"The dogs are undergoing the awake-dog MRI brain scans before and after they are trained so we can look for baseline neural features that would predict the dogs' future detection performance," Deshpande said. "This would enable us to scan a prospective dog's brain and determine the likelihood of its success."
Forty dogs are undergoing the scans and training during the two-year project.
"After a dog gets its initial scan, we train that dog to be a detection dog," iK9 President Roland Beason said. "After four to six weeks, we scan it again. At two other time points we will again scan the dog."
During the MRI scanning, various odors are presented to the dog's nose, with the idea that researchers can determine a specific neural marker in the brain image—to determine if a dog has the makings of a detector dog.
Current methods of finding and training suitable dogs are time consuming and costly for agencies around the globe.
"If we can pinpoint a specific neural marker on the scan, this could result in tremendous financial savings for the government and private companies since they would not use training resources on unsuitable dogs," said Deshpande, who adds that cost of training a highly specialized detector dog can cost up to $30,000.
The researchers hope their findings will result in a test that can used by agencies nationwide. "Auburn is known around the world for its canine programs," Deshpande said. "We have an excellent team working on this project."
by Charles Martin
Categories: Health Sciences, Security, Engineering
Auburn experts harness the power of genetics to develop cancer treatments for humans and dogs
Experts in the Auburn University Research Initiative in Cancer (AURIC) are pursuing genetic approaches to better understand both the causes of cancer, and ways to treat it using a one-health approach. By working with dogs, which have many of the same cancers as humans, they learn about treating both humans and dogs. In breast cancer, researchers have identified multiple mutations in the dog that mirror mutations in women. These mutations give us an understanding of the pathway that a cell takes when it becomes cancerous. Researchers at Auburn are also using genetics to create new therapies for cancer. In the case of osteosarcoma, they have harnessed a canine virus, engineering it to attack bone cancer cells, in an attempt to treat dogs with this disease. Check out some of their research highlights below.
To learn more, visit: http://www.auriconline.org
Categories: Health Sciences
Experts at Auburn University say biosecurity is crucial tool in battle against avian influenza
While avian influenza has been confirmed in 20 states, Alabama remains free of the disease and Alabama poultry producers are doing all that they can to keep the disease at bay.
A poultry scientist with the Alabama Cooperative Extension System said poultry producers are more vigilant than ever when it comes to sanitation and other biosecurity measures.
"All our Alabama poultry growers have biosecurity measures in place," said Ken Macklin. "Biosecurity measures are the first line of defense against avian influenza and other poultry diseases."
Macklin said that more than 43 million chickens and turkeys have either died from the disease or had to be euthanized because the flock tested positive for a highly contagious form of avian influenza in the first five months of 2015. The most severely impacted states are in the upper Midwest, including Iowa, Minnesota, South Dakota and Wisconsin.
"These cases in commercial poultry operations in the upper Midwest have mostly been linked to a failure of biosecurity," said Macklin. "Growers may have thought they were following biosecurity guidelines fully, but it seems that there were lapses."
Macklin, who is also an associate professor of poultry science at Auburn University, said strong biosecurity measures take many forms.
- Isolating the birds from other animals
- Minimizing access to people and unsanitized equipment
- Keeping the area around the poultry buildings clean and uninviting to wild birds
- Sanitizing the facility between flocks
- Cleaning equipment entering and leaving the farm
- Having an all in, all out policy regarding the placement and removal of the birds
- Disposing properly of bedding material and any mortalities
Joseph Giambrone, an Auburn University professor of poultry science, called the losses to the national poultry industry staggering.
"The losses are in the hundreds of millions of dollars," said Giambrone. "We can expect a reduction of at least 10 percent in egg laying production and a similar drop in turkey production nationally."
Macklin said the potential production loss is why Alabama producers are working hard to keep their flocks free of the disease. According to Auburn University research done in 2012, poultry and egg production and processing contributed more than $15 billion to the state's economy and employed more than 86,000 people.
Giambrone, whose research focuses on viral diseases of poultry, said the disease is spread by migrating water fowl such as ducks and geese.
"This outbreak began in Canada, and water fowl spread it south along the migratory bird flyways," he said. "It was brought into the Midwest by birds using the Mississippi flyway. It has persisted so long there because of the heavy concentration of poultry producers in that region of the country."
Giambrone said ducks and geese shed the virus in fecal material.
"Infected water fowl shed the virus into ponds and lakes as well as onto the land they are grazing."
Macklin said that warmer weather may slow the disease's spread.
"The virus can survive for days, especially if it is in water. In water, the virus can survive up to 100 days with a water temperature of 63 degrees Fahrenheit. But when water temperatures reach the 80s, the virus can survive for less than a month."
He said the virus has a reduced ability to survive on land.
"On land, the virus can survive for 30 days at 40 degrees Fahrenheit and 7 days at 68 degrees Fahrenheit," said Macklin. "Once the outside temperature hits the 80s the virus breaks down in hours."
While warmer weather may halt the disease's progress in the United States, Giambrone emphasized that the disease can return next year.
"Even if we get control of the disease this year, wild water fowl in Alaska and Canada remain carriers of the disease and are a threat to bring it back to the United States when they migrate again next year."
By Maggie Lawrence

Categories: Health Sciences, Energy & the Environment, Food Systems, Security
Auburn University and the University of Massachusetts Medical School team with French Biotech Company to treat neurologic disorder in children
Auburn University and the University of Massachusetts Medical (UMMS) school have partnered with Paris-based biotech firm, Lysogene, in studies related to GM1 glandliosidosis.
GM1 gangliosidosis is a member of a group of about 40 related disorders that result from dysfunction of lysosomal enzymes or related proteins. GM1 is a neurologic condition of children that is typically fatal by two years of age. An inherited disorder, GM1 progressively destroys nerve cells in the brain and spinal cord, and is a neurodegenerative disease much like Parkinson’s or Alzheimer’s. There is no cure or effective treatment available and it affects one in every 100,000 to 200,000 newborns.
For more than 40 years, Scott Richey Research Center (SRRC) in Auburn University’s College of Veterinary Medicine has researched GM1 gangliosidosis in felines, as GM1 also occurs naturally in cats. The goal of SRRC’s GM1 research is to find a cure for feline GM1 and, through research partners, successfully apply similar therapies for application in humans.
One of the most successful experimental treatments found to date is gene therapy, using a non-harmful viral vector (AAV) to produce missing enzymes, in this case beta-galactosidase. In feline trials at SRRC, it has successfully restored beta-galactosidase levels to normal, prevented storage of GM1 ganglioside, and quadrupled the lifespan of GM1 cats as survival benefits continue to increase.
Auburn University, Lysogene, and the UMMS will work together on preclinical studies related to AAV gene therapy. According to a press release from Lysogene, the collaboration will combine Lysogene's outstanding translational and clinic expertise in gene therapy for central nervous system disorders with the unique preclinical expertise and infrastructure of UMMS and with Auburn's ability to design and text innovative AAV-based gene therapy approaches to treatment.
To learn more about this collaboration, visit: http://www.clinicalleader.com/doc/lysogene-university-of-massachusetts-medical-school-and-auburn-university-0001
Click here to learn more about Auburn’s Scott Richey Research Center.
Categories: Health Sciences
Get to know Brian Vaughn, an award-winning Auburn University authority on children and peer-relationships
Parents often find that no matter how much they prepare beforehand or think they know about children, they can learn more from simply watching and living the experience. That bit of advice to parents is based on research by Brian Vaughn, an award-winning Auburn University authority on children and peer-relationships.
Throughout the past decade, Vaughn, a professor of human development and family studies in Auburn’s College of Human Sciences, has conducted research on peer relationships at Auburn’s Harris Early Learning Center in Birmingham.
“I study how children learn to love in their families and how they learn to use the character that’s developed within the context of those early family relationships to accomplish the kinds of goals that they set for themselves as they move out of the family and into social groups,” Vaughn said.
Vaughn is an authority in child development with special emphasis on the social/emotional development of infants and young children. His published research has made important contributions for understanding the development and consequences of social attachments between children and their major caregivers. He has also contributed to the literature of social competence and peer relationships in early childhood.
“Unless you understand how trajectories unfold for the average case, you’re never going to understand the pathway that leads to deviance or problems,” Vaughn said. “If I’m successful in that, then it will be possible to put the atypical in context. I find that uncovering the mystery rather than changing the ways that trajectories move along motivates many people in science.”
Vaughn has discovered that children who enjoy interacting with other children become more socially skilled and socially competent. Most recently, his research has expanded to include the roles that sleep may play in a child’s cognitive and social/emotional development and adaptive functioning for preschool children. He has found that children who receive more sleep tend to develop higher quality social relationships and a larger vocabulary.
Vaughn is a recipient of the Creative Research and Scholarship Award, which was presented to him at the ninth annual Auburn University Faculty Awards ceremony in October. The award recognizes and encourages the individual efforts of Auburn faculty who honor the practice of mentoring undergraduate research and scholarship, and it is meant to highlight significant commitment to undergraduate scholarship and creative work outside the classroom.
Vaughn credits his career success to a personal drive to solve questions. “I’m curious about puzzles and mysteries, and to me the interesting and exciting part about science is finding the solution to a puzzle or demystifying something that people don’t really know about,” he said.
“When I was invited to come to Auburn, the most impressive thing I noticed was the degree of collegiality and support presence in my department and the College of Human Sciences,” said Vaughn, who has been at Auburn since December 1988. “I thought, ‘Yes. This is a place I could complete my career.'”
As a father, Vaughn’s advice for child rearing is “that not everything you learned in textbooks applies to you. Your family situation and your child is going to be unique, and many of the things that are given as advice don’t apply.”
Vaughn said he finds satisfaction in seeing students complete their programs, especially on a graduate level of instruction.
“Watching students who didn’t think they were ready or belonged walk across the stage at graduation gives me a thrill,” he said. “I really do like that. I am happy to talk to any student who really wants to learn about human development at almost any time.”
“I know that I will never stop being curious and never stop finding out things I didn’t already know,” Vaughn said. “I’ve been very fortunate to find interesting things several times. Staying curious and never thinking that you know all you need to know about some phenomenon, I think is the key to creativity.”
by Tori Rivers
To learn more about Brian Vaughn, visit his faculty page or the Auburn Research Blog
Categories: Health Sciences


